Polycystic ovary syndrome
| Polycystic ovary syndrome | |
|---|---|
| Other names | Hyperandrogenic anovulation (HA),[1] Stein-Leventhal syndrome[2] |
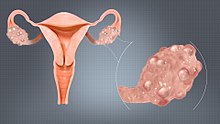 | |
| A polycystic ovary | |
| Specialty | Gynecology,endocrinology |
| Symptoms | Irregularmenstrual periods,heavy periods,excess hair,acne,pelvic pain,difficulty getting pregnant,patches of thick, darker, velvety skin[3] |
| Complications | Type 2 diabetes,obesity,obstructive sleep apnea,heart disease,mood disorders,endometrial cancer[4] |
| Duration | Long term[5] |
| Causes | Genetic and environmental factors[6][7] |
| Risk factors | Obesity,not enough exercise, family history[8] |
| Diagnostic method | Based on anovulation, highandrogenlevels,ovarian cysts[4] |
| Differential diagnosis | Adrenal hyperplasia,hypothyroidism,high blood levels of prolactin[9] |
| Treatment | Weight loss,exercise[10][11] |
| Medication | Birth control pills,metformin,GLP-1,anti-androgens[12] |
| Frequency | 2% to 20% of women of childbearing age[8][13] |
Polycystic ovary syndrome,orpolycystic ovarian syndrome(PCOS), is the most commonendocrinedisorder in women of reproductive age.[14]The syndrome is named aftercystswhich form on theovariesof some women with this condition, though this is not a universal symptom, and not the underlying cause of the disorder.[15][16]
Women with PCOS may experience irregularmenstrual periods,heavy periods,excess hair,acne,pelvic pain,difficulty getting pregnant,andpatches of thick, darker, velvety skin.[3]The primary characteristics of this syndrome include:hyperandrogenism,anovulation,insulin resistance,andneuroendocrinedisruption.[17]
A review of international evidence found that the prevalence of PCOS could be as high as 26% among some populations, though ranges between 4% and 18% are reported for general populations.[18][19][20]
The exact cause of PCOS remains uncertain, and treatment involves management of symptoms using medication.[19]
Definition
[edit]Two definitions are commonly used:
- NIH
- In 1990, a consensus workshop sponsored by theNIH/NICHDsuggested that a person has PCOS if they have all of the following:[21]
- Oligoovulation
- Signs ofandrogen excess(clinical or biochemical)
- Exclusion of other disorders that can result in menstrual irregularity and hyperandrogenism (e.g.: Congenital Suprarrenal Hyperplasia, androgen producer tumors, hyperprolactinemia).
- Rotterdam
- In 2003, a consensus workshop sponsored byESHRE/ASRMinRotterdamindicated PCOS to be present if any two out of three criteria are met, in the absence of other entities that might cause these findings:[22][23][24]
- Oligoovulationand/oranovulation
- Excess androgen activity
- Polycystic ovaries (bygynecologic ultrasound)
- The Rotterdam definition is wider, including many more women, the most notable ones being women without androgen excess. Critics say that findings obtained from the study of women with androgen excess cannot necessarily be extrapolated to women without androgen excess.[25][26]
- Androgen Excess PCOS Society
- In 2006, the Androgen Excess PCOS Society suggested a tightening of the diagnostic criteria to all of the following:[22]
- Excessandrogenactivity
- Oligoovulation/anovulation and/or polycystic ovaries
- Exclusion of other entities that would cause excess androgen activity
Signs and symptoms
[edit]Signs and symptoms of PCOS include irregular or nomenstrual periods,heavy periods,excess body and facial hair,acne,pelvic pain,difficulty getting pregnant,andpatches of thick, darker, velvety skin,[3]ovarian cysts, enlarged ovaries, excess androgen, and weight gain.[27][28]
Associated conditions includetype 2 diabetes,obesity,obstructive sleep apnea,heart disease,mood disorders,andendometrial cancer.[4]
Common signs and symptoms of PCOS include the following:
- Menstrual disorders:PCOS mostly producesoligomenorrhea(fewer than nine menstrual periods in a year) oramenorrhea(no menstrual periods for three or more consecutive months), but other types of menstrual disorders may also occur.[22]
- Infertility:This generally results directly from chronicanovulation(lack of ovulation).[22]
- High levels of masculinizing hormones:Known as hyperandrogenism, the most common signs areacneandhirsutism(male pattern of hair growth, such as on the chin or chest), but it may producehypermenorrhea(heavy and prolonged menstrual periods),androgenic alopecia(increased hair thinning or diffuse hair loss), or other symptoms.[22][29]Approximately three-quarters of women with PCOS (by the diagnostic criteria of NIH/NICHD 1990) have evidence ofhyperandrogenemia.[30]
- Metabolic syndrome:This appears as a tendency towardscentral obesityand other symptoms associated withinsulin resistance,including low energy levels and food cravings.[22]Seruminsulin,insulin resistance, andhomocysteinelevels are higher in women with PCOS.[31]
- Acne:A rise in testosterone levels, increases the oil production within the sebaceous glands and clogs pores.[32]For many women, the emotional impact is great and quality of life can be significantly reduced.[33]
- Androgenic alopecia:Estimates suggest that androgenic alopecia affects 22% of PCOS sufferers.[32]This is a result of high testosterone levels that are converted into the dihydrotestosterone (DHT) hormone. Hair follicles become clogged, making hair fall out and preventing further growth.[34]
- Acanthosis nigricans(AN): A skin condition where dark, thick and "velvety" patches can form.[35]
- Polycystic ovaries: PCOS is a complicated disorder characterized by high androgen levels, irregular menstruation, and/or small cysts on one or both ovaries.Ovariesmight get enlarged and comprise follicles surrounding the eggs. As result, ovaries might fail to function regularly. This disease is related to the number of follicles per ovary each month growing from the average range of 6–8 to double, triple or more.[citation needed]Women with PCOS have higher risk of multiple diseases including infertility, type 2 diabetes mellitus (DM-2), cardiovascular risk, metabolic syndrome, obesity, impaired glucose tolerance, depression, obstructive sleep apnea (OSA), endometrial cancer, and nonalcoholic fatty liver disease/nonalcoholic steatohepatitis (NAFLD/NASH).[36]
Women with PCOS tend to have central obesity, but studies are conflicting as to whether visceral and subcutaneous abdominal fat is increased, unchanged, or decreased in women with PCOS relative to non-PCOS women with the samebody mass index.[37]In any case, androgens, such astestosterone,androstanolone(dihydrotestosterone), andnandrolone decanoatehave been found to increase visceral fat deposition in both female animals and women.[38]
Although 80% of PCOS presents in women with obesity, 20% of women diagnosed with the disease are non-obese or "lean" women.[39]However, obese women that have PCOS have a higher risk of adverse outcomes, such ashypertension,insulin resistance,metabolic syndrome,andendometrial hyperplasia.[40]
Even though most women with PCOS are overweight or obese, it is important to acknowledge that non-overweight women can also be diagnosed with PCOS. Up to 30% of women diagnosed with PCOS maintain a normal weight before and after diagnosis. "Lean" women still face the various symptoms of PCOS with the added challenges of having their symptoms properly addressed and recognized. Lean women often go undiagnosed for years, and usually are diagnosed after struggles to conceive.[41]Lean women are likely to have a missed diagnosis of diabetes and cardiovascular disease, these women also have an increased risk of developing insulin resistance, despite not being overweight. Lean women are often taken less seriously with their diagnosis of PCOS, and also face challenges finding appropriate treatment options. This is because most treatment options are limited to approaches of losing weight and healthy dieting.[42]
Hormone levels
[edit]Testosteronelevels are usually elevated in women with PCOS.[43][44]In a 2020systematic reviewandmeta-analysisof sexual dysfunction related to PCOS which included 5,366 women with PCOS from 21 studies, testosterone levels were analyzed and were found to be 2.34 nmol/L (67 ng/dL) in women with PCOS and 1.57 nmol/L (45 ng/dL) in women without PCOS.[44]In a 1995 study of 1,741 women with PCOS, mean testosterone levels were 2.6 (1.1–4.8) nmol/L (75 (32–140) ng/dL).[45]In a 1998 study which reviewed many studies and subjected them to meta-analysis, testosterone levels in women with PCOS were 62 to 71 ng/dL (2.2–2.5 nmol/L) and testosterone levels in women without PCOS were about 32 ng/dL (1.1 nmol/L).[46]In a 2010 study of 596 women with PCOS which usedliquid chromatography–mass spectrometry(LC–MS) to quantify testosterone, median levels of testosterone were 41 and 47 ng/dL (with 25th–75th percentiles of 34–65 ng/dL and 27–58 ng/dL and ranges of 12–184 ng/dL and 1–205 ng/dL) via two different labs.[47]If testosterone levels are above 100 to 200 ng/dL, per different sources, other possible causes ofhyperandrogenism,such ascongenital adrenal hyperplasiaor anandrogen-secretingtumor,may be present and should be excluded.[45][48][43]
Associated conditions
[edit]Warning signs may include a change in appearance. But there are also manifestations of mental health problems, such as anxiety, depression, and eating disorders.[27][medical citation needed]
A diagnosis of PCOS suggests an increased risk of the following:
- Endometrial hyperplasiaandendometrial cancer(cancer of the uterine lining) are possible, due to overaccumulation of uterine lining, and also lack ofprogesterone,resulting in prolonged stimulation of uterine cells by estrogen.[21][49]It is not clear whether this risk is directly due to the syndrome or from the associated obesity,hyperinsulinemia,andhyperandrogenism.[50][51][52]
- Insulin resistance/type 2 diabetes.A review published in 2010 concluded that women with PCOS have an elevated prevalence of insulin resistance and type 2 diabetes, even when controlling forbody mass index(BMI).[21][53]PCOS is also associated with higher risk for diabetes.[54]
- High blood pressure,in particular if obese or during pregnancy[55]
- Depressionandanxiety[22][56]
- Dyslipidemia– disorders of lipid metabolism – cholesterol and triglycerides. Women with PCOS show a decreased removal ofatherosclerosis-inducing remnants, seemingly independent of insulin resistance/type 2 diabetes.[57]
- Cardiovascular disease,[21]with a meta-analysis estimating a 2-fold risk of arterial disease for women with PCOS relative to women without PCOS, independent of BMI.[58]
- Strokes[21]
- Weight gain[citation needed]
- Miscarriage[59][60]
- Sleep apnea,particularly if obesity is present[citation needed]
- Non-alcoholic fatty liver disease,particularly if obesity is present[citation needed]
- Acanthosis nigricans(patches of darkened skin under the arms, in the groin area, on the back of the neck)[21]
- Autoimmune thyroiditis[citation needed]
- Iron deficiency[61]
The risk ofovarian cancerandbreast canceris not significantly increased overall.[49]
Cause
[edit]PCOS is aheterogeneous disorderof uncertain cause.[62][63]There is some evidence that it is agenetic disease.Such evidence includes the familial clustering of cases, greaterconcordanceinmonozygoticcompared withdizygotictwins and heritability of endocrine and metabolic features of PCOS.[7][62][63]There is some evidence that exposure to higher than typical levels ofandrogensand theanti-Müllerian hormone(AMH)in uteroincreases the risk of developing PCOS in later life.[64]
It may be caused by a combination of genetic and environmental factors.[6][7][65]Risk factors includeobesity,a lack of physical exercise, and a family history of someone with the condition.[8]Diagnosis is based on two of the following three findings:anovulation,high androgen levels, andovarian cysts.[4]Cysts may be detectable byultrasound.[9]Other conditions that produce similar symptoms includeadrenal hyperplasia,hypothyroidism,andhigh blood levels of prolactin.[9]
Genetics
[edit]The genetic component appears to be inherited in anautosomal dominantfashion with highgenetic penetrancebut variableexpressivityin females; this means that each child has a 50% chance of inheriting the predisposing genetic variant(s) from a parent, and, if a daughter receives the variant(s), the daughter will have the disease to some extent.[63][66][67][68]The genetic variant(s) can be inherited from either the father or the mother, and can be passed along to both sons (who may be asymptomatic carriers or may have symptoms such as earlybaldnessand/or excessive hair) and daughters, who will show signs of PCOS.[66][68]Thephenotypeappears to manifest itself at least partially via heightened androgen levels secreted byovarian follicle thecacells from women with the allele.[67]The exact gene affected has not yet been identified.[7][63][69]In rare instances, single-gene mutations can give rise to the phenotype of the syndrome.[70]Current understanding of the pathogenesis of the syndrome suggests, however, that it is a complex multigenic disorder.[71]
Due to the scarcity of large-scale screening studies, the prevalence of endometrial abnormalities in PCOS remains unknown, though women with the condition may be at increased risk for endometrial hyperplasia and carcinoma as well as menstrual dysfunction and infertility.[citation needed]
The severity of PCOS symptoms appears to be largely determined by factors such as obesity.[7][22][72]PCOS has some aspects of ametabolic disorder,since its symptoms are partly reversible. Even though considered as agynecologicalproblem, PCOS consists of 28 clinical symptoms.[73]
Even though the name suggests that the ovaries are central to disease pathology, cysts are a symptom instead of the cause of the disease. Some symptoms of PCOS will persist even if both ovaries are removed; the disease can appear even if cysts are absent. Since its first description by Stein and Leventhal in 1935, the criteria of diagnosis, symptoms, and causative factors are subject to debate. Gynecologists often see it as a gynecological problem, with the ovaries being the primary organ affected. However, recent insights show a multisystem disorder, with the primary problem lies in hormonal regulation in thehypothalamus,with the involvement of many organs. The term PCOS is used due to the fact that there is a wide spectrum of symptoms possible. It is common to have polycystic ovaries without having PCOS; approximately 20% of European women have polycystic ovaries, but most of those women do not have PCOS.[15]
Environment
[edit]PCOS may be related to or worsened by exposures[clarification needed]during theprenatal period,[74][75][76]epigeneticfactors, environmental impacts (especially industrial endocrine disruptors, such asbisphenol Aand certain drugs)[77][78][79]and the increasing rates of obesity.[78]
Endocrine disruptorsare defined as chemicals that can interfere with theendocrine systemby mimicking hormones such asestrogen.According to theNIH (National Institute of Health),examples of endocrine disruptors can includedioxinsandtriclosan.Endocrine disruptors can cause adverse health impacts in animals.[80]Additional research is needed to assess the role that endocrine disruptors may play in disrupting reproductive health in women and possibly triggering or exacerbating PCOS and its related symptoms.[81]
Pathogenesis
[edit]Polycystic ovaries develop when the ovaries are stimulated to produce excessive amounts of androgenic hormones, in particular testosterone, by either one or a combination of the following (almost certainly combined with genetic susceptibility):[67]
- the release of excessiveluteinizing hormone(LH) by theanterior pituitarygland
- through high levels of insulin in the blood (hyperinsulinaemia) in women whose ovaries are sensitive to this stimulus
A majority of women with PCOS haveinsulin resistanceand/or areobese,which is a strong risk factor for insulin resistance, although insulin resistance is a common finding among women with PCOS in normal-weight women as well.[10][22][31]Elevated insulin levels contribute to or cause the abnormalities seen in thehypothalamic–pituitary–ovarian axisthat lead to PCOS. Hyperinsulinemia increasesGnRHpulse frequency,[82]which in turn results in an increase in the LH/FSH ratio[82][83]increased ovarian androgen production; decreased follicular maturation; and decreasedSHBGbinding.[82]Furthermore, excessive insulin increases the activity of17α-hydroxylase,which catalyzes the conversion ofprogesteronetoandrostenedione,which is in turn converted to testosterone. The combined effects ofhyperinsulinemiacontribute to an increased risk of PCOS.[82]
Adipose (fat) tissuepossessesaromatase,an enzyme that converts androstenedione toestroneand testosterone toestradiol.The excess of adipose tissue in obese women creates the paradox of having both excess androgens (which are responsible for hirsutism andvirilization) and excess estrogens (which inhibit FSH vianegative feedback).[84]
The syndrome acquired its most widely used name due to the common sign on ultrasound examination of multiple (poly) ovariancysts.These "cysts" are in fact immatureovarian follicles.The follicles have developed from primordial follicles, but this development has stopped ( "arrested" ) at an early stage, due to the disturbed ovarian function. The follicles may be oriented along the ovarian periphery, appearing as a 'string of pearls' on ultrasound examination.[85]
PCOS may be associated withchronic inflammation,[86]with several investigators correlating inflammatory mediators with anovulation and other PCOS symptoms.[87][88]Similarly, there seems to be a relation between PCOS and an increased level ofoxidative stress.[89]
Diagnosis
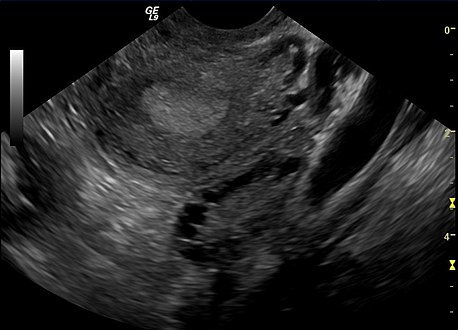
[edit]Not every person with PCOS has polycystic ovaries (PCO), nor does everyone withovarian cystshave PCOS; although apelvic ultrasoundis a major diagnostic tool, it is not the only one.[90]The diagnosis is fairly straightforward using the Rotterdam criteria, even when the syndrome is associated with a wide range of symptoms.[91]
-
Transvaginal ultrasound scan of polycystic ovary
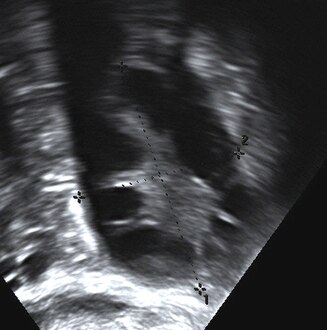
-
Polycystic ovary as seen on sonography
Differential diagnosis
[edit]Other causes of irregular or absent menstruation and hirsutism, such ashypothyroidism,congenital adrenal hyperplasia(21-hydroxylase deficiency) (which may cause excessive body hair, deep tone voice and others symptoms similar tohyperandrogenism),Cushing's syndrome,hyperprolactinemia(leading toanovulation), androgen-secreting neoplasms, and other pituitary or adrenal disorders, should be investigated.[22][24][92]
Assessment and testing
[edit]Standard assessment
[edit]- History-taking, specifically for menstrual pattern, obesity, hirsutism and acne. Aclinical prediction rulefound that these four questions can diagnose PCOS with asensitivityof 77.1% (95%confidence interval[CI] 62.7%–88.0%) and aspecificityof 93.8% (95% CI 82.8%–98.7%).[93]
- Gynecologic ultrasonography,specifically looking for smallovarian follicles.These are believed to be the result of disturbed ovarian function with failed ovulation, reflected by the infrequent or absent menstruation that is typical of the condition. In a normalmenstrual cycle,one egg is released from a dominant follicle – in essence, a cyst that bursts to release the egg. After ovulation, the follicle remnant is transformed into aprogesterone-producingcorpus luteum,which shrinks and disappears after approximately 12–14 days. In PCOS, there is a so-called "follicular arrest"; i.e., several follicles develop to a size of 5–7 mm, but not further. No single follicle reaches the preovulatory size (16 mm or more). According to the Rotterdam criteria, which are widely used for diagnosis of PCOS,[10]12 or more small follicles should be seen in a suspect ovary on ultrasound examination.[21]More recent research suggests that there should be at least 25 follicles in an ovary to designate it as having polycystic ovarian morphology (PCOM) in women aged 18–35 years.[94]The follicles may be oriented in the periphery, giving the appearance of a 'string of pearls'.[95]If a high-resolution transvaginal ultrasonography machine is not available, an ovarian volume of at least 10 ml is regarded as an acceptable definition of having polycystic ovarian morphology. rather than follicle count.[94]
- Laparoscopicexamination may reveal a thickened, smooth, pearl-white outer surface of the ovary. (This would usually be an incidental finding if laparoscopy were performed for some other reason, as it would not be routine to examine the ovaries in this way to confirm a diagnosis of PCOS.)[96]
- Serum (blood) levels ofandrogens,includingandrostenedioneandtestosteronemay be elevated.[22]Dehydroepiandrosterone sulfate(DHEA-S) levels above 700–800 μg/dL are highly suggestive of adrenal dysfunction because DHEA-S is made exclusively by the adrenal glands.[97][92]Thefree testosteronelevel is thought to be the best measure,[92][98]with approximately 60 per cent of PCOS patients demonstrating supranormal levels.[30]
Some other blood tests are suggestive but not diagnostic. The ratio of LH (luteinizing hormone) to FSH (follicle-stimulating hormone), when measured ininternational units,is elevated in women with PCOS. Commoncut-offsto designate abnormally high LH/FSH ratios are 2:1[99]or 3:1[92]as tested on day 3 of the menstrual cycle. The pattern is not very sensitive; a ratio of 2:1 or higher was present in less than 50% of women with PCOS in one study.[99]There are often low levels ofsex hormone-binding globulin,[92]in particular among obese or overweight women.[100] Anti-Müllerian hormone(AMH) is increased in PCOS, and may become part of its diagnostic criteria.[101][102][103]
Glucose tolerance testing
[edit]- Two-hour oralglucose tolerance test(GTT) in women with risk factors (obesity, family history, history of gestational diabetes)[22]may indicate impaired glucose tolerance (insulin resistance) in 15–33% of women with PCOS.[92]Frank diabetes can be seen in 65–68% of women with this condition.[104]Insulin resistance can be observed in both normal weight and overweight people, although it is more common in the latter (and in those matching the stricter NIH criteria for diagnosis); 50–80% of people with PCOS may have insulin resistance at some level.[22]
- Fasting insulin level or GTT with insulin levels (also called IGTT). Elevated insulin levels have been helpful to predict response to medication and may indicate women needing higher doses of metformin or the use of a second medication to significantly lower insulin levels. Elevatedblood sugarand insulin values do not predict who responds to an insulin-lowering medication, low-glycemic diet, and exercise. Many women with normal levels may benefit from combination therapy. A hypoglycemic response in which the two-hour insulin level is higher and the blood sugar lower than fasting is consistent with insulin resistance. A mathematical derivation known as the HOMAI, calculated from the fasting values in glucose and insulin concentrations, allows a direct and moderately accurate measure of insulin sensitivity (glucose-level x insulin-level/22.5).[105]
The four types of PCOS
[edit]PCOS diagnosis is categorized into four different types;
- Insulin-resistant PCOSis the most common and occurs because of high insulin levels in the body, as a result the pancreas releases more insulin that then leaves the body at an excess of insulin that then signals the body to produce androgen at higher levels.[106]
- Inflammatory PCOSresults from inflammation in the body that is caused by stress and or high inflamatory foods. With inflamatory PCOS because of the inflammation the body will not ovulate, that results in an imbalance in hormones that then causes the body to produce androgen at higher levels.[106]
- Post-pill PCOSresults from individuals stopping oral contraceptives. When you stop taking these pills the body will produce androgen at higher levels resulting in PCOS symptoms.[106]
- Adrenal PCOSis a PCOS caused by how our body reacts to stress. As a result DHEAS a type of androgens that from in the adrenal glands.[106]
Management
[edit]PCOS has no cure.[5]Treatment may involve lifestyle changes such as weight loss and exercise.[10][11]
Recent research suggests that daily exercise including both aerobic and strength activities can improve hormone imbalances.[107]
Birth control pillsmay help with improving the regularity of periods, excess hair growth, and acne.[12]Combined oral contraceptives are especially effective, and used as the first-line of treatment to reduce acne and hirsutism, and regulate menstrual cycle. This is especially the case in adolescents.[107]
Metformin,GLP-1,andanti-androgensmay also help.[12]Other typical acne treatments and hair removal techniques may be used.[12]Efforts to improve fertility include weight loss,metformin,andovulation inductionusingclomipheneorletrozole.[108]In vitro fertilizationis used by some in whom other measures are not effective.[108]
Certain cosmetic procedures may also help alleviate symptoms in some cases. For example, the use of laser hair removal, electrolysis, or general waxing, plucking and shaving are all effective methods for reducing hirsutism.[35] The primary treatments for PCOS include lifestyle changes and use of medications.[109]
Goals of treatment may be considered under four categories:[citation needed]
- Lowering of insulin resistance
- Reducing androgen and testosterone levels
- Restoration of fertility
- Treatment ofhirsutismor acne
- Restoration of regular menstruation, and prevention ofendometrial hyperplasiaandendometrial cancer
In each of these areas, there is considerable debate as to the optimal treatment. One of the major factors underlying the debate is the lack of large-scale clinical trials comparing different treatments.Smaller trialstend to beless reliableand hence may produce conflicting results. General interventions that help to reduce weight or insulin resistance can be beneficial for all these aims, because they address what is believed to be the underlying cause.[110]As PCOS appears to cause significant emotional distress, appropriate support may be useful.[111]
Diet
[edit]Where PCOS is associated with being overweight or obesity, successful weight loss is the most effective method of restoring normal ovulation/menstruation. TheAmerican Association of Clinical Endocrinologistsguidelines recommend a goal of achieving 10–15% weight loss or more, which improvesinsulin resistanceand all[clarification needed]hormonal disorders.[112]Still, many women find it very difficult to achieve and sustain significant weight loss. Insulin resistance itself can cause increased food cravings and lower energy levels, which can make it difficult to lose weight on a regular weight-loss diet. Ascientific reviewin 2013 found similar improvements in weight, body composition andpregnancy rate,menstrual regularity, ovulation, hyperandrogenism, insulin resistance, lipids, and quality of life to occur with weight loss, independent of diet composition.[113]Still, alow GI diet,in which a significant portion of total carbohydrates is obtained from fruit, vegetables, and whole-grain sources, has resulted in greater menstrual regularity than amacronutrient-matched healthy diet.[113]
Reducing intake of food groups that cause inflammation, such as dairy, sugars and simple carbohydrates, can be beneficial.[35]
Amediterranean dietis often very effective due to its anti-inflammatory and anti-oxidative properties.[107]
Vitamin D deficiencymay play some role in the development of themetabolic syndrome,and treatment of any such deficiency is indicated.[114][115]However, a systematic review of 2015 found no evidence that vitamin D supplementation reduced or mitigated metabolic and hormonal dysregulations in PCOS.[116]As of 2012, interventions usingdietary supplementsto correct metabolic deficiencies in people with PCOS had been tested in small, uncontrolled and nonrandomized clinical trials; the resulting data are insufficient to recommend their use.[117]
Medications
[edit]Medications for PCOS includeoral contraceptivesandmetformin.The oral contraceptives increasesex hormone binding globulinproduction, which increases binding of free testosterone. This reduces the symptoms ofhirsutismcaused by high testosterone and regulates return to normalmenstrual periods.[114]Anti-androgenssuch asfinasteride,flutamide,spironolactone,andbicalutamidedo not show advantages over oral contraceptives, but could be an option for people who do not tolerate them.[118]Finasterideis the only oral medication for the treatment ofandrogenic alopecia,that isFDAapproved.[35]
Metformin is a medication commonly used intype 2 diabetes mellitusto reduce insulin resistance, and is usedoff label(in the UK, US, AU and EU) to treat insulin resistance seen in PCOS. In many cases, metformin also supports ovarian function and return to normal ovulation.[114][119]A newer insulin resistance medication class, thethiazolidinediones(glitazones), have shown equivalent efficacy to metformin, but metformin has a more favorable side effect profile.[120][121]The United Kingdom'sNational Institute for Health and Clinical Excellencerecommended in 2004 that women with PCOS and abody mass indexabove 25 be given metformin when other therapy has failed to produce results.[122][123]Metformin may not be effective in every type of PCOS, and therefore there is some disagreement about whether it should be used as a general first line therapy.[124]In addition to this, metformin is associated with several unpleasant side effects: including abdominal pain, metallic taste in the mouth, diarrhoea and vomiting.[125]Metformin is thought to be safe to use during pregnancy (pregnancy categoryB in the US).[126]A review in 2014 concluded that the use of metformin does not increase the risk of majorbirth defectsin women treated with metformin during the first trimester.[127]Liraglutide may reduce weight and waist circumference in people with PCOS more than other medications.[128]The use ofstatinsin the management of underlying metabolic syndrome remains unclear.[109]
It can be difficult to become pregnant with PCOS because it causes irregularovulation.Medications to induce fertility when trying to conceive include the ovulation inducerclomipheneor pulsatileleuprorelin.Evidence from randomised controlled trials suggests that in terms of live birth, metformin may be better than placebo, and metform plus clomiphene may be better than clomiphene alone, but that in both cases women may be more likely to experience gastrointestinal side effects with metformin.[129]
Infertility
[edit]Not all people with PCOS have difficulty becoming pregnant. But some individuals with PCOS may have difficulty getting pregnant since their body does not produce the hormones necessary for regular ovulation.[130]PCOS might also increase the risk of miscarriage or premature delivery. However, it is possible to have a normal pregnancy. Including medical care and a healthy lifestyle to follow.[citation needed]
For those that do,anovulationor infrequent ovulation is a common cause and PCOS is the main cause of anovulatory infertility.[131]Other factors include changed levels ofgonadotropins,hyperandrogenemia,andhyperinsulinemia.[132]Like women without PCOS, women with PCOS that are ovulating may be infertile due to other causes, such as tubal blockages due to a history of sexually transmitted diseases.[133]
For overweight anovulatory women with PCOS,weight lossand diet adjustments, especially to reduce the intake of simple carbohydrates, are associated with resumption of natural ovulation.[134]Digital health interventions have been shown to be particularly effective in providing combined therapy to manage PCOS through both lifestyle changes and medication.[135]
Femarais an alternative medicine that raises FSH levels and promote the development of the follicle.[35]
For those women that after weight loss still are anovulatory or for anovulatory lean women, thenovulation inductionusing the medicationsletrozoleorclomiphene citrateare the principal treatments used to promote ovulation.[136][137][138]Clomiphene can cause mood swings and abdominal cramping for some.[35]
Previously, the anti-diabetes medicationmetforminwas recommended treatment for anovulation, but it appears less effective than letrozole or clomiphene.[139][140]
For women not responsive to letrozole or clomiphene and diet and lifestyle modification, there are options available includingassisted reproductive technologyprocedures such ascontrolled ovarian hyperstimulationwithfollicle-stimulating hormone(FSH) injections followed byin vitro fertilisation(IVF).[141]
Though surgery is not commonly performed, the polycystic ovaries can be treated with a laparoscopic procedure called "ovarian drilling"(puncture of 4–10 small follicles with electrocautery, laser, or biopsy needles), which often results in either resumption of spontaneous ovulations[114]or ovulations after adjuvant treatment with clomiphene or FSH.[142](Ovarian wedge resection is no longer used as much due to complications such asadhesionsand the presence of frequently effective medications.) There are, however, concerns about the long-term effects of ovarian drilling on ovarian function.[114]
In a small UK randomized trial,bariatric surgeryled to more spontaneous ovulations than behavioral interventions combined with medical therapy in adult women with PCOS, raising the prospect that surgery could enhance prospects of spontaneous fertility.[143]
Mental health
[edit]Women with PCOS are far more likely to have depression than women without. Symptoms of depression might be heightened by certain physiological manifestations of this disease such as hirsutism or obesity that can lead to low self-esteem or poor body image.[33]Researchers suggest that there be mental health screenings performed in tandem with PCOS assessment in order to identify these complications early and treat them accordingly.[144]
PCOS is associated with other mental health related conditions besides depression such asanxiety,bipolar disorder,andobsessive–compulsive disorder.[33]Additionally, it has been found to significantly increase risk of eating disorders.[144]Screening for these mental health conditions will also be helpful in treatment of PCOS.
Lifestyle changes for people with PCOS have been proven to be difficult due to lack of intrinsic motivation, altered risk perception or other PCOS-related barriers. However, self management techniques and behavior change can be taught in a multidisciplinary approach with the goal of supporting those with PCOS in managing their symptoms.[145]
Hirsutism and acne
[edit]When appropriate (e.g., in women of child-bearing age who require contraception), a standard contraceptive pill is frequently effective in reducing hirsutism.[114]Progestogens such as norgestrel and levonorgestrel should be avoided due to their androgenic effects.[114]Metformin combined with an oral contraceptive may be more effective than either metformin or the oral contraceptive on its own.[146]
In the case of taking medication for acne, Kelly Morrow-Baez PHD, in her exposition titledThriving with PCOS,informs that it "takes time for medications to adjust hormone levels, and once those hormone levels are adjusted, it takes more time still for pores to be unclogged of overproduced oil and for any bacterial infections under the skin to clear up before you will see discernible results." (p. 138)[35]
Other medications with anti-androgen effects includeflutamide,[147]andspironolactone,[114]which can give some improvement in hirsutism. Metformin can reduce hirsutism, perhaps by reducing insulin resistance, and is often used if there are other features such as insulin resistance, diabetes, or obesity that should also benefit from metformin.Eflornithine(Vaniqa) is a medication that is applied to the skin in cream form, and acts directly on the hair follicles to inhibit hair growth. It is usually applied to the face.[114]5-alpha reductase inhibitors(such asfinasterideanddutasteride) may also be used;[148]they work by blocking the conversion oftestosteronetodihydrotestosterone(the latter of which responsible for most hair growth alterations andandrogenic acne).
Although these agents have shown significant efficacy in clinical trials (for oral contraceptives, in 60–100% of individuals[114]), the reduction in hair growth may not be enough to eliminate the social embarrassment of hirsutism, or the inconvenience of plucking or shaving. Individuals vary in their response to different therapies. It is usually worth trying other medications if one does not work, but medications do not work well for all individuals.[149]
Menstrual irregularity
[edit]If fertility is not the primary aim, thenmenstruationcan usually be regulated with a contraceptive pill.[114]The purpose of regulating menstruation, in essence, is for the patient's convenience, and perhaps their sense of well-being; there is no medical requirement for regular periods, as long as they occur sufficiently often.[150]
If a regular menstrual cycle is not desired, then therapy for an irregular cycle is not necessarily required. Most experts say that, if a menstrual bleed occurs at least every three months, then the endometrium (womb lining) is being shed sufficiently often to prevent an increased risk of endometrial abnormalities or cancer.[151]If menstruation occurs less often or not at all, some form of progestogen replacement is recommended.[148]
Alternative medicine
[edit]A 2017 review concluded that while both myo-inositol and D-chiro-inositols may regulate menstrual cycles and improve ovulation, there is a lack of evidence regarding effects on the probability of pregnancy.[152][153]A 2012 and 2017 review have foundmyo-inositolsupplementation appears to be effective in improving several of the hormonal disturbances of PCOS.[154][155]Myo-inositol reduces the amount of gonadotropins and the length of controlled ovarian hyperstimulation in women undergoing in vitro fertilization.[156]A 2011 review found not enough evidence to conclude any beneficial effect fromD-chiro-inositol.[157]There is insufficient evidence to support the use ofacupuncture,current studies are inconclusive and there's a need for additionalrandomized controlled trials.[158][159]
Epidemiology
[edit]PCOS is the most commonendocrine disorderamong women between the ages of 18 and 44.[22]It affects approximately 2% to 20% of this age group depending on how it is defined.[8][13]When someone is infertile due to lack of ovulation, PCOS is the most common cause and could guide to patients' diagnosis.[4]The earliest known description of what is now recognized as PCOS dates from 1721 in Italy.[160]
The prevalence of PCOS depends on the choice of diagnostic criteria. TheWorld Health Organizationestimates that it affects 116 million women worldwide as of 2010 (3.4% of women).[161]Another estimate indicates that 7% of women of reproductive age are affected.[162]Another study using the Rotterdam criteria found that about 18% of women had PCOS, and that 70% of them were previously undiagnosed.[22]Prevalence also varies across countries due to lack of large-scale scientific studies; India, for example, has a purported rate of 1 in 5 women having PCOS.[163]
There are few studies that have investigated the racial differences in cardiometabolic factors in women with PCOS. There is also limited data on the racial differences in the risk of metabolic syndrome and cardiovascular disease in adolescents and young adults with PCOS.[164]The first study to comprehensively examine racial differences discovered notable racial differences in risk factors for cardiovascular disease. African American women were found to be significantly more obese, with a significantly higher prevalence of metabolic syndrome compared to white adult women with PCOS.[165]It is important for the further research of racial differences among women with PCOS, to ensure that every woman that is affected by PCOS has the available resources for management.[166][167]
Ultrasonographic findings of polycystic ovaries are found in 8–25% of women non-affected by the syndrome.[168][169][170][171]14% women on oral contraceptives are found to have polycystic ovaries.[169]Ovarian cysts are also a common side effect of levonorgestrel-releasingintrauterine devices(IUDs).[172]
There are few studies that have investigated the racial differences in cardiometabolic factors in women with PCOS.[173]
History
[edit]The condition was first described in 1935 by American gynecologists Irving F. Stein, Sr. and Michael L. Leventhal, from whom its original name ofStein–Leventhal syndromeis taken.[90][21]Stein and Leventhal first described PCOS as an endocrine disorder in the United States, and since then, it has become recognized as one of the most common causes of oligo ovulatory infertility among women.[49]
The earliest published description of a person with what is now recognized as PCOS was in 1721 in Italy.[160]Cyst-related changes to the ovaries were described in 1844.[160]
Etymology
[edit]Other names for this syndrome include polycystic ovarian syndrome, polycystic ovary disease, functional ovarian hyperandrogenism, ovarianhyperthecosis,sclerocystic ovary syndrome, and Stein–Leventhal syndrome. Theeponymouslast option is the original name; it is now used, if at all, only for the subset of women with all the symptoms of amenorrhea with infertility,hirsutism,and enlarged polycystic ovaries.[90]
Most common names for this disease derive from a typical finding on medical images, called a polycystic ovary. A polycystic ovary has an abnormally large number of developing eggs visible near its surface, looking like many smallcysts.[90]
Society and culture
[edit]In 2005, 4 million cases of PCOS were reported in the US, costing $4.36 billion in healthcare costs.[174]In 2016 out of the National Institute Health's research budget of $32.3 billion for that year, 0.1% was spent on PCOS research.[175]Among those aged between 14 and 44, PCOS is conservatively estimated to cost $4.37 billion per year.[23]
As opposed to women in the general population, women with PCOS experience higher rates of depression and anxiety. International guidelines and Indian guidelines suggest psychosocial factors should be considered in women with PCOS, as well as screenings for depression and anxiety.[176]Globally, this aspect has been increasingly focused on because it reflects the true impact of PCOS on the lives of patients. Research shows that PCOS adversely impacts a patient's quality of life.[176]
Public figures
[edit]A number of celebrities and public figures have spoken about their experiences with PCOS, including:
- Victoria Beckham[177]
- Maci Bookout[178]
- Frankie Bridge[179]
- Harnaam Kaur[180]
- Jaime King[181]
- Chrisette Michele[182]
- Lea Michele[183]
- Keke Palmer[184]
- Sasha Pieterse[185][186]
- Daisy Ridley[187]
- Romee Strijd[188]
- Lee Tilghman[189]
See also
[edit]References
[edit]- ^Kollmann M, Martins WP, Raine-Fenning N (2014)."Terms and thresholds for the ultrasound evaluation of the ovaries in women with hyperandrogenic anovulation".Human Reproduction Update.20(3): 463–464.doi:10.1093/humupd/dmu005.PMID24516084.
- ^Legro RS (2017)."Stein-Leventhal syndrome".Encyclopedia Britannica.Archivedfrom the original on 29 October 2020.Retrieved30 January2021.[better source needed]
- ^abc"What are the symptoms of PCOS?".Eunice Kennedy Shriver National Institute of Child Health and Human Development.29 September 2022.Archivedfrom the original on 9 October 2021.Retrieved13 October2021.
- ^abcde"Polycystic Ovary Syndrome (PCOS): Condition Information".National Institute of Child Health and Human Development. January 31, 2017.Archivedfrom the original on 22 October 2018.Retrieved19 November2018.
- ^ab"Is there a cure for PCOS?".Eunice Kennedy Shriver National Institute of Child Health and Human Development.31 January 2017.Archivedfrom the original on 9 October 2021.Retrieved13 October2021.
- ^abDe Leo V, Musacchio MC, Cappelli V, Massaro MG, Morgante G, Petraglia F (July 2016)."Genetic, hormonal and metabolic aspects of PCOS: an update".Reproductive Biology and Endocrinology(Review).14(1): 38.doi:10.1186/s12958-016-0173-x.PMC4947298.PMID27423183.
- ^abcdeDiamanti-Kandarakis E, Kandarakis H, Legro RS (August 2006). "The role of genes and environment in the etiology of PCOS".Endocrine.30(1): 19–26.doi:10.1385/ENDO:30:1:19.PMID17185788.S2CID21220430.
- ^abcd"What causes PCOS?".Eunice Kennedy Shriver National Institute of Child Health and Human Development.29 September 2022.Archivedfrom the original on 9 October 2021.Retrieved13 October2021.
- ^abc"How do health care providers diagnose PCOS?".Eunice Kennedy Shriver National Institute of Child Health and Human Development.29 September 2022.Archivedfrom the original on 9 October 2021.Retrieved13 October2021.
- ^abcdMortada R, Williams T (August 2015). "Metabolic Syndrome: Polycystic Ovary Syndrome".FP Essentials(Review).435:30–42.PMID26280343.
- ^abGiallauria F, Palomba S, Vigorito C, Tafuri MG, Colao A, Lombardi G, et al. (July 2009). "Androgens in polycystic ovary syndrome: the role of exercise and diet".Seminars in Reproductive Medicine(Review).27(4): 306–315.doi:10.1055/s-0029-1225258.PMID19530064.S2CID260321191.
- ^abcdNational Institutes of Health (NIH)(2014-07-14)."Treatments to Relieve Symptoms of PCOS".Archivedfrom the original on 2 April 2015.Retrieved13 March2015.
- ^abPal L, ed. (2013)."Diagnostic Criteria and Epidemiology of PCOS".Polycystic Ovary Syndrome Current and Emerging Concepts.Dordrecht: Springer. p. 7.ISBN978-1-4614-8394-6.Archivedfrom the original on 2017-09-10.
- ^Goodman NF, Cobin RH, Futterweit W, Glueck JS, Legro RS, Carmina E (November 2015)."American Association of Clinical Endocrinologists, American College of Endocrinology, and androgen excess and PCOS society disease state clinical review: guide to the best practices in the evaluation and treatment of polycystic ovary syndrome-part 1".Endocrine Practice.21(11): 1291–1300.doi:10.4158/EP15748.DSC.PMID26509855.
- ^abDunaif A, Fauser BC (November 2013)."Renaming PCOS--a two-state solution".The Journal of Clinical Endocrinology and Metabolism.98(11): 4325–4328.doi:10.1210/jc.2013-2040.PMC3816269.PMID24009134.
Around 20% of European women have polycystic ovaries (the prevalence is even higher in some other populations) but approximately two-thirds of these women do not have PCOS
- ^Khan MJ, Ullah A, Basit S. Genetic Basis of Polycystic Ovary Syndrome (PCOS): Current Perspectives. Appl Clin Genet. 2019 Dec 24;12:249-260. doi: 10.2147/TACG.S200341. PMID 31920361; PMCID: PMC6935309.
- ^Crespo RP, Bachega TA, Mendonça BB, Gomes LG (June 2018)."An update of genetic basis of PCOS pathogenesis".Archives of Endocrinology and Metabolism.62(3): 352–361.doi:10.20945/2359-3997000000049.PMC10118782.PMID29972435.S2CID49681196.
- ^Muscogiuri G, Altieri B, de Angelis C, Palomba S, Pivonello R, Colao A, et al. (September 2017). "Shedding new light on female fertility: The role of vitamin D".Reviews in Endocrine & Metabolic Disorders.18(3): 273–283.doi:10.1007/s11154-017-9407-2.PMID28102491.S2CID33422072.
- ^abLentscher JA, Slocum B, Torrealday S (March 2021). "Polycystic Ovarian Syndrome and Fertility".Clinical Obstetrics and Gynecology.64(1): 65–75.doi:10.1097/GRF.0000000000000595.PMID33337743.S2CID229323594.
- ^Wolf WM, Wattick RA, Kinkade ON, Olfert MD (November 2018)."Geographical Prevalence of Polycystic Ovary Syndrome as Determined by Region and Race/Ethnicity".International Journal of Environmental Research and Public Health.15(11): 2589.doi:10.3390/ijerph15112589.PMC6266413.PMID30463276.
indigenous Australian women could have a prevalence as high as 26%
- ^abcdefghPolycystic Ovarian SyndromeateMedicine
- ^abcdefghijklmnoTeede H, Deeks A, Moran L (June 2010)."Polycystic ovary syndrome: a complex condition with psychological, reproductive and metabolic manifestations that impacts on health across the lifespan".BMC Medicine.8(1): 41.doi:10.1186/1741-7015-8-41.PMC2909929.PMID20591140.
- ^abAzziz R (March 2006)."Controversy in clinical endocrinology: diagnosis of polycystic ovarian syndrome: the Rotterdam criteria are premature".The Journal of Clinical Endocrinology and Metabolism.91(3): 781–785.doi:10.1210/jc.2005-2153.PMID16418211.
- ^abRotterdam ESHRE/ASRM-Sponsored PCOS consensus workshop group (January 2004)."Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS)".Human Reproduction.19(1): 41–47.doi:10.1093/humrep/deh098.PMID14688154.
- ^Carmina E (February 2004)."Diagnosis of polycystic ovary syndrome: from NIH criteria to ESHRE-ASRM guidelines".Minerva Ginecologica.56(1): 1–6.PMID14973405.NAID10025610607.Archivedfrom the original on 2021-11-02.Retrieved2021-10-13.
- ^Hart R, Hickey M, Franks S (October 2004). "Definitions, prevalence and symptoms of polycystic ovaries and polycystic ovary syndrome".Best Practice & Research. Clinical Obstetrics & Gynaecology.18(5): 671–683.doi:10.1016/j.bpobgyn.2004.05.001.PMID15380140.
- ^ab"What We Talk About When We Talk About PCOS".www.vice.com.23 January 2019.Archivedfrom the original on 2022-01-19.Retrieved2022-01-19.
- ^"Polycystic Ovary Syndrome (PCOS)".www.hopkinsmedicine.org.2022-02-28.Archivedfrom the original on 2023-02-10.Retrieved2023-02-09.
- ^Cortet-Rudelli C, Dewailly D (Sep 21, 2006)."Diagnosis of Hyperandrogenism in Female Adolescents".Hyperandrogenism in Adolescent Girls.Armenian Health Network, Health.am.Archivedfrom the original on 2007-09-30.Retrieved2006-11-21.
- ^abHuang A, Brennan K, Azziz R (April 2010)."Prevalence of hyperandrogenemia in the polycystic ovary syndrome diagnosed by the National Institutes of Health 1990 criteria".Fertility and Sterility.93(6): 1938–1941.doi:10.1016/j.fertnstert.2008.12.138.PMC2859983.PMID19249030.
- ^abNafiye Y, Sevtap K, Muammer D, Emre O, Senol K, Leyla M (April 2010)."The effect of serum and intrafollicular insulin resistance parameters and homocysteine levels of nonobese, nonhyperandrogenemic polycystic ovary syndrome patients on in vitro fertilization outcome".Fertility and Sterility.93(6): 1864–1869.doi:10.1016/j.fertnstert.2008.12.024.PMID19171332.
- ^abPasquali R (2018). "Lifestyle Interventions and Natural and Assisted Reproduction in Patients with PCOS".Infertility in Women with Polycystic Ovary Syndrome.Cham: Springer International Publishing. pp. 169–180.doi:10.1007/978-3-319-45534-1_13.ISBN978-3-319-45533-4.
- ^abcBrutocao C, Zaiem F, Alsawas M, Morrow AS, Murad MH, Javed A (November 2018). "Psychiatric disorders in women with polycystic ovary syndrome: a systematic review and meta-analysis".Endocrine.62(2): 318–325.doi:10.1007/s12020-018-1692-3.PMID30066285.S2CID51889051.
- ^Devi T (2018). "Lifestyle Modifications in Polycystic Ovarian Syndrome".Decoding Polycystic Ovarian Syndrome (PCOS).Jaypee Brothers Medical Publishers (P) Ltd. p. 195.doi:10.5005/jp/books/13089_17.ISBN978-93-86322-85-2.
- ^abcdefgMorrow-Baez K (2018).Thriving with PCOS: Lifestyle Strategies to Successfully Manage Polycystic Ovary Syndrome.Rowman & Littlefield Publishers.
- ^Rasquin LI, Anastasopoulou C, Mayrin JV (2023). "Polycystic Ovarian Disease".StatPearls.StatPearls Publishing.PMID29083730.Archivedfrom the original on 2023-05-08.Retrieved2023-09-01.
- ^Sam S (February 2015). "Adiposity and metabolic dysfunction in polycystic ovary syndrome".Hormone Molecular Biology and Clinical Investigation.21(2): 107–116.doi:10.1515/hmbci-2015-0008.PMID25781555.S2CID23592351.
- ^Corbould A (October 2008). "Effects of androgens on insulin action in women: is androgen excess a component of female metabolic syndrome?".Diabetes/Metabolism Research and Reviews.24(7): 520–532.doi:10.1002/dmrr.872.PMID18615851.S2CID24630977.
- ^Goyal M, Dawood AS (2017)."Debates Regarding Lean Patients with Polycystic Ovary Syndrome: A Narrative Review".Journal of Human Reproductive Sciences.10(3): 154–161.doi:10.4103/jhrs.JHRS_77_17.PMC5672719.PMID29142442.
- ^Sachdeva G, Gainder S, Suri V, Sachdeva N, Chopra S (2019)."Obese and Non-obese Polycystic Ovarian Syndrome: Comparison of Clinical, Metabolic, Hormonal Parameters, and their Differential Response to Clomiphene".Indian Journal of Endocrinology and Metabolism.23(2): 257–262.doi:10.4103/ijem.IJEM_637_18.PMC6540884.PMID31161114.
- ^Johnstone E, Cannon-Albright L, Peterson CM, Allen-Brady K (July 2018). "Lean PCOS may be a genetically distinct from obese PCOS: lean women with polycystic ovary syndrome and their relatives have no increased risk of T2DM".Human Reproduction.33.Oxford, England: Oxford Univ Press: 454.doi:10.26226/morressier.5af300b3738ab10027aa99cd.S2CID242055977.
- ^Goyal M, Dawood AS (2017)."Debates Regarding Lean Patients with Polycystic Ovary Syndrome: A Narrative Review".Journal of Human Reproductive Sciences.10(3): 154–161.doi:10.4103/jhrs.jhrs_77_17.PMC5672719.PMID29142442.
- ^abMazze R, Strock ES, Simonson GD, Bergenstal RM (11 January 2007)."Type 2 Diabetes and Metabolic Syndrome in Children and Adolescents".Staged Diabetes Management: A Systematic Approach(2nd ed.). John Wiley & Sons. pp. 213–.ISBN978-0-470-06171-8.OCLC1039172275.Archivedfrom the original on 29 May 2024.Retrieved18 September2022.
Diagnosis and treatment. The first diagnostic test [of PCOS] is measurement of total testosterone and free testosterone by radioimmunoassay. If total testosterone is between 50 ng/dL and 200 ng/dL above normal (<2.5 ng/dL) PCOS is present. If >200 ng/dL then serum DHEA-S should be measured. If total testosterone or DHEA-S >700 μg/dL then rule out an ovarian or adrenal tumor. These tests should be followed by tests for hypothyroidism, hyperprolactinemia, and adrenal hyperplasia.
- ^abLoh HH, Yee A, Loh HS, Kanagasundram S, Francis B, Lim LL (September 2020). "Sexual dysfunction in polycystic ovary syndrome: a systematic review and meta-analysis".Hormones (Athens).19(3): 413–423.doi:10.1007/s42000-020-00210-0.PMID32462512.S2CID218898082.
A total of 5366 women with PCOS from 21 studies were included. [...] Women with PCOS [...] [had higher] serum total testosterone level (2.34 ± 0.58 nmol/L vs 1.57 ± 0.60 nmol/L, p < 0.001) compared with women without PCOS. [...] PCOS is characterized by high levels of androgens (dehydroepiandrosterone, androstenedione, and testosterone) and luteinizing hormone (LH), and increased LH/follicle stimulating hormone (FSH) ratio [52].
- ^abBalen AH, Conway GS, Kaltsas G, Techatrasak K, Manning PJ, West C, et al. (August 1995). "Polycystic ovary syndrome: the spectrum of the disorder in 1741 patients".Hum Reprod.10(8): 2107–11.doi:10.1093/oxfordjournals.humrep.a136243.PMID8567849.
The criteria for the diagnosis of the polycystic ovary syndrome (PCOS) have still not been agreed universally. A population of 1741 women with PCOS were studied, all of whom had polycystic ovaries seen by ultrasound scan. The frequency distributions of the serum concentrations of [...] testosterone [...] were determined and compared with the symptoms and signs of PCOS. [...] A rising serum concentration of testosterone [mean and 95th percentiles 2.6 (1.1-4.8) nmol/1] was associated with an increased risk of hirsutism, infertility and cycle disturbance. [...] If the serum testosterone concentration is >4.8 nmol/1, other causes of hyperandrogenism should be excluded.
- ^Steinberger E, Ayala C, Hsi B, Smith KD, Rodriguez-Rigau LJ, Weidman ER, et al. (1998). "Utilization of commercial laboratory results in management of hyperandrogenism in women".Endocr Pract.4(1): 1–10.doi:10.4158/EP.4.1.1.PMID15251757.
- ^Legro RS, Schlaff WD, Diamond MP, Coutifaris C, Casson PR, Brzyski RG, et al. (December 2010)."Total testosterone assays in women with polycystic ovary syndrome: precision and correlation with hirsutism".J Clin Endocrinol Metab.95(12): 5305–13.doi:10.1210/jc.2010-1123.PMC2999971.PMID20826578.
Design and Setting: We conducted a blinded laboratory study including masked duplicate samples at three laboratories—two academic (University of Virginia, RIA; and Mayo Clinic, LC/MS) and one commercial (Quest, LC/MS). Participants and Interventions: Baseline testosterone levels from 596 women with PCOS who participated in a large, multicenter, randomized controlled infertility trial performed at academic health centers in the United States were run by varying assays, and results were compared. [...] The median testosterone level by RIA was 50 ng/dl (25th–75th percentile, 34–71 ng/dl); by LC/MS at Mayo, 47 ng/dl (25th–75th percentile, 34–65 ng/dl); and by LC/MS at Quest, 41 ng/dl (25th–75th percentile, 27–58 ng/dl) (Fig. 1). The minimum and maximum values detected by RIA were 8 and 189 ng/dl, respectively; by LC/MS at Mayo, 12 and 184 ng/dl, respectively; and by LC/MS at Quest, 1 and 205 ng/dl, respectively. [...] Our sample size was robust and the largest study to date examining quality control of total testosterone serum levels in women.
- ^Carmina E, Stanczyk FZ, Lobo RA (2019). "Evaluation of Hormonal Status". In Strauss JF, Barbieri RL (eds.).Yen and Jaffe's Reproductive Endocrinology: Physiology, Pathophysiology, and Clinical Management(8th ed.). Elsevier. pp. 887–915.e4.doi:10.1016/B978-0-323-47912-7.00034-2.ISBN978-0-323-47912-7.S2CID56977185.
- ^abcBarry JA, Azizia MM, Hardiman PJ (1 September 2014)."Risk of endometrial, ovarian and breast cancer in women with polycystic ovary syndrome: a systematic review and meta-analysis".Human Reproduction Update.20(5): 748–758.doi:10.1093/humupd/dmu012.PMC4326303.PMID24688118.
- ^New MI (May 1993). "Nonclassical congenital adrenal hyperplasia and the polycystic ovarian syndrome".Annals of the New York Academy of Sciences.687(1): 193–205.Bibcode:1993NYASA.687..193N.doi:10.1111/j.1749-6632.1993.tb43866.x.PMID8323173.S2CID30161989.
- ^Hardiman P, Pillay OC, Atiomo W (May 2003). "Polycystic ovary syndrome and endometrial carcinoma".Lancet.361(9371): 1810–1812.doi:10.1016/S0140-6736(03)13409-5.PMID12781553.S2CID27453081.
- ^Mather KJ, Kwan F, Corenblum B (January 2000)."Hyperinsulinemia in polycystic ovary syndrome correlates with increased cardiovascular risk independent of obesity".Fertility and Sterility.73(1): 150–156.doi:10.1016/S0015-0282(99)00468-9.PMID10632431.
- ^Moran LJ, Misso ML, Wild RA, Norman RJ (2010)."Impaired glucose tolerance, type 2 diabetes and metabolic syndrome in polycystic ovary syndrome: a systematic review and meta-analysis".Human Reproduction Update.16(4): 347–363.doi:10.1093/humupd/dmq001.PMID20159883.
- ^Falcone T, Hurd RW (2007).Clinical Reproductive Medicine and Surgery.Elsevier Health Sciences. p. 223.ISBN978-0-323-03309-1.Archivedfrom the original on 2023-01-14.Retrieved2020-05-24.
- ^"Polycystic ovary syndrome (PCOS) - Symptoms and causes".Mayo Clinic.Archivedfrom the original on 2021-11-21.Retrieved2021-06-26.
- ^Barry JA, Kuczmierczyk AR, Hardiman PJ (September 2011)."Anxiety and depression in polycystic ovary syndrome: a systematic review and meta-analysis".Human Reproduction.26(9): 2442–2451.doi:10.1093/humrep/der197.PMID21725075.
- ^Ovalle F, Azziz R (June 2002)."Insulin resistance, polycystic ovary syndrome, and type 2 diabetes mellitus".Fertility and Sterility.77(6): 1095–1105.doi:10.1016/s0015-0282(02)03111-4.PMID12057712.
- ^de Groot PC, Dekkers OM, Romijn JA, Dieben SW, Helmerhorst FM (1 July 2011)."PCOS, coronary heart disease, stroke and the influence of obesity: a systematic review and meta-analysis".Human Reproduction Update.17(4): 495–500.doi:10.1093/humupd/dmr001.PMID21335359.
- ^Goldenberg N, Glueck C (February 2008)."Medical therapy in women with polycystic ovarian syndrome before and during pregnancy and lactation".Minerva Ginecologica.60(1): 63–75.PMID18277353.Archivedfrom the original on 2021-11-02.Retrieved2021-10-13.
- ^Boomsma CM, Fauser BC, Macklon NS (January 2008). "Pregnancy complications in women with polycystic ovary syndrome".Seminars in Reproductive Medicine.26(1): 72–84.doi:10.1055/s-2007-992927.PMID18181085.S2CID260316768.
- ^"Iron Deficiency Injectables Market: Global Industry Trends, Share, Size, Growth, Opportunity and Forecast 2020-2025".imarc.Archivedfrom the original on 2023-08-02.Retrieved2023-08-02.
- ^abPage 836 (Section:Polycystic ovary syndrome) in:Fauser BC, Diedrich K, Bouchard P, Domínguez F, Matzuk M, Franks S, et al. (2011)."Contemporary genetic technologies and female reproduction".Human Reproduction Update.17(6): 829–847.doi:10.1093/humupd/dmr033.PMC3191938.PMID21896560.
- ^abcdLegro RS, Strauss JF (September 2002)."Molecular progress in infertility: polycystic ovary syndrome".Fertility and Sterility.78(3): 569–576.doi:10.1016/S0015-0282(02)03275-2.PMID12215335.
- ^Filippou P, Homburg R (July 2017)."Is foetal hyperexposure to androgens a cause of PCOS?".Human Reproduction Update.23(4): 421–432.doi:10.1093/humupd/dmx013.PMID28531286.
- ^Dumesic DA, Oberfield SE, Stener-Victorin E, Marshall JC, Laven JS, Legro RS (October 2015)."Scientific Statement on the Diagnostic Criteria, Epidemiology, Pathophysiology, and Molecular Genetics of Polycystic Ovary Syndrome".Endocrine Reviews(Review).36(5): 487–525.doi:10.1210/er.2015-1018.PMC4591526.PMID26426951.
- ^abCrosignani PG, Nicolosi AE (2001)."Polycystic ovarian disease: heritability and heterogeneity".Human Reproduction Update.7(1): 3–7.doi:10.1093/humupd/7.1.3.PMID11212071.
- ^abcStrauss JF (November 2003). "Some new thoughts on the pathophysiology and genetics of polycystic ovary syndrome".Annals of the New York Academy of Sciences.997(1): 42–48.Bibcode:2003NYASA.997...42S.doi:10.1196/annals.1290.005.PMID14644808.S2CID23559461.
- ^abHamosh A (12 September 2011)."POLYCYSTIC OVARY SYNDROME 1; PCOS1".OMIM.McKusick-Nathans Institute of Genetic Medicine, Johns Hopkins University School of Medicine.Archivedfrom the original on 16 July 2015.Retrieved15 November2011.
- ^Amato P, Simpson JL (October 2004). "The genetics of polycystic ovary syndrome".Best Practice & Research. Clinical Obstetrics & Gynaecology.18(5): 707–718.doi:10.1016/j.bpobgyn.2004.05.002.PMID15380142.
- ^Draper N, Walker EA, Bujalska IJ, Tomlinson JW, Chalder SM, Arlt W, et al. (August 2003). "Mutations in the genes encoding 11beta-hydroxysteroid dehydrogenase type 1 and hexose-6-phosphate dehydrogenase interact to cause cortisone reductase deficiency".Nature Genetics.34(4): 434–439.doi:10.1038/ng1214.PMID12858176.S2CID22772927.
- ^Ehrmann DA (March 2005). "Polycystic ovary syndrome".The New England Journal of Medicine.352(12): 1223–1236.doi:10.1056/NEJMra041536.PMID15788499.S2CID79796961.
- ^Faghfoori Z, Fazelian S, Shadnoush M, Goodarzi R (November 2017). "Nutritional management in women with polycystic ovary syndrome: A review study".Diabetes & Metabolic Syndrome(Review).11(Suppl 1): S429–S432.doi:10.1016/j.dsx.2017.03.030.PMID28416368.
- ^Witchel SF, Oberfield SE, Peña AS (August 2019)."Polycystic Ovary Syndrome: Pathophysiology, Presentation, and Treatment With Emphasis on Adolescent Girls".Journal of the Endocrine Society.3(8): 1545–1573.doi:10.1210/js.2019-00078.PMC6676075.PMID31384717.
- ^Hoeger KM (May 2014). "Developmental origins and future fate in PCOS".Seminars in Reproductive Medicine.32(3): 157–158.doi:10.1055/s-0034-1371086.PMID24715509.S2CID32069697.
- ^Abbott DH, Barnett DK, Bruns CM, Dumesic DA (2005)."Androgen excess fetal programming of female reproduction: a developmental aetiology for polycystic ovary syndrome?".Human Reproduction Update.11(4): 357–374.doi:10.1093/humupd/dmi013.PMID15941725.
- ^Rasgon N (June 2004). "The relationship between polycystic ovary syndrome and antiepileptic drugs: a review of the evidence".Journal of Clinical Psychopharmacology.24(3): 322–334.doi:10.1097/01.jcp.0000125745.60149.c6.PMID15118487.S2CID24603227.
- ^Rutkowska A, Rachoń D (April 2014). "Bisphenol A (BPA) and its potential role in the pathogenesis of the polycystic ovary syndrome (PCOS)".Gynecological Endocrinology.30(4): 260–265.doi:10.3109/09513590.2013.871517.PMID24397396.S2CID5828672.
- ^abPalioura E, Diamanti-Kandarakis E (December 2013). "Industrial endocrine disruptors and polycystic ovary syndrome".Journal of Endocrinological Investigation.36(11): 1105–1111.doi:10.1007/bf03346762.PMID24445124.S2CID27141519.
- ^Hu X, Wang J, Dong W, Fang Q, Hu L, Liu C (November 2011). "A meta-analysis of polycystic ovary syndrome in women taking valproate for epilepsy".Epilepsy Research.97(1–2): 73–82.doi:10.1016/j.eplepsyres.2011.07.006.PMID21820873.S2CID26422134.
- ^"Endocrine Disruptors".National Institute of Environmental Health Sciences.Archivedfrom the original on 2020-06-11.Retrieved2022-11-10.
- ^Merkin SS, Phy JL, Sites CK, Yang D (July 2016)."Environmental determinants of polycystic ovary syndrome".Fertility and Sterility.106(1): 16–24.doi:10.1016/j.fertnstert.2016.05.011.PMID27240194.
- ^abcdDiamanti-Kandarakis E, Dunaif A (December 2012)."Insulin resistance and the polycystic ovary syndrome revisited: an update on mechanisms and implications".Endocrine Reviews.33(6): 981–1030.doi:10.1210/er.2011-1034.PMC5393155.PMID23065822.
- ^Lewandowski KC, Cajdler-Łuba A, Salata I, Bieńkiewicz M, Lewiński A (2011)."The utility of the gonadotrophin releasing hormone (GnRH) test in the diagnosis of polycystic ovary syndrome (PCOS)".Endokrynologia Polska.62(2): 120–128.PMID21528473.ProQuest2464206947.Archivedfrom the original on 2021-10-27.Retrieved2021-10-13.
- ^Rojas J, Chávez M, Olivar L, Rojas M, Morillo J, Mejías J, et al. (2014)."Polycystic ovary syndrome, insulin resistance, and obesity: navigating the pathophysiologic labyrinth".Int J Reprod Med.2014:71905.doi:10.1155/2014/719050.PMC4334071.PMID25763405.
- ^Ali HI, Elsadawy ME, Khater NH (March 2016)."Ultrasound assessment of polycystic ovaries: Ovarian volume and morphology; which is more accurate in making the diagnosis?!".The Egyptian Journal of Radiology and Nuclear Medicine.47(1): 347–350.doi:10.1016/j.ejrnm.2015.10.002.
- ^Sathyapalan T, Atkin SL (2010)."Mediators of inflammation in polycystic ovary syndrome in relation to adiposity".Mediators of Inflammation.2010:758656.doi:10.1155/2010/758656.PMC2852606.PMID20396393.
- ^Fukuoka M, Yasuda K, Fujiwara H, Kanzaki H, Mori T (November 1992). "Interactions between interferon gamma, tumour necrosis factor alpha, and interleukin-1 in modulating progesterone and oestradiol production by human luteinized granulosa cells in culture".Human Reproduction.7(10): 1361–1364.doi:10.1093/oxfordjournals.humrep.a137574.PMID1291559.
- ^González F, Rote NS, Minium J, Kirwan JP (January 2006)."Reactive oxygen species-induced oxidative stress in the development of insulin resistance and hyperandrogenism in polycystic ovary syndrome".The Journal of Clinical Endocrinology and Metabolism.91(1): 336–340.doi:10.1210/jc.2005-1696.PMID16249279.
- ^Murri M, Luque-Ramírez M, Insenser M, Ojeda-Ojeda M, Escobar-Morreale HF (2013)."Circulating markers of oxidative stress and polycystic ovary syndrome (PCOS): a systematic review and meta-analysis".Human Reproduction Update.19(3): 268–288.doi:10.1093/humupd/dms059.PMID23303572.
- ^abcdImaging in Polycystic Ovary DiseaseateMedicine
- ^Lujan ME, Chizen DR, Pierson RA (August 2008)."Diagnostic criteria for polycystic ovary syndrome: pitfalls and controversies".Journal of Obstetrics and Gynaecology Canada.30(8): 671–679.doi:10.1016/S1701-2163(16)32915-2.PMC2893212.PMID18786289.
- ^abcdefPolycystic Ovarian Syndrome~workupateMedicine
- ^Pedersen SD, Brar S, Faris P, Corenblum B (June 2007)."Polycystic ovary syndrome: validated questionnaire for use in diagnosis".Canadian Family Physician.53(6): 1042–7, 1041.PMC1949220.PMID17872783.
- ^abDewailly D, Lujan ME, Carmina E, Cedars MI, Laven J, Norman RJ, et al. (2013)."Definition and significance of polycystic ovarian morphology: a task force report from the Androgen Excess and Polycystic Ovary Syndrome Society".Human Reproduction Update.20(3): 334–352.doi:10.1093/humupd/dmt061.PMID24345633.
- ^O'Brien WT (1 January 2011).Top 3 Differentials in Radiology.Thieme. p. 369.ISBN978-1-60406-228-1.Archivedfrom the original on 19 April 2016.Retrieved30 August2014.
Ultrasound findings in PCOS include enlarged ovaries with peripheral follicles in a "string of pearls" configuration.
- ^Bordewijk EM, Ng KY, Rakic L, Mol BW, Brown J, Crawford TJ, et al. (February 2020)."Laparoscopic ovarian drilling for ovulation induction in women with anovulatory polycystic ovary syndrome".The Cochrane Database of Systematic Reviews.2(2): CD001122.doi:10.1002/14651858.CD001122.pub5.PMC7013239.PMID32048270.
- ^Somani N, Harrison S, Bergfeld WF (2008). "The clinical evaluation of hirsutism".Dermatologic Therapy.21(5): 376–391.doi:10.1111/j.1529-8019.2008.00219.x.PMID18844715.S2CID34029116.
- ^Sharquie KE, Al-Bayatti AA, Al-Ajeel AI, Al-Bahar AJ, Al-Nuaimy AA (July 2007). "Free testosterone, luteinizing hormone/follicle stimulating hormone ratio and pelvic sonography in relation to skin manifestations in patients with polycystic ovary syndrome".Saudi Medical Journal.28(7): 1039–1043.OCLC151296412.PMID17603706.INIST18933286.
- ^abBanaszewska B, Spaczyński RZ, Pelesz M, Pawelczyk L (2003). "Incidence of elevated LH/FSH ratio in polycystic ovary syndrome women with normo- and hyperinsulinemia".Roczniki Akademii Medycznej W Bialymstoku.48:131–134.CiteSeerX10.1.1.410.676.PMID14737959.
- ^Macpherson G (2002).Black's Medical Dictionary(40 ed.). Lanham, MD: Scarecrow Press. p. 496.ISBN0-8108-4984-4.
- ^Dumont A, Robin G, Catteau-Jonard S, Dewailly D (December 2015)."Role of Anti-Müllerian Hormone in pathophysiology, diagnosis and treatment of Polycystic Ovary Syndrome: a review".Reproductive Biology and Endocrinology(Review).13:137.doi:10.1186/s12958-015-0134-9.PMC4687350.PMID26691645.
- ^Dewailly D, Andersen CY, Balen A, Broekmans F, Dilaver N, Fanchin R, et al. (2014)."The physiology and clinical utility of anti-Mullerian hormone in women".Human Reproduction Update(Review).20(3): 370–385.doi:10.1093/humupd/dmt062.hdl:10023/7488.PMID24430863.
- ^Broer SL, Broekmans FJ, Laven JS, Fauser BC (2014)."Anti-Müllerian hormone: ovarian reserve testing and its potential clinical implications".Human Reproduction Update.20(5): 688–701.doi:10.1093/humupd/dmu020.PMID24821925.
- ^Andersen M, Glintborg D (September 2018)."Diagnosis and follow-up of type 2 diabetes in women with PCOS: a role for OGTT?".European Journal of Endocrinology.179(3): D1–D14.doi:10.1530/EJE-18-0237.PMID29921567.S2CID49315075.
- ^Muniyappa R, Madan R, Varghese RT (2000)."Assessing Insulin Sensitivity and Resistance in Humans".In Feingold KR, Anawalt B, Boyce A, Chrousos G (eds.).Endotext.South Dartmouth (MA): MDText.com, Inc.PMID25905189.Archivedfrom the original on 2022-06-16.Retrieved2022-10-19.
- ^abcdadmin (2022-06-20)."What Are The Four Types of PCOs?".Ferticity IVF & Fertility Clinics.Retrieved2024-05-29.
- ^abcDiamanti-Kandarakis E, ed. (2022).Polycystic Ovary Syndrome.doi:10.1016/c2018-0-03276-4.ISBN978-0-12-823045-9.S2CID222263507.Archivedfrom the original on 2024-05-29.Retrieved2023-08-22.
- ^abNational Institutes of Health (NIH)(2014-07-14)."Treatments for Infertility Resulting from PCOS".Archivedfrom the original on 2 April 2015.Retrieved13 March2015.
- ^abLegro RS, Arslanian SA, Ehrmann DA, Hoeger KM, Murad MH, Pasquali R, et al. (December 2013)."Diagnosis and treatment of polycystic ovary syndrome: an Endocrine Society clinical practice guideline".The Journal of Clinical Endocrinology and Metabolism.98(12): 4565–4592.doi:10.1210/jc.2013-2350.PMC5399492.PMID24151290.
- ^Magkos F, Yannakoulia M, Chan JL, Mantzoros CS (2009)."Management of the metabolic syndrome and type 2 diabetes through lifestyle modification".Annual Review of Nutrition.29:223–256.doi:10.1146/annurev-nutr-080508-141200.PMC5653262.PMID19400751.
- ^Veltman-Verhulst SM, Boivin J, Eijkemans MJ, Fauser BJ (2012)."Emotional distress is a common risk in women with polycystic ovary syndrome: a systematic review and meta-analysis of 28 studies".Human Reproduction Update.18(6): 638–651.doi:10.1093/humupd/dms029.PMID22824735.
- ^Garvey WT, Mechanick JI, Brett EM, Garber AJ, Hurley DL, Jastreboff AM, et al. (Reviewers of the AACE/ACE Obesity Clinical Practice Guidelines) (July 2016)."American association of clinical endocrinologists and American college of endocrinology comprehensive clinical practice guidelines for medical care of patients with obesity".Endocrine Practice.22(Suppl 3): 1–203.doi:10.4158/EP161365.GL.PMID27219496.
- ^abMoran LJ, Ko H, Misso M, Marsh K, Noakes M, Talbot M, et al. (2013)."Dietary composition in the treatment of polycystic ovary syndrome: a systematic review to inform evidence-based guidelines".Human Reproduction Update.19(5): 432.doi:10.1093/humupd/dmt015.PMID23727939.
- ^abcdefghijkPolycystic Ovarian Syndrome~treatmentateMedicine
- ^Krul-Poel YH, Snackey C, Louwers Y, Lips P, Lambalk CB, Laven JS, et al. (December 2013)."The role of vitamin D in metabolic disturbances in polycystic ovary syndrome: a systematic review".European Journal of Endocrinology(Review).169(6): 853–865.doi:10.1530/EJE-13-0617.PMID24044903.
- ^He C, Lin Z, Robb SW, Ezeamama AE (2015)."Serum Vitamin D Levels and Polycystic Ovary syndrome: A Systematic Review and Meta-Analysis".Nutrients.7(6): 4555–4577.doi:10.3390/nu7064555.PMC4488802.PMID26061015.
- ^Huang G, Coviello A (December 2012). "Clinical update on screening, diagnosis and management of metabolic disorders and cardiovascular risk factors associated with polycystic ovary syndrome".Current Opinion in Endocrinology, Diabetes and Obesity.19(6): 512–519.doi:10.1097/med.0b013e32835a000e.PMID23108199.S2CID205792902.
- ^Alesi S, Forslund M, Melin J, Romualdi D, Peña A, Tay CT, et al. (September 2023)."Efficacy and safety of anti-androgens in the management of polycystic ovary syndrome: a systematic review and meta-analysis of randomised controlled trials".eClinicalMedicine.63:102162.doi:10.1016/j.eclinm.2023.102162.PMC10424142.PMID37583655.
- ^Lord JM, Flight IH, Norman RJ (October 2003)."Metformin in polycystic ovary syndrome: systematic review and meta-analysis".BMJ.327(7421): 951–953.doi:10.1136/bmj.327.7421.951.PMC259161.PMID14576245.
- ^Li XJ, Yu YX, Liu CQ, Zhang W, Zhang HJ, Yan B, et al. (March 2011). "Metformin vs thiazolidinediones for treatment of clinical, hormonal and metabolic characteristics of polycystic ovary syndrome: a meta-analysis".Clinical Endocrinology.74(3): 332–339.doi:10.1111/j.1365-2265.2010.03917.x.PMID21050251.S2CID19620846.
- ^Grover A, Yialamas MA (March 2011). "Metformin or thiazolidinedione therapy in PCOS?".Nature Reviews. Endocrinology.7(3): 128–129.doi:10.1038/nrendo.2011.16.PMID21283123.S2CID26162421.GaleA250471047.
- ^National Institute for Health and Clinical Excellence.11 Clinical guideline 11: Fertility: assessment and treatment for people with fertility problems.London, 2004.
- ^Balen A (December 2008)."Metformin therapy for the management of infertility in women with polycystic ovary syndrome"(PDF).Scientific Advisory Committee Opinion Paper 13.Royal College of Obstetricians and Gynaecologists. Archived fromthe original(PDF)on 2009-12-18.Retrieved2009-12-13.
- ^Leeman L, Acharya U (August 2009). "The use of metformin in the management of polycystic ovary syndrome and associated anovulatory infertility: the current evidence".Journal of Obstetrics and Gynaecology.29(6): 467–472.doi:10.1080/01443610902829414.PMID19697191.S2CID3339588.
- ^NICE (December 2018)."Metformin Hydrochloride".National Institute for Care Excellence.NICE.Archivedfrom the original on 2021-06-10.Retrieved2017-11-02.
- ^Feig DS, Moses RG (October 2011)."Metformin therapy during pregnancy: good for the goose and good for the gosling too?".Diabetes Care.34(10): 2329–2330.doi:10.2337/dc11-1153.PMC3177745.PMID21949224.
- ^Cassina M, Donà M, Di Gianantonio E, Litta P, Clementi M (1 September 2014)."First-trimester exposure to metformin and risk of birth defects: a systematic review and meta-analysis".Human Reproduction Update.20(5): 656–669.doi:10.1093/humupd/dmu022.PMID24861556.
- ^Wang FF, Wu Y, Zhu YH, Ding T, Batterham RL, Qu F, et al. (October 2018)."Pharmacologic therapy to induce weight loss in women who have obesity/overweight with polycystic ovary syndrome: a systematic review and network meta-analysis"(PDF).Obesity Reviews.19(10): 1424–1445.doi:10.1111/obr.12720.PMID30066361.S2CID51891552.Archived(PDF)from the original on 2021-12-03.Retrieved2021-10-13.
- ^Sharpe A, Morley LC, Tang T, Norman RJ, Balen AH (December 2019)."Metformin for ovulation induction (excluding gonadotrophins) in women with polycystic ovary syndrome".The Cochrane Database of Systematic Reviews.2019(12): CD013505.doi:10.1002/14651858.CD013505.PMC6915832.PMID31845767.
- ^"Erase the Dread and Stigma of PCOD".Matria.Archivedfrom the original on 2022-01-19.Retrieved2022-01-19.
- ^Balen AH, Morley LC, Misso M, Franks S, Legro RS, Wijeyaratne CN, et al. (November 2016). "The management of anovulatory infertility in women with polycystic ovary syndrome: an analysis of the evidence to support the development of global WHO guidance".Human Reproduction Update.22(6): 687–708.doi:10.1093/humupd/dmw025.PMID27511809.
- ^Qiao J, Feng HL (2010)."Extra- and intra-ovarian factors in polycystic ovary syndrome: impact on oocyte maturation and embryo developmental competence".Human Reproduction Update.17(1): 17–33.doi:10.1093/humupd/dmq032.PMC3001338.PMID20639519.
- ^"What are some causes of female infertility?".National Institute of Child Health and Human Development, National Institutes of Health.31 January 2017.Archivedfrom the original on 8 August 2020.Retrieved25 October2019.
- ^Jurczewska J, Szostak-Węgierek D (April 2022)."The Influence of Diet on Ovulation Disorders in Women-A Narrative Review".Nutrients.14(8): 1556.doi:10.3390/nu14081556.PMC9029579.PMID35458118.
- ^Wang L, Liu Y, Tan H, Huang S (May 2022)."Transtheoretical model-based mobile health application for PCOS".Reproductive Health.19(1): 117.doi:10.1186/s12978-022-01422-w.PMC9097413.PMID35549736.
- ^Franik S, Le QK, Kremer JA, Kiesel L, Farquhar C (September 2022)."Aromatase inhibitors (letrozole) for ovulation induction in infertile women with polycystic ovary syndrome".The Cochrane Database of Systematic Reviews.2022(9): CD010287.doi:10.1002/14651858.CD010287.pub4.PMC9514207.PMID36165742.
- ^Tanbo T, Mellembakken J, Bjercke S, Ring E, Åbyholm T, Fedorcsak P (October 2018)."Ovulation induction in polycystic ovary syndrome".Acta Obstetricia et Gynecologica Scandinavica.97(10): 1162–1167.doi:10.1111/aogs.13395.hdl:10852/72989.PMID29889977.
- ^Hu S, Yu Q, Wang Y, Wang M, Xia W, Zhu C (May 2018). "Letrozole versus clomiphene citrate in polycystic ovary syndrome: a meta-analysis of randomized controlled trials".Archives of Gynecology and Obstetrics.297(5): 1081–1088.doi:10.1007/s00404-018-4688-6.PMID29392438.S2CID4800270.
- ^Penzias A, Bendikson K, Butts S, Coutifaris C, Falcone T, Fossum G, et al. (September 2017)."Role of metformin for ovulation induction in infertile patients with polycystic ovary syndrome (PCOS): a guideline".Fertility and Sterility.108(3): 426–441.doi:10.1016/j.fertnstert.2017.06.026.PMID28865539.
- ^Legro RS, Barnhart HX, Schlaff WD, Carr BR, Diamond MP, Carson SA, et al. (February 2007)."Clomiphene, metformin, or both for infertility in the polycystic ovary syndrome".The New England Journal of Medicine.356(6): 551–566.doi:10.1056/NEJMoa063971.PMID17287476.[non-primary source needed]
- ^Homburg R (October 2004). "Management of infertility and prevention of ovarian hyperstimulation in women with polycystic ovary syndrome".Best Practice & Research. Clinical Obstetrics & Gynaecology.18(5): 773–788.doi:10.1016/j.bpobgyn.2004.05.006.PMID15380146.
- ^Ghanem ME, Elboghdady LA, Hassan M, Helal AS, Gibreel A, Houssen M, et al. (November 2013)."Clomiphene citrate co-treatment with low dose urinary FSH versus urinary FSH for clomiphene resistant PCOS: randomized controlled trial".Journal of Assisted Reproduction and Genetics.30(11): 1477–1485.doi:10.1007/s10815-013-0090-2.PMC3879942.PMID24014214.
- ^Smarasinghe SS (June 8, 2024)."Bariatric surgery for spontaneous ovulation in women living with polycystic ovary syndrome: the BAMBINI multicentre, open-label, randomised controlled trial".The Lancet.403(10443): 2489–2503.doi:10.1016/S0140-6736(24)00538-5.PMID38782004.
- ^abBerni TR, Morgan CL, Berni ER, Rees DA (June 2018). "Polycystic Ovary Syndrome Is Associated With Adverse Mental Health and Neurodevelopmental Outcomes".The Journal of Clinical Endocrinology and Metabolism.103(6): 2116–2125.doi:10.1210/jc.2017-02667.PMID29648599.
- ^Ee C, Pirotta S, Mousa A, Moran L, Lim S (November 2021)."Providing lifestyle advice to women with PCOS: an overview of practical issues affecting success".BMC Endocrine Disorders.21(1): 234.doi:10.1186/s12902-021-00890-8.PMC8609880.PMID34814919.
- ^Fraison E, Kostova E, Moran LJ, Bilal S, Ee CC, Venetis C, et al. (August 2020)."Metformin versus the combined oral contraceptive pill for hirsutism, acne, and menstrual pattern in polycystic ovary syndrome".The Cochrane Database of Systematic Reviews.2020(8): CD005552.doi:10.1002/14651858.CD005552.pub3.PMC7437400.PMID32794179.
- ^"Polycystic ovary syndrome – Treatment".United Kingdom: National Health Service. 17 October 2011.Archivedfrom the original on 6 November 2011.Retrieved19 November2011.
- ^abPolycystic Ovarian Syndrome~medicationateMedicine
- ^van Zuuren EJ, Fedorowicz Z, Carter B, Pandis N (April 2015)."Interventions for hirsutism (excluding laser and photoepilation therapy alone)".The Cochrane Database of Systematic Reviews.2015(4): CD010334.doi:10.1002/14651858.CD010334.pub2.PMC6481758.PMID25918921.
- ^"Irregular periods - NHS".Nhs.uk. 2020-10-21.Archivedfrom the original on 2022-07-19.Retrieved2022-07-19.
- ^"What are the health risks of PCOS?".Verity – PCOS Charity.Verity. 2011. Archived fromthe originalon 25 December 2012.Retrieved21 November2011.
- ^Pundir J, Psaroudakis D, Savnur P, Bhide P, Sabatini L, Teede H, et al. (February 2018)."Inositol treatment of anovulation in women with polycystic ovary syndrome: a meta-analysis of randomised trials"(PDF).BJOG.125(3): 299–308.doi:10.1111/1471-0528.14754.PMID28544572.S2CID21090113.Archived(PDF)from the original on 2021-10-24.Retrieved2021-10-13.
- ^Amoah-Arko A, Evans M, Rees A (20 October 2017). "Effects of myoinositol and D-chiro inositol on hyperandrogenism and ovulation in women with polycystic ovary syndrome: a systematic review".Endocrine Abstracts.doi:10.1530/endoabs.50.P363.
- ^Unfer V, Carlomagno G, Dante G, Facchinetti F (July 2012). "Effects of myo-inositol in women with PCOS: a systematic review of randomized controlled trials".Gynecological Endocrinology.28(7): 509–515.doi:10.3109/09513590.2011.650660.PMID22296306.S2CID24582338.
- ^Zeng L, Yang K (January 2018). "Effectiveness of myoinositol for polycystic ovary syndrome: a systematic review and meta-analysis".Endocrine.59(1): 30–38.doi:10.1007/s12020-017-1442-y.PMID29052180.S2CID4376339.
- ^Laganà AS, Vitagliano A, Noventa M, Ambrosini G, D'Anna R (October 2018). "Myo-inositol supplementation reduces the amount of gonadotropins and length of ovarian stimulation in women undergoing IVF: a systematic review and meta-analysis of randomized controlled trials".Archives of Gynecology and Obstetrics.298(4): 675–684.doi:10.1007/s00404-018-4861-y.PMID30078122.S2CID51921158.
- ^Galazis N, Galazi M, Atiomo W (April 2011). "D-Chiro-inositol and its significance in polycystic ovary syndrome: a systematic review".Gynecological Endocrinology.27(4): 256–262.doi:10.3109/09513590.2010.538099.PMID21142777.S2CID1989262.
- ^Lim CE, Ng RW, Cheng NC, Zhang GS, Chen H (July 2019)."Acupuncture for polycystic ovarian syndrome".The Cochrane Database of Systematic Reviews.2019(7): CD007689.doi:10.1002/14651858.CD007689.pub4.PMC6603768.PMID31264709.
- ^Wu XK, Stener-Victorin E, Kuang HY, Ma HL, Gao JS, Xie LZ, et al. (June 2017)."Effect of Acupuncture and Clomiphene in Chinese Women With Polycystic Ovary Syndrome: A Randomized Clinical Trial".JAMA.317(24): 2502–2514.doi:10.1001/jama.2017.7217.PMC5815063.PMID28655015.
- ^abcKovacs GT, Norman R (2007-02-22).Polycystic Ovary Syndrome.Cambridge University Press. p. 4.ISBN978-1-139-46203-7.Archivedfrom the original on 16 June 2013.Retrieved29 March2013.
- ^Vos T, Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, et al. (December 2012)."Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010".Lancet.380(9859): 2163–2196.doi:10.1016/S0140-6736(12)61729-2.PMC6350784.PMID23245607.
- ^McLuskie I, Newth A (January 2017). "New diagnosis of polycystic ovary syndrome".BMJ.356:i6456.doi:10.1136/bmj.i6456.hdl:10044/1/44217.PMID28082338.S2CID13042313.
- ^Pruthi B (26 September 2019)."One in five Indian women suffers from PCOS".The Hindu.Archivedfrom the original on 15 April 2021.RetrievedApril 16,2021.
- ^Ladson G, Dodson WC, Sweet SD, Archibong AE, Kunselman AR, Demers LM, et al. (July 2011)."Racial influence on the polycystic ovary syndrome phenotype: a black and white case-control study".Fertility and Sterility.96(1): 224–229.e2.doi:10.1016/j.fertnstert.2011.05.002.PMC3132396.PMID21723443.
- ^Hillman JK, Johnson LN, Limaye M, Feldman RA, Sammel M, Dokras A (September 2013)."Black women with polycystic ovary syndrome (PCOS) have increased risk for metabolic syndrome (MET SYN) and cardiovascular disease (CVD) compared to white women with PCOS".Fertility and Sterility.100(3): S100–S101.doi:10.1016/j.fertnstert.2013.07.1707.
- ^Elghobashy M, Lau GM, Davitadze M, Gillett CD, O'Reilly MW, Arlt W, et al. (2023)."Concerns and expectations in women with polycystic ovary syndrome vary across age and ethnicity: findings from PCOS Pearls Study".Frontiers in Endocrinology.14:1175548.doi:10.3389/fendo.2023.1175548.PMC10446892.PMID37621648.
- ^"Recommendations from the 2023 International Evidence-based Guideline for the Assessment and Management of Polycystic Ovary Syndrome (2023)".www.asrm.org.Archivedfrom the original on 2023-11-26.Retrieved2023-11-26.
- ^Polson DW, Adams J, Wadsworth J, Franks S (April 1988). "Polycystic ovaries--a common finding in normal women".Lancet.1(8590): 870–872.doi:10.1016/s0140-6736(88)91612-1.PMID2895373.S2CID41297081.
- ^abClayton RN, Ogden V, Hodgkinson J, Worswick L, Rodin DA, Dyer S, et al. (August 1992). "How common are polycystic ovaries in normal women and what is their significance for the fertility of the population?".Clinical Endocrinology.37(2): 127–134.doi:10.1111/j.1365-2265.1992.tb02296.x.PMID1395063.S2CID12384062.
- ^Farquhar CM, Birdsall M, Manning P, Mitchell JM, France JT (February 1994). "The prevalence of polycystic ovaries on ultrasound scanning in a population of randomly selected women".The Australian & New Zealand Journal of Obstetrics & Gynaecology.34(1): 67–72.doi:10.1111/j.1479-828X.1994.tb01041.x.PMID8053879.S2CID312422.
- ^van Santbrink EJ, Hop WC, Fauser BC (March 1997)."Classification of normogonadotropic infertility: polycystic ovaries diagnosed by ultrasound versus endocrine characteristics of polycystic ovary syndrome".Fertility and Sterility.67(3): 452–458.doi:10.1016/S0015-0282(97)80068-4.PMID9091329.
- ^Hardeman J, Weiss BD (March 2014). "Intrauterine devices: an update".American Family Physician.89(6): 445–450.PMID24695563.
- ^Chahal N, Quinn M, Jaswa EA, Kao CN, Cedars MI, Huddleston HG (December 2020)."Comparison of metabolic syndrome elements in White and Asian women with polycystic ovary syndrome: results of a regional, American cross-sectional study".F&S Reports.1(3): 305–313.doi:10.1016/j.xfre.2020.09.008.PMC8244318.PMID34223261.
- ^Azziz R, Marin C, Hoq L, Badamgarav E, Song P (August 2005)."Health care-related economic burden of the polycystic ovary syndrome during the reproductive life span".The Journal of Clinical Endocrinology and Metabolism.90(8): 4650–4658.doi:10.1210/jc.2005-0628.PMID15944216.
- ^"RCDC Estimates of Funding for Various Research, Condition, and Disease Categories (RCDC)".NIH.Archived fromthe originalon 28 February 2019.Retrieved3 December2018.
- ^abChaudhari AP, Mazumdar K, Mehta PD (2018)."Anxiety, Depression, and Quality of Life in Women with Polycystic Ovarian Syndrome".Indian Journal of Psychological Medicine.40(3): 239–246.doi:10.4103/IJPSYM.IJPSYM_561_17.PMC5968645.PMID29875531.
- ^"Sarah Hall investigates polycystic ovary syndrome".The Guardian.2002-02-28.Archivedfrom the original on 2024-05-29.Retrieved2022-01-21.
- ^Migdol E."'Teen Mom' Star Nails the 'Lose-Lose' Side of Chronic Illness Doctors Don't Always Get ".The Mighty.Archivedfrom the original on 2022-01-19.Retrieved2022-11-14.
- ^"All the celebrities who've opened up about life with Polycystic Ovary Syndrome".Cosmopolitan.26 November 2021.Archivedfrom the original on 2022-09-01.Retrieved2022-09-01.
- ^Chowdhury J."What Every Woman Should Know About PCOS".www.refinery29.com.Archivedfrom the original on 2022-01-21.Retrieved2022-01-21.
- ^"Actress Jaime King on her investment in Allara, a chronic care platform for women".Fortune.Archivedfrom the original on 2022-09-01.Retrieved2022-09-01.
- ^"Chrisette Michele Opens Up About Living With PCOS & No Longer Being Vegan - BlackDoctor.org - Where Wellness & Culture Connect".BlackDoctor.org.2015-12-10.Archivedfrom the original on 2022-01-22.Retrieved2022-01-22.
- ^"Lea Michele On How PCOS Changed Her Relationship With Food: 'The Side Effects Can Be Brutal'".Health Magazine.Archived fromthe originalon 2022-09-01.Retrieved2022-09-01.
- ^Natale N (2021-11-17)."Keke Palmer Says PCOS Causes Facial Hair and Adult Acne".Prevention.Archivedfrom the original on 2022-01-21.Retrieved2022-01-21.
- ^Seemayer Z (September 26, 2017)."Sasha Pieterse Tears Up Over Health Problems, Opens Up About Losing 15 Pounds Since Joining 'DWTS'".Entertainment Tonight.Archivedfrom the original on October 10, 2017.RetrievedSeptember 27,2017.
- ^Mizoguchi K, Stern AB (October 5, 2017)."Sasha Pieterse Wows on People's Ones to Watch Red Carpet as She Reveals Why She's 'So Thankful to DWTS'".people.com.Archivedfrom the original on 2021-12-11.Retrieved2021-12-11.
- ^"'Star Wars: The Force Awakens' Actress Opens Up About Painful Disorder ".ABC News.Archivedfrom the original on 2022-01-21.Retrieved2022-01-21.
- ^"Romee Strijd's Pregnancy Announcement Comes With an Honest Message About Reproductive Health".Vogue.29 May 2020.Archivedfrom the original on 2022-09-01.Retrieved2022-09-01.
- ^Silman A (March 10, 2020)."Lee's American Dream".The Cut.New York Media.Archivedfrom the original on April 12, 2023.RetrievedApril 12,2023.
Further reading
[edit]- Bremer AA (October 2010)."Polycystic ovary syndrome in the pediatric population".Metabolic Syndrome and Related Disorders.8(5): 375–394.doi:10.1089/met.2010.0039.PMC3125559.PMID20939704.
- "Polycystic Ovary Syndrome (PCOS)".Eunice Kennedy Shriver National Institute of Child Health and Human Development.31 January 2017.Archivedfrom the original on 22 October 2018.Retrieved19 November2018.
External links
[edit] Media related toPolycystic ovary syndromeat Wikimedia Commons
Media related toPolycystic ovary syndromeat Wikimedia Commons