Calcifediol

| |

| |
| Names | |
|---|---|
| Preferred IUPAC name
(1S,3Z)-3-[(2E)-2-{(1R,3aS,7aR)-1-[(2R)-6-Hydroxy-6-methylheptan-2-yl]-7a-methyloctahydro-4H-inden-4-ylidene}ethylidene]-4-methylidenecyclohexan-1-ol | |
| Other names | |
| Identifiers | |
3D model (JSmol)
|
|
| ChEBI | |
| ChEMBL | |
| ChemSpider | |
| DrugBank | |
| ECHA InfoCard | 100.039.067 |
| KEGG | |
| MeSH | Calcifediol |
PubChemCID
|
|
| UNII | |
CompTox Dashboard(EPA)
|
|
| |
| |
| Properties | |
| C27H44O2 | |
| Molar mass | 400.64 g/mol |
| Pharmacology | |
| H05BX05(WHO) | |
| Legal status | |
Except where otherwise noted, data are given for materials in theirstandard state(at 25 °C [77 °F], 100 kPa).
| |
Calcifediol,also known ascalcidiol,25-hydroxycholecalciferol,or25-hydroxyvitamin D3(abbreviated25(OH)D3),[1]is a form ofvitamin Dproduced in theliverbyhydroxylationofvitamin D3(cholecalciferol) by the enzymevitamin D 25-hydroxylase.[3][4][5]Calcifediol can be further hydroxylated by theenzyme25(OH)D-1α-hydroxylase,primarily in the kidney, to formcalcitriol(1,25-(OH)2D3), which is the active hormonal form of vitamin D.[3][4][5]
Calcifediol is strongly bound in blood by thevitamin D-binding protein.[5]Measurement of serum calcifediol is the usual test performed to determine a person's vitamin D status, to showvitamin D deficiencyor sufficiency.[4][5]Calcifediol is available as an oral medication in some countries to supplement vitamin D status.[4][6][7]
Biology[edit]
Calcifediol is the precursor for calcitriol, the active form of vitamin D.[3][4]It is synthesized in the liver, by hydroxylation of cholecalciferol (vitamin D3) at the 25-position.[3]This enzymatic 25-hydroxylase reaction is mostly due to the actions ofCYP2R1,present inmicrosomes,although other enzymes such asmitochondrialCYP27A1can contribute.[5][8]Variations in the expression and activity of CYP2R1, such as low levels inobesity,affect circulating calcifediol.[8]Similarly, vitamin D2,ergocalciferol,can also be 25-hydroxylated to form 25-hydroxyergocalciferol, (ercalcidiol, 25(OH)D2);[1]both forms are measured together in blood as 25(OH)D.[3][4]
At a typical intake of cholecalciferol (up to 2000 IU/day), conversion to calcifediol is rapid. When large doses are given (100,000 IU), it takes 7 days to reach peak calcifediol concentrations.[9]Calcifediol binds in the blood to vitamin D-binding protein (also known as gc-globulin) and is the main circulating vitamin D metabolite.[4][5]Calcifediol has anelimination half-lifeof around 15 to 30 days.[4][9]
Calcifediol is further hydroxylated at the 1- Alpha -position in the kidneys to form 1,25-(OH)2D3,calcitriol.[3][4]This enzymatic25(OH)D-1α-hydroxylasereaction is performed exclusively byCYP27B1,which is highly expressed in the kidneys where it is principally regulated byparathyroid hormone,but also byFGF23and calcitriol itself.[3][5][8]CYP27B1 is also expressed in a number of other tissues, includingmacrophages,monocytes,keratinocytes,placentaandparathyroid glandand extra-renal synthesis of calcitriol from calcifediol has been shown to have biological effects in these tissues.[8][10]
Calcifediol is also converted into24,25-dihydroxycholecalciferolby 24-hydroxylation.[3]This enzymatic reaction is performed byCYP24A1which is expressed in many vitamin D target tissues including kidney, and is induced by calcitriol.[5]This will inactivate calcitriol tocalcitroic acid,but 24,25-(OH)2D3may have some biological actions itself.[5]
Blood test for vitamin D deficiency[edit]
In medical practice, a blood test for 25-hydroxy-vitamin D, 25(OH)D, is used to determine an individual's vitamin D status.[11]The name 25(OH)D refers to any combination of calcifediol (25-hydroxy-cholecalciferol), derived from vitamin D3,and ercalcidiol (25-hydroxy-ergocalciferol),[1]derived from vitamin D2.The first of these (also known as 25-hydroxy vitamin D3) is made by the body, or is sourced from certain animal foods or cholecalciferol supplements. The second (25-hydroxy vitamin D2) is from certain vegetable foods or ergocalciferol supplements.[11]Clinical tests for 25(OH)D often measure the total level of both of these two compounds together, generally without differentiating.[12]
This measurement is considered the best indicator of overall vitamin D status.[11][13][14]US labs generally report 25(OH)D levels as ng/mL. Other countries use nmol/L. Multiply ng/mL by 2.5 to convert to nmol/L.[4]
This test can be used to diagnosevitamin D deficiency,and is performed in people with high risk for vitamin D deficiency, when the results of the test can be used to support beginning replacement therapy with vitamin D supplements.[4][15] Patients withosteoporosis,chronic kidney disease,malabsorption,obesity,and some other infections may be at greater risk for being vitamin D-deficient and so are more likely to have this test.[15]Although vitamin D deficiency is common in some populations including those living at higher latitudes or with limited sun exposure, the 25(OH)D test is not usually requested for the entire population.[15]Physicians may advise low risk patients to takeover-the-countervitamin D supplements in place of having screening.[15]
It is the mostsensitivemeasure, though experts have called for improved standardization and reproducibility across different laboratories.[4][13]According toMedlinePlus,the recommended range of 25(OH)D is 20 to 40 ng/mL (50 to 100 nmol/L) though they recognize many experts recommend 30 to 50 ng/mL (75 to 125 nmol/L).[11]The normal range varies widely depending on several factors, including age and geographic location. A broadreference rangeof 20 to 150 nmol/L (8-60 ng/mL) has also been suggested,[16]while other studies have defined levels below 80 nmol/L (32 ng/mL) as indicative of vitamin D deficiency.[17]
Increasing calcifediol levels up to levels of 80 nmol/L (32 ng/mL) are associated with increasing the fraction of calcium that is absorbed from the gut.[13]Urinary calcium excretion balances intestinal calcium absorption and does not increase with calcifediol levels up to ~400 nmol/L (160 ng/mL).[18]
Supplementation[edit]
Calcifediol supplements have been used in some studies to improve vitamin D status.[4]Indications for their use include vitamin D deficiency or insufficiency, refractory rickets (vitamin D resistant rickets),familial hypophosphatemia,hypoparathyroidism,hypocalcemia andrenal osteodystrophyand, with calcium, in primary or corticosteroid-inducedosteoporosis.[19]
Calcifediol may have advantages over cholecalciferol for the correction of vitamin D deficiency states.[6]A review of the results of ninerandomized control trialswhich compared oral doses of both, found that calcifediol was 3.2-fold more potent than cholecalciferol.[6]Calcifediol is better absorbed from the intestine and has greater affinity for the vitamin-D-binding protein, both of which increase its bioavailability.[20]Orally administered calcifediol has a much shorter half-life with faster elimination.[20]These properties may be beneficial in people with intestinalmalabsorption,obesity, or treated with certain other medications.[20]
In 2016, the FDA approved a formulation of calcifediol (Rayaldee) 60 microgram daily as a prescription medication to treat secondaryhyperparathyroidismin patients withchronic kidney disease.[7]
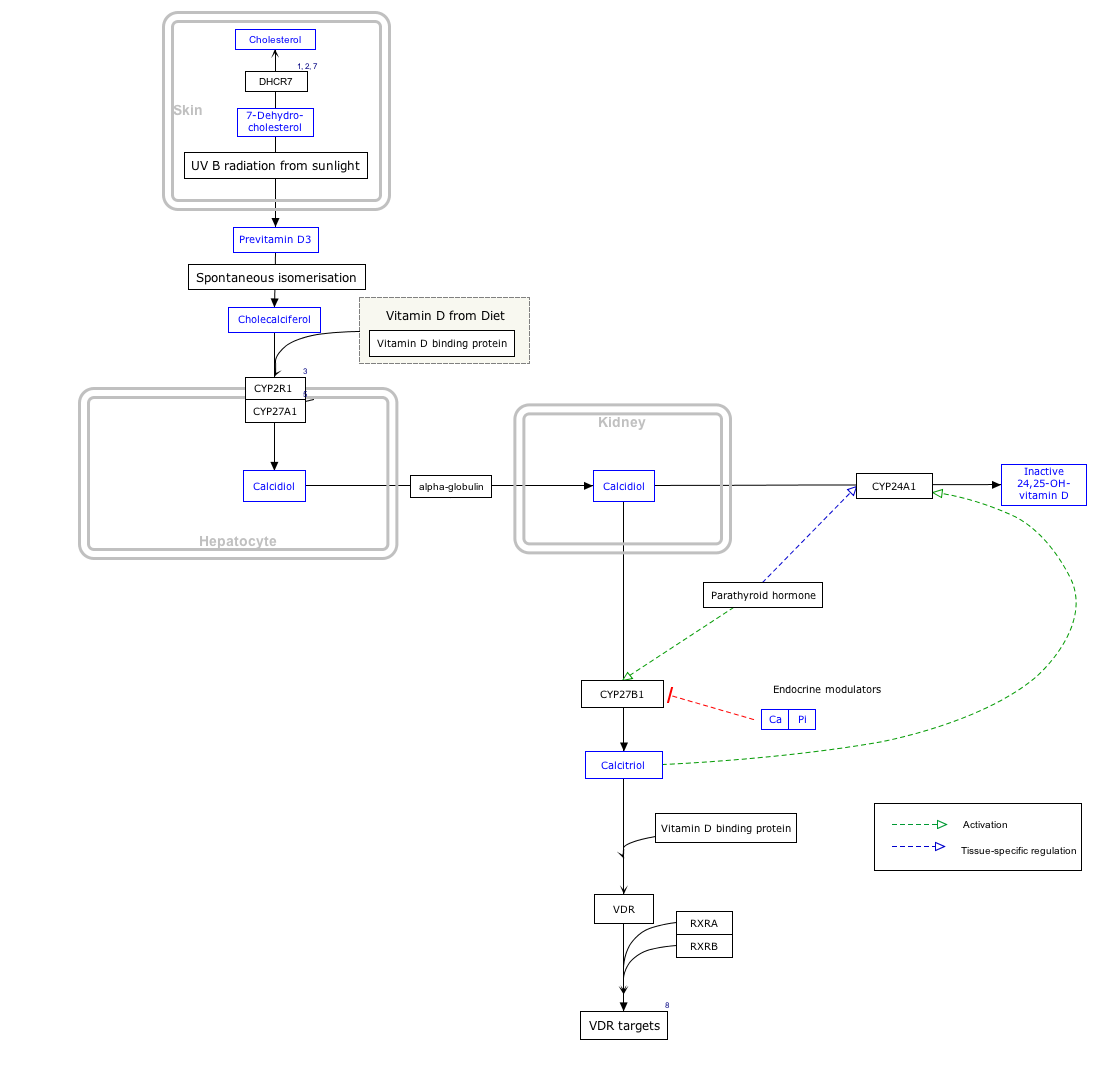
Interactive pathway map[edit]
Click on genes, proteins and metabolites below to link to respective articles.[§ 1]
- ^The interactive pathway map can be edited at WikiPathways:"VitaminDSynthesis_WP1531".
History[edit]
Research in the laboratory ofHector DeLucaidentified 25(OH)D in 1968 and showed that the liver was necessary for its formation.[21]The enzyme responsible for this synthesis,cholecalciferol 25-hydroxylase,was isolated in the same laboratory byMichael F. Holickin 1972.[22]
Research[edit]
Studies are ongoing comparing the effects of calcifediol with other forms of vitamin D including cholecalciferol in prevention and treatment ofosteoporosis.[3][20]
References[edit]
- ^abcd"IUPAC-IUB Joint Commission on Biochemical Nomenclature (JCBN): Nomenclature of vitamin D. Recommendations 1981".European Journal of Biochemistry.124(2): 223–7. May 1982.doi:10.1111/j.1432-1033.1982.tb06581.x.PMID7094913.
- ^"Drug and medical device highlights 2018: Helping you maintain and improve your health".Health Canada.14 October 2020.Retrieved17 April2024.
- ^abcdefghi"Vitamin D".Micronutrient Information Center, Linus Pauling Institute, Oregon State University, Corvallis. 11 February 2021.Retrieved14 March2022.
- ^abcdefghijklm"Office of Dietary Supplements - Vitamin D".ods.od.nih.gov.9 October 2020.Retrieved31 October2020.
- ^abcdefghiBikle DD (March 2014)."Vitamin D metabolism, mechanism of action, and clinical applications".Chemistry & Biology.21(3): 319–29.doi:10.1016/j.chembiol.2013.12.016.PMC3968073.PMID24529992.
- ^abcQuesada-Gomez JM, Bouillon R (August 2018). "Is calcifediol better than cholecalciferol for vitamin D supplementation?".Osteoporosis International(review).29(8): 1697–1711.doi:10.1007/s00198-018-4520-y.PMID29713796.S2CID14005489.
- ^ab"Rayaldee (calcifediol) FDA Approval History - Drugs".Retrieved4 March2021.
- ^abcdBouillon R, Bikle D (November 2019)."Vitamin D Metabolism Revised: Fall of Dogmas".Journal of Bone and Mineral Research(Review).34(11): 1985–1992.doi:10.1002/jbmr.3884.PMC9000993.PMID31589774.
- ^abHeaney RP, Armas LA, Shary JR, Bell NH, Binkley N, Hollis BW (June 2008)."25-Hydroxylation of vitamin D3: relation to circulating vitamin D3 under various input conditions".The American Journal of Clinical Nutrition.87(6): 1738–42.doi:10.1093/ajcn/87.6.1738.PMID18541563.
- ^Adams JS, Hewison M (July 2012)."Extrarenal expression of the 25-hydroxyvitamin D-1-hydroxylase".Arch Biochem Biophys.523(1): 95–102.doi:10.1016/j.abb.2012.02.016.PMC3361592.PMID22446158.
- ^abcd"25-hydroxy vitamin D test: Medline Plus".Retrieved 4 March 2021.
- ^"25HDN - Clinical: 25-Hydroxyvitamin D2 and D3, Serum".Mayo Clinic Labs. 2021.Retrieved4 March2021.
- ^abcHeaney RP (December 2004)."Functional indices of vitamin D status and ramifications of vitamin D deficiency".The American Journal of Clinical Nutrition.80(6 Suppl): 1706S–9S.doi:10.1093/ajcn/80.6.1706S.PMID15585791.
- ^Theodoratou E, Tzoulaki I, Zgaga L, Ioannidis JP (April 2014)."Vitamin D and multiple health outcomes: umbrella review of systematic reviews and meta-analyses of observational studies and randomised trials".BMJ.348:g2035.doi:10.1136/bmj.g2035.PMC3972415.PMID24690624.
- ^abcdAmerican Society for Clinical Pathology,"Five Things Physicians and Patients Should Question",Choosing Wisely:an initiative of theABIM Foundation,American Society for Clinical Pathology,retrievedAugust 1,2013,which cites
- Sattar N, Welsh P, Panarelli M, Forouhi NG (January 2012). "Increasing requests for vitamin D measurement: costly, confusing, and without credibility".Lancet.379(9811): 95–6.doi:10.1016/S0140-6736(11)61816-3.PMID22243814.S2CID12669468.
- Bilinski KL, Boyages SC (July 2012). "The rising cost of vitamin D testing in Australia: time to establish guidelines for testing".The Medical Journal of Australia.197(2): 90.doi:10.5694/mja12.10561.PMID22794049.S2CID45880893.
- Lu CM (May 2012)."Pathology consultation on vitamin D testing: clinical indications for 25(OH) vitamin D measurement".American Journal of Clinical Pathology.137(5).American Society for Clinical Pathology:831–2.doi:10.1309/ajcp2gp0ghkqrcoe.PMID22645788.,which cites
- Arya SC, Agarwal N (May 2012)."The measurement of vitamin D3requires maintaining quality control ".American Journal of Clinical Pathology.137(5): 832, author reply 833.doi:10.1309/AJCP2GP0GHKQRCOE.PMID22523224.
- Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. (July 2011)."Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline".The Journal of Clinical Endocrinology and Metabolism.96(7): 1911–30.doi:10.1210/jc.2011-0385.PMID21646368.
- ^Bender DA (2003)."Vitamin D".Nutritional biochemistry of the vitamins.Cambridge: Cambridge University Press.ISBN978-0-521-80388-5.Retrieved December 10, 2008 throughGoogle Book Search.
- ^Hollis BW (February 2005)."Circulating 25-hydroxyvitamin D levels indicative of vitamin D sufficiency: implications for establishing a new effective dietary intake recommendation for vitamin D".The Journal of Nutrition.135(2): 317–22.doi:10.1093/jn/135.2.317.PMID15671234.
- ^Kimball SM, Ursell MR, O'Connor P, Vieth R (September 2007)."Safety of vitamin D3 in adults with multiple sclerosis".The American Journal of Clinical Nutrition.86(3): 645–51.doi:10.1093/ajcn/86.3.645.PMID17823429.
- ^"Calcifediol".go.drugbank.Retrieved7 March2021.
- ^abcdCesareo R, Falchetti A, Attanasio R, Tabacco G, Naciu AM, Palermo A (May 2019)."Hypovitaminosis D: Is It Time to Consider the Use of Calcifediol?".Nutrients(Review).11(5): 1016.doi:10.3390/nu11051016.PMC6566727.PMID31064117.
- ^Ponchon G, Kennan AL, DeLuca HF (November 1969).""Activation" of vitamin D by the liver ".The Journal of Clinical Investigation.48(11): 2032–7.doi:10.1172/JCI106168.PMC297455.PMID4310770.
- ^Holick MF, DeLuca HF, Avioli LV (January 1972). "Isolation and identification of 25-hydroxycholecalciferol from human plasma".Archives of Internal Medicine.129(1): 56–61.doi:10.1001/archinte.1972.00320010060005.PMID4332591.