Cerebral infarction,also known as anischemic stroke,is the pathologic process that results in an area ofnecrotictissue in the brain (cerebral infarct).[1]In mid to high income countries, a stroke is the main reason for disability among people and the 2nd cause of death.[2]It is caused by disrupted blood supply (ischemia) and restricted oxygen supply (hypoxia). This is most commonly due to a thrombotic occlusion, or an embolic occlusion of major vessels which leads to a cerebral infarct.[3][4]In response to ischemia, the brain degenerates by the process ofliquefactive necrosis.[1]
| Cerebral infarct | |
|---|---|
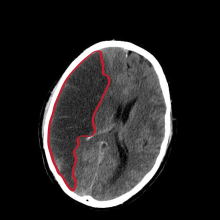 | |
| CT scanslice of the brain showing a right-hemisphericcerebral infarct (left side of image). | |
| Specialty | Neurology |
Classification
editThere are various classification systems[5]for cerebral infarcts, some of which are described below.
- The Oxford Community Stroke Project classification (OCSP, also known as the Bamford or Oxford classification) relies primarily on the initial symptoms. Based on the extent of the symptoms, the stroke episode is classified astotal anterior circulation infarct(TACI),partial anterior circulation infarct(PACI),lacunar infarct(LACI) orposterior circulation infarct(POCI). These four entities predict the extent of the stroke, the area of the brain affected, the underlying cause, and the prognosis.[6][7]
- The TOAST (Trial ofOrg 10172in Acute Stroke Treatment) classification is based on clinical symptoms as well as results of further investigations; on this basis, a stroke is classified as being due to (1) thrombosis or embolism due toatherosclerosisof a large artery, (2) embolism ofcardiacorigin, (3) occlusion of a small blood vessel, (4) other determined cause, (5) undetermined cause (two possible causes, no cause identified, or incomplete investigation).[8]
Stroke recognition
editThere are many tests that can be done to prescreen a patient who may be showing stroke-like symptoms. No one test is better than the other and they all have room for improvement. One of these tests that is used by prehospital personnel is the Cincinnati Pre Hospital Stroke scale (CPSS). This test looks for facial droop, arm drift, and a change in the person's speech pattern. Another test that can be used and is a modification to the CPSS is the Face Arm Speech Test (FAST). This checks for facial weakness, arm weakness, and speech disturbances. The ROSIER (Recognition of Stroke in The ER), is a test used by anER physician.Each variable is rated from a -2 to a +5.Loss of consciousness(-1), convulsive fit (-1), facial weakness (+1), arm weakness (+1), leg weakness (+1), abnormal speech patterns (+1), and visual defect (+1).[9]In recent years, a study has been done to show how AI can aid in diagnosis of cerebral infarct and improve patient outcomes in areas that may not have stroke trained physicians.[10]
Symptoms
editIschemic strokes usually present as a problem with brain orspinal cordfunction. Symptoms typically arise suddenly and may progress within minutes to hours. In rare cases, symtoms may appear gradually over a prolonged period of time, creating diagnostic difficulties.[12]Most strokes occur without warning, but can be preceded by short-lasting stroke symptoms, known as aTransient Ischemic Attack(TIA). Common symptoms include one sided weakness, facialparalysisor numbness, vision problems, trouble speaking, problems with walking and keeping balanced. A person can show one or more of these symptoms during a stroke. Decreased consciousness is more uncommon than in stroke due tointracerebral hemorrhage,but may be present when there is infarctions in more than one part of the brain or in the brain stem.[13]
Symptoms of cerebral infarction can help determine which parts of the brain are affected. If the infarct is located in theprimary motor cortex,contralateral hemiparesis is said to occur. Withbrainstemlocalization, brainstem syndromes are typical:Wallenberg's syndrome,Weber's syndrome,Millard–Gubler syndrome,Benedikt syndromeor others.
Risk factors
editMajor risk factors for cerebral infarction are generally the same as foratherosclerosis.These includehigh blood pressure,diabetes mellitus,tobacco smoking,obesity,anddyslipidemia.[14]There are also risks that a person can't control. These include a person's age, family history of strokes, being African American, and being born a male. A person's risk of a stroke doubles each decade after the age of 55.[15]TheAmerican Heart Association/American Stroke Association(AHA/ASA) recommends controlling these risk factors in order to prevent stroke.[16]The AHA/ASA guidelines also provide information on how to prevent stroke if someone has more specific concerns, such assickle-cell diseaseor pregnancy. It is also possible to calculate the risk of stroke in the next decade based on information gathered through theFramingham Heart Study.[17]
Pathophysiology
editCerebral infarction is caused by a disruption to blood supply that is severe enough and long enough in duration to result in tissue death. The disruption to blood supply can come from many causes, including:
- Thrombosis(obstruction of a blood vessel by a blood clot forming locally)
- Embolism(obstruction due to anembolusfrom elsewhere in the body),[18]
- Systemic hypoperfusion (general decrease in blood supply, e.g., inshock)[19]
- Cerebral venous sinus thrombosis.[20]
- Unusual causes such as gas embolism from rapid ascents in scuba diving.[21]
Even in cases where there is a complete blockage to blood flow of a major blood vessel supplying the brain, there is typically some blood flow to the downstream tissue through collateral blood vessels, and the tissue can typically survive for some length of time that is dependent upon the level of remaining blood flow.[22]If blood flow is reduced enough, oxygen delivery can decrease enough to cause the tissue to undergo theischemic cascade.The ischemic cascade leads to energy failure that prevents neurons from sufficiently moving ions through active transport which leads the neurons to first cease firing, then depolarize leading to ion imbalances that cause fluid inflows and cellular edema, then undergo a complex chain of events that can lead to cell death through one or more pathways.[23][24][25]
Diagnosis
editComputed tomography(CT) andMRIscanning will show damaged area in the brain. A CT scan will rule out ahemorrhagic stroke,is cheaper for the patient, and can be found in almost all hospitals unlike an MRI machine.[26][27]Once the Doctor rules out a hemorrhagic stroke, rTPA can be given.[26]An MRI can help to diagnose an acute cerebral infarct as quickly as 6 hours from start of symptoms,[26]It can also help time when the stroke happened.[28]The biggest problem with an MRI is it can't be done on a patient with certain metallic implants or if the patient isclaustrophobic.[29]A head and neck CT angiogram can be performed within 6 hours of onset of symptoms to see where the occlusion may be located which can help in determining the cause of the stroke.[30]In people who die from a stroke an autopsy can reveal additional diseases or conditions beyond the stroke itself, as well as uncover uncommon causes of a stroke.[31]
Treatment
editIn the last decade, similar to myocardial infarction treatment, thrombolytic drugs were introduced in the therapy of cerebral infarction. The use of intravenousrtPAtherapy can be advocated in patients who arrive to stroke unit and can be fully evaluated within 3 hours of the onset. The quicker rTPA is started, the better the outcome for the patient.[30]
If cerebral infarction is caused by athrombusoccluding blood flow to an artery supplying the brain, definitive therapy is aimed at removing the blockage by breaking the clot down (thrombolysis), or by removing it mechanically (thrombectomy). The more rapidly blood flow is restored to the brain, the fewer brain cells die.[32]In increasing numbers of primary stroke centers, pharmacologic thrombolysis with the drugtissue plasminogen activator(tPA), is used to dissolve the clot and unblock the artery. Giving rTPA lessens the chance of disability after 3 months by 30%.[30]Another intervention for acute cerebral ischemia is removal of the offending thrombus directly. This is accomplished by inserting a catheter into thefemoral artery,directing it into thecerebral circulation,and deploying a corkscrew-like device to ensnare the clot, which is then withdrawn from the body. Mechanical embolectomy devices have been demonstrated effective at restoring blood flow in patients who were unable to receivethrombolytic drugsor for whom the drugs were ineffective,[33][34][35][36]though no differences have been found between newer and older versions of the devices.[37]The devices have only been tested on patients treated with mechanical clot embolectomy within eight hours of the onset of symptoms.
Angioplastyandstentinghave begun to be looked at as possible viable options in treatment of acute cerebral ischaemia. In asystematic reviewof six uncontrolled, single-center trials, involving a total of 300 patients, of intra-cranial stenting in symptomatic intracranial arterial stenosis, the rate of technical success (reduction to stenosis of <50%) ranged from 90 to 98%, and the rate of major peri-procedural complications ranged from 4-10%. The rates of restenosis and/or stroke following the treatment were also favorable.[38]This data suggests that a large,randomized controlled trialis needed to more completely evaluate the possible therapeutic advantage of this treatment.
If studies show carotid stenosis, and the patient has residual function in the affected side,carotid endarterectomy(surgical removal of the stenosis) may decrease the risk of recurrence if performed rapidly after cerebral infarction.Carotid endarterectomyis also indicated to decrease the risk of cerebral infarction for symptomatic carotid stenosis (>70 to 80% reduction in diameter).[39]
In tissue losses that are not immediately fatal, the best course of action is to make every effort to restore impairments throughphysical therapy,cognitive therapy,occupational therapy,speech therapyandexercise.
Permissive hypertension - allowing for higher than normal blood pressures in the acute phase of cerebral infarction - can be used to encourage perfusion to the penumbra.[40]
References
edit- ^abKumar V, Abbas AK, Aster JC, Perkins JA, Robbins SL, Cotran RS (2015).Robbins and Cotran pathologic basis of disease.Student consult (Ninth ed.). Philadelphia, Pa: Elsevier; Saunders.ISBN978-1-4557-2613-4.
- ^Murphy SJ, Werring DJ (September 2020)."Stroke: causes and clinical features".Medicine.48(9):561–566.doi:10.1016/j.mpmed.2020.06.002.PMC7409792.PMID32837228.
- ^Douglas VC, Aminoff MJ (2023). "24-09: Stroke". In Papadakis MA, McPhee SJ, Rabow MW, McQuaid KR (eds.).Current Medical Diagnosis & Treatment 2023.New York, NY: McGraw-Hill Education.Retrieved2024-03-21.
- ^Shin TH, Lee DY, Basith S, Manavalan B, Paik MJ, Rybinnik I, et al. (July 2020)."Metabolome Changes in Cerebral Ischemia".Cells.9(7): 1630.doi:10.3390/cells9071630.PMC7407387.PMID32645907.
- ^Amarenco P, Bogousslavsky J, Caplan LR, Donnan GA, Hennerici MG (2009)."Classification of stroke subtypes".Cerebrovascular Diseases.27(5):493–501.doi:10.1159/000210432.PMID19342825.
- ^Bamford J, Sandercock P, Dennis M, Burn J, Warlow C (June 1991). "Classification and natural history of clinically identifiable subtypes of cerebral infarction".Lancet.337(8756):1521–1526.doi:10.1016/0140-6736(91)93206-O.PMID1675378.S2CID21784682.Later publications distinguish between "syndrome" and "infarct", based on evidence from imaging. "Syndrome" may be replaced by "hemorrhage" if imaging demonstrates a bleed. SeeInternet Stroke Center."Oxford Stroke Scale".Retrieved2008-11-14.
- ^Bamford JM (2000). "The role of the clinical examination in the subclassification of stroke".Cerebrovascular Diseases.10(4):2–4.doi:10.1159/000047582.PMID11070389.S2CID29493084.
- ^Adams HP, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, et al. (January 1993)."Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment".Stroke.24(1):35–41.doi:10.1161/01.STR.24.1.35.PMID7678184.
- ^Chaudhary D, Diaz J, Lu Y, Li J, Abedi V, Zand R (November 2022). "An updated review and meta-analysis of screening tools for stroke in the emergency room and prehospital setting".Journal of the Neurological Sciences.442:120423.doi:10.1016/j.jns.2022.120423.PMID36201961.
- ^Miyamoto N, Ueno Y, Yamashiro K, Hira K, Kijima C, Kitora N, et al. (2023-12-14)."Stroke classification and treatment support system artificial intelligence for usefulness of stroke diagnosis".Frontiers in Neurology.14:1295642.doi:10.3389/fneur.2023.1295642.PMC10753815.PMID38156087.
- ^Kentar M, Mann M, Sahm F, Olivares-Rivera A, Sanchez-Porras R, Zerelles R, et al. (March 2020). "Detection of spreading depolarizations in a middle cerebral artery occlusion model in swine".Acta Neurochirurgica.162(3):581–592.doi:10.1007/s00701-019-04132-8.PMID31940093.S2CID210196036.
- ^Fernandes PM, Whiteley WN, Hart SR, Salman RA (1 February 2013). "Strokes: mimics and chameleons".Practical Neurology.13(1):21–28.doi:10.1136/practneurol-2012-000465.
- ^Lyerly M (2020). "Chapter 24: Stroke & Neurovascular Disorders". In Amthor F, Theibert WA, Standaert DG, Roberson E (eds.).Essentials of Modern Neuroscience.New York, NY: McGraw Hill LLC. p. 7.ISBN978-1-259-86104-8.
- ^Hankey GJ (August 2006)."Potential new risk factors for ischemic stroke: what is their potential?".Stroke.37(8):2181–2188.doi:10.1161/01.STR.0000229883.72010.e4.PMID16809576.
- ^Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, et al. (March 2018). "2018 Guidelines for the Early Management of Patients With Acute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association".Stroke.49(3):e46 –e110.doi:10.1161/STR.0000000000000158.PMID29367334.
- ^Furie KL, Kasner SE, Adams RJ, Albers GW, Bush RL, Fagan SC, et al. (January 2011). "Guidelines for the prevention of stroke in patients with stroke or transient ischemic attack: a guideline for healthcare professionals from the american heart association/american stroke association".Stroke.42(1):227–276.doi:10.1161/STR.0b013e3181f7d043.PMID20966421.
- ^D'Agostino RB, Wolf PA, Belanger AJ, Kannel WB (January 1994)."Stroke risk profile: adjustment for antihypertensive medication. The Framingham Study".Stroke.25(1):40–43.doi:10.1161/01.str.25.1.40.PMID8266381.
- ^Donnan GA, Fisher M, Macleod M, Davis SM (May 2008). "Stroke".Lancet.371(9624):1612–1623.doi:10.1016/S0140-6736(08)60694-7.PMID18468545.S2CID208787942.(subscription required)
- ^Shuaib A, Hachinski VC (September 1991)."Mechanisms and management of stroke in the elderly".CMAJ.145(5):433–443.PMC1335826.PMID1878825.
- ^Stam J (April 2005)."Thrombosis of the cerebral veins and sinuses".The New England Journal of Medicine.352(17):1791–1798.doi:10.1056/NEJMra042354.PMID15858188.S2CID42126852.
- ^Levett DZ, Millar IL (November 2008). "Bubble trouble: a review of diving physiology and disease".Postgraduate Medical Journal.84(997):571–578.doi:10.1136/pgmj.2008.068320.PMID19103814.S2CID1165852.
- ^Vagal A, Aviv R, Sucharew H, Reddy M, Hou Q, Michel P, et al. (September 2018)."Collateral Clock Is More Important Than Time Clock for Tissue Fate".Stroke.49(9):2102–2107.doi:10.1161/STROKEAHA.118.021484.PMC6206882.PMID30354992.
- ^Krnjević K (September 1999)."Early effects of hypoxia on brain cell function".Croatian Medical Journal.40(3):375–380.PMID10411965.
- ^Hartings JA, Shuttleworth CW, Kirov SA, Ayata C, Hinzman JM, Foreman B, et al. (May 2017)."The continuum of spreading depolarizations in acute cortical lesion development: Examining Leão's legacy".Journal of Cerebral Blood Flow and Metabolism.37(5):1571–1594.doi:10.1177/0271678X16654495.PMC5435288.PMID27328690.
- ^Kalogeris T, Baines CP, Krenz M, Korthuis RJ (December 2016)."Ischemia/Reperfusion".Comprehensive Physiology.7(1):113–170.doi:10.1002/cphy.c160006.ISBN978-0-470-65071-4.PMC5648017.PMID28135002.
- ^abcLin MP, Liebeskind DS (October 2016)."Imaging of Ischemic Stroke".Continuum.22(5, Neuroimaging):1399–1423.doi:10.1212/CON.0000000000000376.PMC5898964.PMID27740982.
- ^Hakimi R, Garg A (October 2016). "Imaging of Hemorrhagic Stroke".Continuum.22(5, Neuroimaging):1424–1450.doi:10.1212/CON.0000000000000377.PMID27740983.
- ^White P, Nanapragasam A (April 2018)."What is new in stroke imaging and intervention?".Clinical Medicine.18(Suppl 2):s13 –s16.doi:10.7861/clinmedicine.18-2-s13.PMC6334026.PMID29700087.
- ^Zhang XH, Liang HM (July 2019)."Systematic review with network meta-analysis: Diagnostic values of ultrasonography, computed tomography, and magnetic resonance imaging in patients with ischemic stroke".Medicine.98(30): e16360.doi:10.1097/MD.0000000000016360.PMC6709059.PMID31348236.
- ^abcPapadakis M, McPhee SJ (2024)."Stroke, Cerebral Infarction".Quick Medical Diagnosis & Treatment 2024.New York, NY: McGraw-Hill Education.Retrieved2024-03-25.
- ^Hudák L, Nagy AC, Molnár S, Méhes G, Nagy KE, Oláh L, et al. (June 2022)."Discrepancies between clinical and autopsy findings in patients who had an acute stroke".Stroke and Vascular Neurology.7(3):215–221.doi:10.1136/svn-2021-001030.PMC9240455.PMID35101949.
- ^Saver JL (January 2006)."Time is brain--quantified".Stroke.37(1):263–266.doi:10.1161/01.STR.0000196957.55928.ab.PMID16339467.
- ^Flint AC, Duckwiler GR, Budzik RF, Liebeskind DS, Smith WS (April 2007)."Mechanical thrombectomy of intracranial internal carotid occlusion: pooled results of the MERCI and Multi MERCI Part I trials".Stroke.38(4):1274–1280.doi:10.1161/01.STR.0000260187.33864.a7.PMID17332445.
- ^Smith WS, Sung G, Starkman S, Saver JL, Kidwell CS, Gobin YP, et al. (July 2005)."Safety and efficacy of mechanical embolectomy in acute ischemic stroke: results of the MERCI trial".Stroke.36(7):1432–1438.doi:10.1161/01.STR.0000171066.25248.1d.PMID15961709.
- ^Lutsep HL, Rymer MM, Nesbit GM (2008). "Vertebrobasilar revascularization rates and outcomes in the MERCI and multi-MERCI trials".Journal of Stroke and Cerebrovascular Diseases.17(2):55–57.doi:10.1016/j.jstrokecerebrovasdis.2007.11.003.PMID18346645.
- ^Smith WS (June 1, 2006)."Safety of mechanical thrombectomy and intravenous tissue plasminogen activator in acute ischemic stroke. Results of the multi Mechanical Embolus Removal in Cerebral Ischemia (MERCI) trial, part I".AJNR. American Journal of Neuroradiology.27(6):1177–1182.PMC8133930.PMID16775259.
- ^Smith WS, Sung G, Saver J, Budzik R, Duckwiler G, Liebeskind DS, et al. (April 2008)."Mechanical thrombectomy for acute ischemic stroke: final results of the Multi MERCI trial".Stroke.39(4):1205–1212.doi:10.1161/STROKEAHA.107.497115.PMID18309168.
- ^Derdeyn CP, Chimowitz MI (August 2007)."Angioplasty and stenting for atherosclerotic intracranial stenosis: rationale for a randomized clinical trial".Neuroimaging Clinics of North America.17(3):355–63,viii–ix.doi:10.1016/j.nic.2007.05.001.PMC2040119.PMID17826637.
- ^Ropper AH, Brown RH, eds. (2005).Adams and Victor's Principles of Neurology(8th ed.). McGraw Hill Professional. p. 698.ISBN0-07-141620-X.
- ^Grotta JC, Albers G, Broderick JP, Kasner SE, Lo EH, Mendelow AD, eds. (24 August 2015).Stroke: pathophysiology, diagnosis, and management(Sixth ed.). Elsevier.ISBN978-0-323-29544-4.OCLC919749088.