Lymphatic filariasisis a human disease caused byparasitic wormsknown asfilarial worms.[2][3]Usually acquired in childhood, it is a leading cause of permanent disability worldwide, impacting over a hundred million people and manifesting itself in a variety of severe clinical pathologies[6][7]While most caseshave no symptoms,some people develop a syndrome calledelephantiasis,which is marked by severeswellingin the arms, legs,breasts,orgenitals.The skin may become thicker as well, and the condition may become painful.[2]Affected people are often unable to work and are often shunned or rejected by others because of their disfigurement and disability.[7]
| Lymphatic filariasis | |
|---|---|
| Other names | Elephantiasis tropica,[1]elephantiasis arabum[1] |
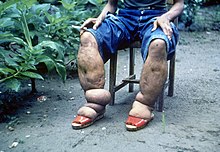 | |
| Elephantiasis of the legs due to filariasis. | |
| Specialty | Infectious diseases |
| Symptoms | None, severe swelling of the arms, legs, breasts, or genitals[2] |
| Causes | Filarial wormsspread bymosquitos[3] |
| Diagnostic method | Microscopic examinationof blood[4] |
| Prevention | Bed nets,mass deworming[2] |
| Medication | Albendazolewithivermectinordiethylcarbamazine[2] |
| Frequency | 40 million (2022)[5] |
It is the first of themosquito-borne diseasesto have been identified.[8]The worms are spread by the bites of infectedmosquitoes.[2]Three types of worms are known to cause the disease:Wuchereria bancrofti,Brugia malayi,andBrugia timori,withWuchereria bancroftibeing the most common.[2]These worms damage the lymphatic system by nesting within the lymphatic vessels and disrupting the system's normal function. Worms can survive within the human body for up to 8 years, all while reproducing millions of larvae which circulate through the blood.[9]The disease is diagnosed bymicroscopic examinationof blood collected during the night. The blood is typically examined as asmearafter being stained withGiemsa stain.Testing the bloodforantibodiesagainst the disease may also permit diagnosis.[4]Otherroundwormsfrom the same family are responsible forriver blindness.[10]
Prevention can be achieved by treating entire groups affected by the disease, known asmass deworming.[2]This is done every year for about six years, to rid a population of the disease entirely.[2]Medicationsusually include a combination of two or moreanthelminticagents:albendazole,ivermectin,anddiethylcarbamazine.[11]Efforts to prevent mosquito bites are also recommended, including reducing the number of mosquitoes and promoting the use ofbed nets.[2]
As of 2022, about 40 million people were infected, and about 863 million people were at risk of the disease in 47 countries.[5]It is most common in tropical Africa and Asia.[2]Lymphatic filariasis is classified as aneglected tropical diseaseand one of the four mainworm infections.[10]The impact of the disease results in economic losses of billions of US dollars a year.[2]
Signs and symptoms
editMost people infected with the worms that cause lymphatic filariasis never develop symptoms;[12]though some have damage tolymph vesselsthat can be detected bymedical ultrasound.[13]Months to years after the initial infection, the worms die, triggering an immune response that manifests with repeated episodes offeverand painful swelling over the nearestlymph nodes(typicallythose along the groin).[12][13]In areas withendemiclymphatic filariasis, people are typically infected in childhood, and symptoms begin in adolescence.[13]
A subset of those affected have continued damage to their lymph vessels. Dysfunctional vessels fail to recirculate lymph fluid, which can pool (calledlymphodema) in the nearest extremity – generally the arm, leg, breast, or scrotum.[13]Loss of lymph function (which transportsimmune cells) results in various repeated infections in the area.[14]Repeated cycles of infection, inflammation, and lymph vessel damage over several years cause the affected extremity to swell to an extremely large size.[15]The surrounding skin thickens, becoming dry, discolored, and dotted with wartlike lumps that contain tortuous loops of lymph vessels.[14]
Even those without lymph damage can sometimes develop an allergic reaction to the worm larvae in thecapillariesof the lung, calledtropical pulmonary eosinophilia.These people develop nocturnalcoughing,fatigue, and weight loss. Over time, this can damage the lungs, resulting inrestrictive lung disease(decreased lung capacity).[16]
Causes
editLymphatic filariasis is caused by infection with three different nematode worms:Wuchereria bancrofti(causes 90% of cases),Brugia malayi,andBrugia timori.[17]The three worms are transmitted by the bite of an infectedmosquito– largely of generaAedes,Anopheles,Culex,orMansonia.When the mosquito bites, infectious nematode larvae are dropped onto the skin. They crawl into the bite wound, through thesubcutaneous tissue,and into nearbylymph vessels.There, they develop into adults over about a year, with adult females up to 10 centimetres (3.9 in) long, and males up to half that length.[18]Adult females and males mate, prompting the female to begin releasing a constant stream of larvae called "microfilariae" – more than 10,000 microfilariae each day for the adult's remaining lifespan of around five to eight years.[18]Microfilariae typically circulate in the blood stream at night; during the day they collect in thecapillariesof the lungs.[18]
A mosquito that feeds on an infected person can take up microfilariae along with itsblood meal.Inside the mosquito, the microfilariae pierce the stomach wall and crawl to the flight muscles, where they mature over 10 to 20 days into their human-infectious form. They then crawl to the mosquito's mouth to be deposited at its next bite, continuing the lifecycle.[18]
The disease itself is a result of a complex interplay between several factors: the worm, theendosymbioticWolbachiabacteria within the worm, the host's immune response, and the numerous opportunistic infections and disorders that arise. The adult worms live in the humanlymphatic systemand obstruct the flow oflymphthroughout the body; this results in chroniclymphedema,most often noted in the lower torso (typically in the legs and genitals).[19]These worms can survive within the human body for up to 8 years, all while reproducing millions of larvae which circulate through the blood.[9]
Diagnosis
editThepreferred methodfor diagnosing lymphatic filariasis is by finding the microfilariae via microscopic examination of the blood. The blood sample is typically in the form of athick smear,stained withGiemsa stain.Technicians analyzing the blood smear must be able to distinguish betweenW. bancroftiand other parasites potentially present. A blood smear is a simple and fairly accurate diagnostic tool, provided the blood sample is taken when the microfilariae are in the peripheral circulation. Because the microfilariae only circulate in the blood at night, the blood specimen must be collected at night.[20]
It is often difficult or impossible to detect the causative organism in the peripheral blood, even in advanced cases.[21]In such cases,testing the blood serumfor antibodies against the disease may also be used.[4]A polymerase chain reaction test can also be performed to detect a minute fraction, as little as 1 pg, of filarial DNA.[22]Dead, calcified worms can be detected by X-ray examinations. Ultrasonography can also be used to detect the movements and noises caused by the movement of adult worms.[23]
Differential diagnosis
editLymphatic filariasis may be confused withpodoconiosis(also known as nonfilarial elephantiasis), a non-infectious disease caused by exposure of bare feet to irritant alkaline clay soils.[24][25]Podoconiosis however typically affects the legs bilaterally, while filariasis is generally unilateral.[24]Also, podoconiosis very rarely affects the groin while filariasis frequently involves the groin. Geographical location may also help to distinguish between these two diseases: podoconiosis is typically found in higher altitude areas with high seasonal rainfall, while filariasis is common in low-lying areas where mosquitos are prevalent.[24]
Prevention
editProtecting against mosquito bites inendemicregions is crucial to the prevention of lymphatic filariasis.Insect repellentsandmosquito nets(especially when treated with an insecticide such asdeltamethrinorpermethrin)[26]have been demonstrated to reduce the transmission of lymphatic filariasis.[27][28]In addition residual spraying and personal protective equipment are known ways to control vectors.[9]
Worldwideeradication of lymphatic filariasisis the definitive goal. This is considered to be achievable since the disease has no known animal reservoir.[27]TheWorld Health Organization(WHO) is coordinating theglobal effort to eradicate filariasis.The mainstay of this program ismass dewormingof entire populations of people who are at risk with antifilarial drugs. The specific treatment depends on the co-endemicity of lymphatic filariasis with other filarial diseases. The WHO's annual MDA guidelines are listed below.
- For areas co-endemic with loiasis 400 mg of albendazole should be administered
- for countries co-endemic with onchocerciasis, 200 mcg/kg of Ivermectin should be administered with 400 mg of albendazole
- in countries without onchocerciasis 6 mg/kg of diethylcarbamazine citrate (DEC) and 400 mg of albendazole should be used
- in countries without onchocerciasis and theIDA Guidelinesare met 200 mcg/kg of ivermectin should be used with 6 mg/kg of diethylcarbamazine and 400 mg of albendazole.[9][11]
Because the parasite requires a human host to reproduce, consistent treatment of at-risk populations (annually for a duration of four to six years)[2]is expected to break the cycle of transmission and cause the extinction of the causative organisms.[27]
In 2011,Sri Lankawas certified by the WHO as having eradicated lymphatic filariasis. In July 2017, the WHO announced that the disease had been eliminated in Tonga. Elimination of the disease has also occurred in Cambodia, China, Cook Islands, Egypt, Kiribati, Maldives, Marshall Islands, Niue, Palau, South Korea, Thailand, Vanuatu, Vietnam, and Wallis and Futuna.[29]In 2020, the WHO announced 2030 targets for this program ofeliminatinglymphatic filariasis in 80% of endemic countries.[30]
Avaccineis not yet available, but in 2013, theUniversity of Illinois College of Medicinewas reporting 95% efficacy in testing againstB. malayiin mice.[31]
Treatment
editTreatment of lymphatic filariasis depends in part on the geographic location of the area of the world in which the disease was acquired but often involves the combination of two or moreanthelminticagents:albendazole,ivermectin,anddiethylcarbamazine.Insub-Saharan Africa,the disease is usually treated with albendazole and ivermectin, whereas in the Western Pacific region, all three anthelmintic agents are used. While diethylcarbamazine in combination with albendazole is often used, it isn't as region-specific as the other combinations. Albendazole monotherapy is used in regions with endemicloiasisin combination with integrated vector control and was the treatment modality for 11.2 million people in 2022.[11]
Wolbachiaareendosymbioticbacteria that live inside the gut of the nematode worms responsible for lymphatic filariasis, and which provide nutrients necessary for their survival.Doxycyclinekills these bacteria, which in turn prevents the maturation of microfilariae into adults. It also shortens the lifespan of the adult worms, causing them to die within 1 to 2 years instead of their normal 10 to 14-year lifespan.[32]Doxycycline is effective in treating lymphatic filariasis. Limitations of thisantibioticprotocol include that it requires 4 to 6 weeks of treatment rather than the single dose of the anthelmintic agents, that doxycycline should not be used in young children and pregnant women, and that it isphototoxic.[33]
Albendazole is classified as an antihelmintics, which specifically works to kill worms.[34]The drug stops the worms from absorbing glucose, evidently leading to starvation and death from fatigue. The effects of albendazole alone have varying results, however, in combination with DEC drugs it has been found more effective.[35]Ivermectin is administered with albendazole, and works by binding to the nerve cells of the parasites, subsequently making them permeable to chloride. This leads to death by paralysis. Ivermectin, however, has been found to only kill the parasites in their early stages of life, and cannot kill an adult, live worm. Therefore, this drug is usually combined with DEC to kill both the microfilariae and the adult worms.[36]
Surgical treatment may be helpful in cases of scrotal elephantiasis andhydrocele.However, surgery is generally ineffective at correcting elephantiasis of the limbs.[37]Acute inflammatory responses due to lymphedema, and hydrocele can be reduced or prevented by practicing good hygiene, skin care, exercise and elevation of infected limbs.[9]
Epidemiology
editLymphatic filariasis occurs in tropical and subtropical regions of Africa, Asia,Central America,theCaribbean,South America, and certain Pacific Island nations. Elephantiasis caused by lymphatic filariasis is one of the most common causes of permanent disability in the world.[7]As of 2018, 51 million people were infected with lymphatic filariasis and at least 863 million people in 50 countries were living in areas that require preventive chemotherapy to stop the spread of infection. By 2022, the prevalence had declined to somewhere around 40 million and the disease remainsendemicin 47 countries. These improvements are a direct result of the WHO'sGlobal Programme to Eliminate Lymphatic Filariasis.[5]Since implementation, 740 million people no longer require preventative chemotherapy to treat the disease.[9]
W. bancroftiis responsible for 90% of lymphatic filariasis.Brugia malayicauses most of the remainder of the cases, whileBrugia timoriis a rare cause.[5]W. bancroftilargely affects areas across the broad equatorial belt (Africa, the Nile Delta, Turkey, India, the East Indies, Southeast Asia, Philippines, Oceanic Islands, and parts of South America). Since lymphatic filariasis requires multiple mosquito bites over several months to years to spread of infection due to tourism is low.[38]The mosquito vectors ofW. bancroftihave a preference for human blood; humans are the only animals naturally infected withW. bancrofti.No reservoir host is known.[39]Lymphatic Filariasis is extremely uncommon in the United States, with only one reported case found in South Carolina in the early 1900s.[7]
In South America, four endemic countries have been working to beset lymphatic filariasis, consisting of Brazil, the Dominican Republic, Guyana, and Haiti.[40]In Latin America, the spread of lymphatic filariasis is throughW. bancrofti,the only anthropods within the region,Culex quinquefasciatus.[41]The exponential rate of development within the Americas is being combated through the development of an MDA program. MDA program, a 3-step drug administering program, has led to a 67% decrease in the need for the drug program.[40]Brazil targeted the rising endemic by administering DEC drugs through an MDA program to the communities hit hardest by the disease. By providing these drugs annually, as well as offering post-care, through showing family members how to treat the disease, creating connections for jobs, as well as providing a social network to incorporate patients into society, Brazil has made the most effort to provide care.[42]Dominican Republic has administered 5 rounds of DEC drugs annually for five years, spanning from 2002-2007. After the initial drastic action, the Dominican then administered another three rounds of MDA. Guyana also used DEC drugs to focus on preventing the spread of the disease, using a DEC-fortified salt from 2003-2007 and ultimately switching to MDA with DEC from 2014 to the present. Targeting patient education and access to treatment.[43]Haiti then focused on the disease by implementing DEC drug in 2002. It reached full geographical coverage by 2012, subsequently in 2014 about 20 communities had eradicated the need for MDA.
In communities where lymphatic filariasis is endemic, as many as 10% of women can be affected by swollen limbs, and 50% of men can develop mutilating genital symptoms.[44]
History
editThere is evidence of Lymphatic filariasis cases dating back 4000 years.[45]The ancient Vedic text, theRig Veda,composed around 1500 BC–1200 BC, makes a possible reference to elephantiasis. The 50th hymn of the7th bookof the Rigveda calls on the godsMitra,Varuna,andAgnifor protection against "that which nests inside and swells". The author of the hymn implores the deities to not let the worm wound his foot. The disease is described as causing eruptions to appear on the ankles and the knees.[46]Artifacts from ancient Egypt (2000 BC) and theNok civilizationin West Africa (500 BC) show possible elephantiasis symptoms. The first clear reference to the disease occurs in ancient Greek literature, wherein scholars differentiated the often similar symptoms of lymphatic filariasis from those ofleprosy,describing leprosy aselephantiasis graecorumand lymphatic filariasis aselephantiasis arabum.[45]
The first documentation of symptoms occurred in the 16th century, whenJan Huyghen van Linschotenwrote about the disease during the exploration ofGoa.Similar symptoms were reported by subsequent explorers in areas of Asia and Africa, though an understanding of the disease did not begin to develop until centuries later.[citation needed]
The causative agents were first identified in the late 19th century.[47]In 1866,Timothy Lewis,building on the work ofJean Nicolas DemarquayandOtto Henry Wucherer,made the connection between microfilariae and elephantiasis, establishing the course of research that would ultimately explain the disease. In 1876,Joseph Bancroftdiscovered the adult form of the worm.[48]In 1877, the lifecycle involving an arthropod vector was theorized byPatrick Manson,who proceeded to demonstrate the presence of the worms in mosquitoes. Manson incorrectly hypothesized that the disease was transmitted through skin contact with water in which the mosquitoes had laid eggs.[49]In 1900,George Carmichael Lowdetermined the actual transmission method by discovering the presence of the worm in the proboscis of the mosquito vector.[45]
Many people inMalabar,Nayars as well as Brahmans and their wives – in fact about a quarter or a fifth of the total population, including the people of the lowest castes – have very large legs, swollen to a great size; and they die of this, and it is an ugly thing to see. They say that this is due to the water through which they go, because the country is marshy. This is calledpericaesin the native language, and all the swelling is the same from the knees downward, and they have no pain, nor do they take any notice of this infirmity.
— Portuguese diplomatTomé Pires,Suma Oriental,1512–1515.[50]
Research directions
editResearchers at theUniversity of Illinois at Chicago(UIC) have developed a novel vaccine for the prevention of lymphatic filariasis. This vaccine has been shown to elicit strong, protective immune responses inmousemodels of lymphatic filariasis infection. The immune response elicited by this vaccine has been demonstrated to be protective against bothW. bancroftiandB. malayiinfection in the mouse model and may prove useful in the human.[51]
On 20 September 2007,geneticistspublished the first draft of the completegenome(geneticcontent) ofBrugia malayi,one of the roundworms that causes lymphatic filariasis.[52]This project had been started in 1994 and by 2000, 80% of the genome had been determined. Determining the content of the genes might lead to thedevelopmentof new drugs and vaccines.[53]
Veterinary disease
editOnchocerca ochengicauses lymphatic filariasis incattle.[54][55]
References
edit- ^abJames WD, Berger T, Elston D (2015).Andrews' Diseases of the Skin: Clinical Dermatology.Elsevier Health Sciences. p. 432.ISBN9780323319690.Archivedfrom the original on 12 October 2016.
- ^abcdefghijklm"Lymphatic filariasis Fact sheet N°102".World Health Organization.March 2014.Archivedfrom the original on 25 March 2014.Retrieved20 March2014.
- ^ab"Lymphatic filariasis".World Health Organization.Retrieved7 May2016.
- ^abc"Parasites – Lymphatic Filariasis Diagnosis".CDC.14 June 2013.Archivedfrom the original on 22 February 2014.Retrieved21 March2014.
- ^abcd"Lymphatic filariasis".who.int.Retrieved4 October2019.
- ^Chakraborty, Sanjukta; Gurusamy, Manokaran; Zawieja, David C.; Muthuchamy, Mariappan (July 2013)."Lymphatic filariasis: Perspectives on lymphatic remodeling and contractile dysfunction in filarial disease pathogenesis".Microcirculation.20(5):349–364.doi:10.1111/micc.12031.ISSN1073-9688.PMC3613430.PMID23237232.
- ^abcdCenters for Disease Control and Prevention(22 October 2018)."Lymphatic Filariasis".Parasites.Retrieved10 December2022.
- ^"Lymphatic filariasis".Health Topics A to Z.World Health Organization.Retrieved25 September2011.
- ^abcdef"Lymphatic filariasis".who.int.Retrieved17 November2023.
- ^ab"Working to overcome the global impact of neglected tropical diseases – Summary"(PDF).Relevé Épidémiologique Hebdomadaire.86(13):113–20. March 2011.PMID21438440.
- ^abc"Global programme to eliminate lymphatic filariasis: progress report, 2022".Weekly epidemiological record/Relevé épidémiologique hebdomadaire.Vol. 98, no. 41. World Health Organization. 13 October 2023. pp.489–502.Retrieved11 December2024.
- ^ab"About Lymphatic Filariasis".U.S. Centers for Disease Control and Prevention. 13 May 2024.Retrieved21 May2024.
- ^abcdDespommier et al. 2019,p. 258.
- ^abLourens & Ferrell 2019,"Disease Progression and Symptoms".
- ^Hotez 2022,p. 60.
- ^Despommier et al. 2019,p. 259.
- ^"Lymphatic filariasis".World Health Organization. 1 June 2023.Retrieved18 May2024.
- ^abcdDespommier et al. 2019,p. 256.
- ^Saladin K (2007).Anatomy & Physiology: The Unity of Form and Function.McGraw-Hill.ISBN978-0-07-287506-5.
- ^van Hoegaerden M, Ivanoff B (1986). "A rapid, simple method for isolation of viable microfilariae".Am J Trop Med Hyg.35(1):148–51.doi:10.4269/ajtmh.1986.35.148.PMID3456213.
- ^Pfarr KM, Debrah AY, Specht S, Hoerauf A (November 2009)."Filariasis and lymphoedema".Parasite Immunology.31(11):664–72.doi:10.1111/j.1365-3024.2009.01133.x.PMC2784903.PMID19825106.
- ^Zhong M, McCarthy J, Bierwert L, Lizotte-Waniewski M, Chanteau S, Nutman TB, Ottesen EA, Williams SA (1996). "A polymerase chain reaction assay for detection of the parasiteWuchereria bancroftiin human blood samples ".Am J Trop Med Hyg.54(4):357–63.doi:10.4269/ajtmh.1996.54.357.PMID8615447.
- ^Amaral F, Dryer G, Figueredo-Silva J, Noroes J, Cavalcanti A, Samico SC, Santos A, Coutinho A (1994). "Live adult worms detected by ultrasonography in human Bancroftian filariasis".Am J Trop Med Hyg.50(6):753–7.doi:10.4269/ajtmh.1994.50.753.PMID8024070.
- ^abcKorevaar DA, Visser BJ (2012)."Podoconiosis, a neglected tropical disease".The Netherlands Journal of Medicine.70(5):210–14.PMID22744921.
- ^Davey G, Tekola F, Newport MJ (2007). "Podoconiosis: non-infectious geochemical elephantiasis".Transactions of the Royal Society of Tropical Medicine and Hygiene.101(12):1175–80.doi:10.1016/j.trstmh.2007.08.013.PMID17976670.
- ^Swales, Jay (2006)."Malaria: Fever Wars".CDC.
- ^abcThe Carter Center."Lymphatic Filariasis Elimination Program"(PDF).Retrieved28 November2015.
- ^U.S. Centers for Disease Control and Prevention."Lymphatic".Retrieved8 July2010.
- ^World Health Organization (31 July 2017)."Congratulations, Tonga! Pacific island state eliminates lymphatic filariasis as a public health problem".Retrieved10 December2022.
- ^World Health Organization(29 October 2020)."Lymphatic filariasis: reporting continued progress towards elimination as a public health problem".News.World Health Organization.Retrieved10 December2022.
- ^Dakshinamoorthy G, Samykutty AK, Munirathinam G, Reddy MV, Kalyanasundaram R (March 2013)."Multivalent fusion protein vaccine for lymphatic filariasis".Vaccine.31(12):1616–22.doi:10.1016/j.vaccine.2012.09.055.PMC3554871.PMID23036503.
- ^Landmann F, Voronin D, Sullivan W, Taylor MJ (November 2011)."Anti-filarial activity of antibiotic therapy is due to extensive apoptosis after Wolbachia depletion from filarial nematodes".PLOS Pathogens.7(11): e1002351.doi:10.1371/journal.ppat.1002351.PMC3207916.PMID22072969.
- ^Taylor MJ, Hoerauf A, Townson S, Slatko BE, Ward SA (2014)."Anti-Wolbachia drug discovery and development: safe macrofilaricides for onchocerciasis and lymphatic filariasis".Parasitology.141(1):119–27.doi:10.1017/s0031182013001108.PMC3884836.PMID23866958.
- ^Prevention, CDC-Centers for Disease Control and (26 October 2020)."CDC - Lymphatic Filariasis - Resources for Health Professionals - Guidance for Evaluation and Treatment".cdc.gov.Retrieved12 December2023.
- ^"Lymphatic filariasis".who.int.Retrieved12 December2023.
- ^Brown, K. R.; Ricci, F. M.; Ottesen, E. A. (2000)."Ivermectin: effectiveness in lymphatic filariasis".Parasitology.121 Suppl: S133–146.doi:10.1017/s0031182000006570.ISSN0031-1820.PMID11386685.S2CID19933533.
- ^Gloviczki P (1995). "The management of lymphatic disorders". In Rutherford RB (ed.).Vascular surgery(4th ed.). Philadelphia: WB Saunders. pp.1883–1945.
- ^Prevention, CDC-Centers for Disease Control and (26 August 2021)."CDC - Lymphatic Filariasis - Epidemiology & Risk Factors".cdc.gov.Retrieved20 November2023.
- ^King CL, Freedman DP (2000). "Filariasis". In G.T. Strickland (ed.).Hunter's tropical medicine and emerging infectious diseases(8th ed.). Philadelphia: E.B. Saunders. pp.740–53.ISBN978-0-7216-6223-7.
- ^abFontes, Gilberto; da Rocha, Eliana Maria Mauricio; Scholte, Ronaldo Guilherme Carvalho; Nicholls, Rubén Santiago (22 December 2020)."Progress towards elimination of lymphatic filariasis in the Americas region".International Health.13(Suppl 1):S33 –S38.doi:10.1093/inthealth/ihaa048.ISSN1876-3405.PMC7753170.PMID33349876.
- ^Fontes, G.; Rocha, E. M.; Brito, A. C.; Fireman, F. A.; Antunes, C. M. (June 2000)."The microfilarial periodicity of Wuchereria bancrofti in north-eastern Brazil".Annals of Tropical Medicine and Parasitology.94(4):373–379.doi:10.1080/00034983.2000.11813552.ISSN0003-4983.PMID10945047.S2CID9316265.
- ^Fontes, Gilberto; Leite, Anderson Brandão; de Lima, Ana Rachel Vasconcelos; Freitas, Helen; Ehrenberg, John Patrick; da Rocha, Eliana Maria Mauricio (26 November 2012)."Lymphatic filariasis in Brazil: epidemiological situation and outlook for elimination".Parasites & Vectors.5:272.doi:10.1186/1756-3305-5-272.ISSN1756-3305.PMC3545725.PMID23181663.
- ^McPherson, T (24 January 2003)."Impact on the quality of life of lymphoedema patients following introduction of a hygiene and skin care regimen in a Guyanese community endemic for lymphatic filariasis: A preliminary clinical intervention study".Filaria Journal.2(1): 1.doi:10.1186/1475-2883-2-1.ISSN1475-2883.PMC149435.PMID12605723.
- ^The Carter Center."Lymphatic Filariasis Elimination Program".Retrieved17 July2008.
- ^abc"Lymphatic Filariasis Discovery".Retrieved21 November2008.
- ^"HYMN L. Various Deities".
- ^Otsuji, Y. (2011)."History, Epidemiology and Control of Filariasis".Tropical Medicine and Health.39(1 Suppl 2):3–13.doi:10.2149/tmh.39-1-suppl_2-3(inactive 1 November 2024).PMC3153148.PMID22028595.
{{cite journal}}:CS1 maint: DOI inactive as of November 2024 (link) - ^Grove, David I (1990).A history of human helminthology.Wallingford: CAB International. pp.1–848.ISBN0-85198-689-7.
- ^Grove, David I (2014).Tapeworms, lice and prions: a compendium of unpleasant infections.Oxford: Oxford University Press. pp.1–602.ISBN978-0-19-964102-4.
- ^ Burma D.P. (2010).Project Of History Of Science, Philosophy And Culture In Indian Civilization, Volume Xiii Part 2: From Physiology And Chemistry To Biochemistry.Pearson Education India. p. 49.ISBN978-81-317-3220-5.
- ^Dakshinamoorthy G, Samykutty AK, Munirathinam G, Reddy MV, Kalyanasundaram R (March 2013)."Multivalent fusion protein vaccine for lymphatic filariasis".Vaccine.31(12):1616–22.doi:10.1016/j.vaccine.2012.09.055.PMC3554871.PMID23036503.(primary source)
- ^Ghedin E, Wang S, Spiro D, Caler E, Zhao Q, Crabtree J, et al. (September 2007)."Draft genome of the filarial nematode parasite Brugia malayi".Science.317(5845):1756–60.Bibcode:2007Sci...317.1756G.doi:10.1126/science.1145406.PMC2613796.PMID17885136.
- ^Williams SA, Lizotte-Waniewski MR, Foster J, Guiliano D, Daub J, Scott AL, Slatko B, Blaxter ML (April 2000). "The filarial genome project: analysis of the nuclear, mitochondrial and endosymbiont genomes of Brugia malayi".International Journal for Parasitology.30(4):411–19.doi:10.1016/s0020-7519(00)00014-x.PMID10731564.
- ^Bain, Odile (2002). "Evolutionary Relationships Among Filarial Nematodes".World Class Parasites.Vol. 5.Boston:Kluwer.pp.21–9.doi:10.1007/0-306-47661-4_3.ISBN1-4020-7038-1.ISBN978-1-4020-7038-9.ISBN978-1-4757-7600-3.ISBN978-0-306-47661-7.
- ^Taylor, Mark J.; Bandi, Claudio; Hoerauf, Achim (2005). "WolbachiaBacterial Endosymbionts of Filarial Nematodes ".Advances in Parasitology.Vol. 60.Elsevier.pp.245–84.doi:10.1016/s0065-308x(05)60004-8.ISBN9780120317608.ISSN0065-308X.PMID16230105.S2CID39363217.
Works cited
edit- Despommier DD, Griffin DO, Gwadz RW, Hotez PJ, Knirsch CA (2019). "22. Lymphatic Filariae".Parasitic Diseases(PDF)(7 ed.). Parasites Without Borders. pp.253–264.Retrieved18 May2024.
- Hotez PJ (2022). "4. Elephantiasis: Lymphatic filariasis, endemic nonfilarial elephantiasis (podoconiosis), and dracunculiasis (Guinea worm)".Forgotten People, Forgotten Diseases: The Neglected Tropical Diseases and Their Impact on Global Health and Development(3 ed.). John Wiley & Sons.ISBN9781683673897.
- Lourens GB, Ferrell DK (June 2019). "Lymphatic Filariasis".Nurs Clin North Am.54(2):181–192.doi:10.1016/j.cnur.2019.02.007.PMID31027660.