Inguinal hernia
| Inguinal hernia | |
|---|---|
 | |
| Diagram of anindirect,scrotalinguinal hernia (medianview from the left). | |
| Pronunciation | |
| Specialty | General surgery |
| Symptoms | Pain, bulging in thegroin[1] |
| Complications | Strangulation[1] |
| Usual onset | < 1 year old, > 50 years old[2] |
| Risk factors | Family history,smoking,chronic obstructive pulmonary disease,obesity,pregnancy,peritoneal dialysis,collagen vascular disease,connective tissue disease, previous openappendectomy[1][2][3] |
| Diagnostic method | Based on symptoms,medical imaging[1] |
| Treatment | Conservative,surgery[1] |
| Frequency | 27% (males), 3% (females)[1] |
| Deaths | 59,800 (2015)[4] |
Aninguinal herniaorgroin herniais ahernia(protrusion) ofabdominal cavitycontents through theinguinal canal.Symptoms, which may include pain or discomfort especially with or following coughing, exercise, orbowel movements,are absent in about a third of patients. Symptoms often get worse throughout the day and improve when lying down. A bulging area may occur that becomes larger when bearing down. Inguinal hernias occur more often on the right than left side. The main concern is strangulation, where theblood supplyto part of theintestineis blocked. This usually produces severe pain and tenderness of the area.[1]
Risk factors for the development of a hernia include:smoking,chronic obstructive pulmonary disease,obesity,pregnancy,peritoneal dialysis,collagen vascular disease,and previous openappendectomy,among others.[1][2]Predisposition to hernias isgenetic[5]and they occur more often in certain families.[6][7][8][1]Deleterious mutationscausing predisposition to hernias seem to havedominantinheritance (especially for men). It is unclear if inguinal hernias are associated with heavy lifting. Hernias can often be diagnosed based on signs and symptoms. Occasionallymedical imagingis used to confirm the diagnosis or rule out other possible causes.[1]
Groin hernias that do not cause symptoms in males do not need to be repaired. Repair, however, is generally recommended in females due to the higher rate offemoral hernias(also a type of groin hernia) which have more complications. If strangulation occursimmediate surgeryis required. Repair may be done by open surgery or bylaparoscopic surgery.Open surgery has the benefit of possibly being done underlocal anesthesiarather thangeneral anesthesia.Laparoscopic surgery generally has less pain following the procedure.[1][9]
In 2015 inguinal, femoral and abdominal hernias affected about 18.5 million people.[10]About 27% of males and 3% of females develop a groin hernia at some time in their life.[1]Groin hernias occur most often before the age of one and after the age of fifty.[2]Globally, inguinal, femoral and abdominal hernias resulted in 60,000 deaths in 2015 and 55,000 in 1990.[4][11]
Signs and symptoms[edit]
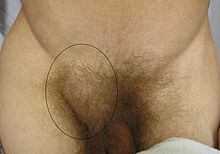
Hernias usually present as bulges in the groin area that can become more prominent when coughing, straining, or standing up. The bulge commonly disappears on lying down. Mild discomfort can develop over time. The inability to "reduce", or place the bulge back into the abdomen usually means the hernia is 'incarcerated' which requires emergency surgery.
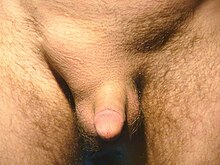
As the hernia progresses, contents of the abdominal cavity, such as the intestines, can descend into the hernia and run the risk of being pinched within the hernia, causing anintestinal obstruction.Significant pain at the hernia site is suggestive of a more severe course, such as incarceration (the hernia cannot be reduced back into the abdomen) and subsequent ischemia and strangulation (when the hernia becomes deprived of blood supply).[12]If the blood supply of the portion of the intestine caught in the hernia is compromised, the hernia is deemed "strangulated" and gutischemiaandgangrenecan result, with potentially fatal consequences. The timing of complications is not predictable.
Pathophysiology[edit]
In males, indirect hernias follow the same route as the descendingtestes,which migrate from theabdomeninto the scrotum during thedevelopment of the urinary and reproductive organs.The larger size of theiringuinal canal,which transmitted the testicle and accommodates the structures of thespermatic cord,might be one reason why men are 25 times more likely to have an inguinal hernia than women. Although several mechanisms such as strength of the posterior wall of the inguinal canal and shutter mechanisms compensating for raised intra-abdominal pressure prevent hernia formation in normal individuals, the exact importance of each factor is still under debate. The physiological school of thought thinks that the risk of hernia is due to aphysiologicaldifference between patients who develop a hernia and those who do not, namely the presence of aponeurotic extensions from the transversus abdominis aponeurotic arch.[13]
Inguinal hernias mostly containthe omentumor a part of thesmall intestines,however, some unusual contents may be anappendicitis,diverticulitis,colon cancer,urinary bladder,ovaries,and rarely malignant lesions.[14]
-
Illustration of an inguinal hernia.
-
Different types of inguinal hernias.
-
Inguinal fossae
Diagnosis[edit]



There are two types of inguinalhernia,directandindirect,which are defined by their relationship to theinferior epigastric vessels.Direct inguinal herniasoccur medial to the inferior epigastric vessels when abdominal contents herniate through a weak spot in the fascia of the posterior wall of the inguinal canal, which is formed by thetransversalis fascia.Indirect inguinal herniasoccur when abdominal contents protrude through thedeep inguinal ring,lateral to the inferior epigastric vessels; this may be caused by failure of embryonic closure of theprocessus vaginalis.
In the case of the female, the opening of thesuperficial inguinal ringis smaller than that of the male. As a result, the possibility for hernias through the inguinal canal in males is much greater because they have a larger opening and therefore a much weaker wall through which the intestines may protrude.
| Type | Description | Relationship toinferior epigastric vessels | Covered byinternal spermatic fascia? | Usual onset |
|---|---|---|---|---|
| Direct inguinal hernia | Enters through a weak point in the fascia of the abdominal wall (Hesselbach triangle) | Medial | No | Adult |
| Indirect inguinal hernia | Protrudes through the inguinal ring and is ultimately the result of theprocessus vaginalisfailing to close after thetesticle's passageduring the embryonic stage | Lateral | Yes | Congenital / Adult |
Inguinal hernias, in turn, belong to groin hernias, which also includesfemoral hernias.A femoral hernia is not via the inguinal canal, but via thefemoral canal,which normally allows passage of the commonfemoral arteryand vein from the pelvis to the leg.
InAmyand's hernia,the content of the hernial sac is theappendix.
InLittre's hernia,the content of the hernial sac contains aMeckel's diverticulum.
Clinical classification of hernia is also important according to which hernia is classified into
- Reducible hernia: is one which can be pushed back into the abdomen by putting manual pressure to it.
- Irreducible/Incarcerated hernia: is one which cannot be pushed back into the abdomen by applying manual pressure.
Irreducible hernias are further classified into
- Obstructed hernia: is one in which the lumen of the herniated part of intestine is obstructed.
- Strangulated hernia: is one in which the blood supply of the hernia contents is cut off, thus, leading to ischemia. The lumen of the intestine may be patent or not.
Direct inguinal hernia[edit]
The direct inguinal hernia enters through a weak point in thefasciaof theabdominal wall,and its sac is noted to be medial to theinferior epigastric vessels.Direct inguinal hernias may occur in males or females, but males are ten times more likely to get a direct inguinal hernia.[15]
A direct inguinal hernia protrudes through a weakened area in thetransversalis fascianear themedial inguinal fossawithin an anatomic region known as the inguinal orHesselbach's triangle,an area defined by the edge of therectus abdominis muscle,theinguinal ligamentand the inferior epigastric artery. These hernias are capable of exiting via thesuperficial inguinal ringand are unable to extend into thescrotum.
When a patient develops a simultaneous direct andindirect herniaon the same side, it is called apantaloon herniaorsaddlebag herniabecause it resembles a pair of pants with the epigastric vessels in the crotch, and the defects can be repaired separately or together. Another term for pantaloon hernia isRomberg's hernia.
Since the abdominal walls weaken with age, direct hernias tend to occur in the middle-aged and elderly. This is in contrast to indirect hernias which can occur at any age including the young, since their etiology includes a congenital component where the inguinal canal is left more patent (compared to individuals less susceptible to indirect hernias).[16][17]Additional risk factors include chronic constipation, being overweight or obese, chronic cough, family history and prior episodes of direct inguinal hernias.[15]
Indirect inguinal hernia[edit]

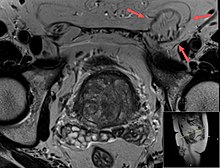
Anindirect inguinal herniaresults from the failure of embryonic closure of thedeep inguinal ring.In the male it can occur after thetesticlehas passed through the deep inguinal ring. It is the most common cause of groin hernia. Adouble indirect inguinal herniahas two sacs.
In the male fetus, theperitoneumgives a coat to the testicle as it passes through this ring, forming a temporary connection called theprocessus vaginalis.In normal development, the processus is obliterated once the testicle is completely descended. The permanent coat of peritoneum that remains around the testicle is called thetunica vaginalis.The testicle remains connected to its blood vessels and the vas deferens, which make up thespermatic cordand descend through the inguinal canal to the scrotum.
The deep inguinal ring, which is the beginning of the inguinal canal, remains as an opening in the fascia transversalis, which forms the fascial inner wall of the spermatic cord. When the opening is larger than necessary for passage of the spermatic cord, the stage is set for an indirect inguinal hernia. The protrusion of peritoneum through theinternal inguinal ringcan be considered an incomplete obliteration of the processus.
In an indirect inguinal hernia, the protrusion passes through the deep inguinal ring and is located lateral to the inferior epigastric artery. Hence, the conjoint tendon is not weakened.
There are three main types
- Bubonocele: in this case the hernia is limited in inguinal canal.
- Funicular: here the processus vaginalis is closed at its lower end just above the epididymis. The content of the hernial sac can be felt separately from the testis which lies below the hernia.
- Complete (or scrotal): here the processus vaginalis is patent throughout. The hernial sac is continuous with the tunica vaginalis of the testis. The hernia descends down to the bottom of the scrotum and it is difficult to differentiate the testis from hernia.
In the female, groin hernias are only 4% as common as in males.Indirect inguinal herniais still the most common groin hernia for females. If a woman has an indirect inguinal hernia, her internal inguinal ring is patent, which is abnormal for females. The protrusion of peritoneum is not called "processus vaginalis" in women, as this structure is related to the migration of the testicle to the scrotum. It is simply a hernia sac. The eventual destination of the hernia contents for a woman is thelabium majuson the same side, and hernias can enlarge one labium dramatically if they are allowed to progress.[citation needed]
Medical imaging[edit]
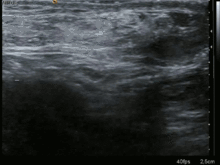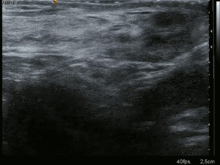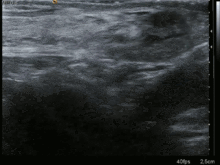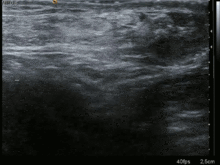
A physician may diagnose an inguinal hernia, as well as the type, frommedical historyandphysical examination.[20]For confirmation or in uncertain cases,medical ultrasonographyis the first choice of imaging, because it can both detect the hernia and evaluate its changes with for example pressure, standing andValsalva maneuver.[21]
When assessed byultrasoundor cross sectional imaging withCTorMRI,the major differential in diagnosing indirect inguinal hernias is differentiation fromspermatic cordlipomas,as both can contain only fat and extend along the inguinal canal into the scrotum.[22]
On axialCT,lipomas originate inferior or lateral to the cord, and are located inside thecremaster muscle,while inguinal hernias lie anteromedial to the cord and are not intramuscular. Large lipomas may appear nearly indistinguishable as the fat engulfs anatomic boundaries, but they do not change position with coughing or straining.[22]
Differential diagnosis[edit]
Differential diagnosisof the symptoms of inguinal hernia mainly includes the following potential conditions:[23]
- Femoral hernia
- Epididymitis
- Testicular torsion
- Lipomas
- Inguinaladenopathy(Lymph nodeSwelling)
- Groinabscess
- Saphenous veindilation, calledSaphena varix
- Vascularaneurysmorpseudoaneurysm
- Hydrocele
- Varicocele
- Cryptorchidism(Undescended testes)
Management[edit]
Conservative[edit]
There is currently no medical recommendation about how to manage an inguinal hernia condition in adults, due to the fact that, until recently,[24][25]elective surgeryused to be recommended. The herniatruss(or hernia belt) is intended to contain a reducible inguinal hernia within the abdomen. It is not considered to provide a cure, and if the pads are hard and intrude into the hernia aperture they may cause scarring and enlargement of the aperture. In addition, most trusses with older designs are not able effectively to contain the hernia at all times, because their pads do not remain permanently in contact with the hernia. The more modern variety of truss is made with non-intrusive flat pads and comes with a guarantee to hold the hernia securely during all activities. They have been described by users as providing greater confidence and comfort when carrying out physically demanding tasks.[citation needed]However, their use is controversial, as data to determine whether they help prevent hernia complications are lacking.[1]A truss also increases the probability of complications, which include strangulation of the hernia, atrophy of the spermatic cord, and atrophy of the fascial margins. This allows the defect to enlarge and makes subsequent repair more difficult.[26]Their popularity is nonetheless likely to increase, as many individuals with small, painless hernias are now delaying hernia surgery due to the risk ofpost-herniorrhaphy pain syndrome.[27]Elasticated pants[specify]used by athletes may also provide useful support for the smaller hernia.[citation needed]
Surgical[edit]
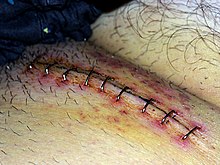
Surgical correction of inguinal hernias is called ahernia repair.It is not recommended in minimally symptomatic hernias, for whichwatchful waitingis advised, due to the risk ofpost herniorraphy pain syndrome.Surgery is commonly performed asoutpatient surgery.There are various surgical strategies which may be considered in the planning of inguinal hernia repair. These include the consideration of mesh use (e.g.syntheticorbiologic), open repair, use oflaparoscopy,type of anesthesia (general or local), appropriateness of bilateral repair, etc. Mesh or non mesh repairs have both benefits in different areas, but mesh repairs may reduce the rate of hernia reappearance, visceral or neurovascular injuries, length of hospital stay and time to return to activities of daily living.[28]Laparoscopy is most commonly used for non-emergency cases; however, a minimally invasive open repair may have a lower incidence of post-operative nausea and mesh associated pain. During surgery conducted under local anaesthesia, the patient will be asked to cough and strain during the procedure to help in demonstrating that the repair is without tension and sound.[29]

(photo: United States Military Medical Archives)
The photograph is blurry as the patient was shaking too much.
Constipation after hernia repair results in strain to evacuate the bowel causing pain, and fear that the sutures may rupture. Opioid analgesia makes constipation worse. Promoting an easy bowel motion is important post-operatively.
Surgical correction is always recommended for inguinal hernias in children.[30]
Emergency surgery for incarceration and strangulation carry much higher risk than planned, "elective" procedures. However, the risk of incarceration is low, evaluated at 0.2% per year.[31]On the other hand,surgeryhas a risk ofinguinodynia(10-12%), and this is why males with minimal symptoms are advised towatchful waiting.[31][32]However, if they experience discomfort while doing physical activities or they routinely avoid them for fear of pain, they should seek surgical evaluation.[33]For female patients, surgery is recommended even for asymptomatic patients.[34]
Epidemiology[edit]
A direct inguinal hernia is less common (~25–30% of inguinal hernias) and usually occurs in men over 40 years of age.
Men have an 8 times higherincidenceof inguinal hernia than women.[35]
See also[edit]
References[edit]
- ^abcdefghijklmFitzgibbons RJ J, Forse RA (19 February 2015)."Clinical practice. Groin hernias in adults"(PDF).The New England Journal of Medicine.372(8): 756–63.doi:10.1056/NEJMcp1404068.PMID25693015.Archived fromthe original(PDF)on 18 November 2021.Retrieved18 November2021.
- ^abcdDomino FJ (2014).The 5-minute clinical consult 2014(22nd ed.). Philadelphia, Pa.: Wolters Kluwer Health/Lippincott Williams & Wilkins. p. 562.ISBN978-1-4511-8850-9.
- ^Burcharth J, Pommergaard HC, Rosenberg J (2013). "The inheritance of groin hernia: a systematic review".Hernia.17(2): 183–9.doi:10.1007/s10029-013-1060-4.PMID23423330.S2CID27799467.
- ^abGBD 2015 Mortality and Causes of Death Collaborators (8 October 2016)."Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015".Lancet.388(10053): 1459–1544.doi:10.1016/S0140-6736(16)31012-1.PMC5388903.PMID27733281.
- ^Öberg S, Andresen K, Rosenberg J (2017)."Etiology of Inguinal Hernias: A Comprehensive Review".Frontiers in Surgery.4:52.doi:10.3389/fsurg.2017.00052.PMC5614933.PMID29018803.
- ^Mihailov E, Nikopensius T, Reigo A, Nikkolo C, Kals M, Aruaas K, et al. (2017)."Whole-exome Sequencing Identifies a Potential TTN Mutation in a Multiplex Family With Inguinal Hernia - PubMed".Hernia: The Journal of Hernias and Abdominal Wall Surgery.21(1): 95–100.doi:10.1007/s10029-016-1491-9.PMC5281683.PMID27115767.
- ^Sezer S, Şimşek N, Celik HT, Erden G, Ozturk G, Düzgün AP, et al. (2014)."Association of Collagen Type I Alpha 1 Gene Polymorphism With Inguinal Hernia - PubMed".Hernia: The Journal of Hernias and Abdominal Wall Surgery.18(4): 507–12.doi:10.1007/s10029-013-1147-y.PMID23925543.S2CID22999363.
- ^Gong Y, Shao C, Sun Q, Chen B, Jiang Y, Guo C, et al. (1994)."Genetic Study of Indirect Inguinal Hernia - PubMed".Journal of Medical Genetics.31(3): 187–92.doi:10.1136/jmg.31.3.187.PMC1049739.PMID8014965.
- ^Simons MP, Aufenacker T, Bay-Nielsen M, et al. (August 2009)."European Hernia Society guidelines on the treatment of inguinal hernia in adult patients".Hernia.13(4): 343–403.doi:10.1007/s10029-009-0529-7.PMC2719730.PMID19636493.
- ^GBD 2015 Disease and Injury Incidence and Prevalence Collaborators (8 October 2016)."Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990-2015: a systematic analysis for the Global Burden of Disease Study 2015".Lancet.388(10053): 1545–1602.doi:10.1016/S0140-6736(16)31678-6.PMC5055577.PMID27733282.
- ^GBD 2013 Mortality and Causes of Death Collaborators (17 December 2014)."Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013".Lancet.385(9963): 117–71.doi:10.1016/S0140-6736(14)61682-2.PMC4340604.PMID25530442.
- ^Neutra R, Velez A, Ferrada R, Galan R (January 1981). "Risk of incarceration of inguinal hernia in Cali, Colombia".Journal of Chronic Diseases.34(11): 561–564.doi:10.1016/0021-9681(81)90018-7.PMID7287860.
- ^Desarda MP (16 April 2003)."Surgical physiology of inguinal hernia repair - a study of 200 cases".BMC Surgery.3(1): 2.doi:10.1186/1471-2482-3-2.PMC155644.PMID12697071.
- ^Yoell JH (September 1959)."SURPRISES IN HERNIAL SACS—Diagnosis of Tumors by Microscopic Examination".California Medicine.91(3): 146–148.ISSN0008-1264.PMC1577810.PMID13846556.
- ^ab"Direct Inguinal Hernia".University of Connecticut. Archived fromthe originalon April 27, 2012.RetrievedMay 6,2012.
- ^James Harmon M.D. Lecture 13. Human Gross Anatomy. University of Minnesota. September 4, 2008.
- ^"Hernia: Treatment, Types, Symptoms (Pain) & Surgery".
- ^"UOTW #16 - Ultrasound of the Week".Ultrasound of the Week.2 September 2014.Retrieved27 May2017.
- ^"UOTW #40 - Ultrasound of the Week".Ultrasound of the Week.9 March 2015.
- ^LeBlanc KE, LeBlanc LL, LeBlanc KA (15 June 2013)."Inguinal hernias: diagnosis and management".American Family Physician.87(12): 844–8.PMID23939566.
- ^Stavros AT, Rapp C (September 2010). "Dynamic Ultrasound of Hernias of the Groin and Anterior Abdominal Wall".Ultrasound Quarterly.26(3): 135–169.doi:10.1097/RUQ.0b013e3181f0b23f.PMID20823750.S2CID31835133.
- ^abBurkhardt JH, Arshanskiy Y, Munson JL, Scholz FJ (March 2011). "Diagnosis of Inguinal Region Hernias with Axial CT: The Lateral Crescent Sign and Other Key Findings".RadioGraphics.31(2): E1–E12.doi:10.1148/rg.312105129.PMID21415178.
- ^Klingensmith ME, Chen LE, Glasgow SC, Goers TA, Melby SJ (2008).The Washington manual of surgery.Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins.ISBN978-0-7817-7447-5.
- ^Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, et al. (August 2009)."European Hernia Society guidelines on the treatment of inguinal hernia in adult patients".Hernia.13(4): 343–403.doi:10.1007/s10029-009-0529-7.PMC2719730.PMID19636493.
- ^Rosenberg J, Bisgaard T, Kehlet H, Wara P, Asmussen T, Juul P, et al. (February 2011). "Danish Hernia Database recommendations for the management of inguinal and femoral hernia in adults".Dan Med Bull.58(2): C4243.PMID21299930.
- ^Purkayastha S, Chow A, Athanasiou T, Tekkis P, Darzi A (July 2008)."Inguinal hernia".BMJ Clin Evid.2008.PMC2908002.PMID19445744.
- ^Aasvang E, Kehlet H (July 2005)."Chronic postoperative pain: the case of inguinal herniorrhaphy".Br J Anaesth.95(1): 69–76.doi:10.1093/bja/aei019.PMID15531621.
- ^Lockhart K, Dunn D, Teo S, Ng JY, Dhillon M, Teo E, et al. (2018)."Mesh versus non-mesh for inguinal and femoral hernia repair".Cochrane Database of Systematic Reviews.2018(9): CD011517.doi:10.1002/14651858.CD011517.pub2.PMC6513260.PMID30209805.
- ^Inguinal HerniaArchived2007-09-27 at theWayback Machine
- ^"Inguinal Hernia".UCSF Pediatric Surgery.Archived fromthe originalon 2020-10-26.Retrieved2018-11-15.
- ^abFitzgibbons RJ, Giobbie-Hurder A, Gibbs JO, Dunlop DD, Reda DJ, McCarthy M, et al. (18 January 2006). "Watchful Waiting vs Repair of Inguinal Hernia in Minimally Symptomatic Men".JAMA.295(3): 285–92.doi:10.1001/jama.295.3.285.PMID16418463.
- ^Simons MP, Aufenacker TJ, Berrevoet F, Bingener J, Bisgaard T, Bittner R, et al. (2017).World guidelines for groin hernia management(PDF).
- ^Brooks D."Overview of treatment for inguinal and femoral hernia in adults".www.uptodate.com.Retrieved2017-11-19.
- ^Rosenberg J, Bisgaard T, Kehlet H, Wara P, Asmussen T, Juul P, et al. (February 2011). "Danish Hernia Database recommendations for the management of inguinal and femoral hernia in adults".Danish Medical Bulletin.58(2): C4243.ISSN1603-9629.PMID21299930.
- ^"Inguinal hernia".Mayo Clinic.2017-08-11.
External links[edit]
- Indirect Inguinal Hernia - University of Connecticut Health Center
 Media related toInguinal herniaat Wikimedia Commons
Media related toInguinal herniaat Wikimedia Commons



