Onychomycosis
| Onychomycosis | |
|---|---|
| Other names | Dermatophytic onychomycosis[1]tinea unguium[1] |
 | |
| A toenail affected by onychomycosis | |
| Specialty | Infectious disease |
| Symptoms | White or yellow nail discoloration, thickening of the nail[2][3] |
| Complications | Lower legcellulitis[3] |
| Usual onset | Older males[2][3] |
| Causes | Fungal infection[3] |
| Risk factors | Athlete's foot,othernail diseases,exposure to someone with the condition,peripheral vascular disease,poor immune function[3] |
| Diagnostic method | Based on appearance, confirmed by laboratory testing[2] |
| Differential diagnosis | Psoriasis,chronicdermatitis,chronicparonychia,nail trauma[2] |
| Treatment | None,anti-fungal medication,trimming the nails[2][3] |
| Medication | Terbinafine,ciclopirox[2] |
| Prognosis | Often recurs[2] |
| Frequency | ~10% of adults[2] |
Onychomycosis,also known astinea unguium,[4]is afungal infectionof thenail.[2]Symptoms may include white or yellow nail discoloration, thickening of the nail, andseparation of the nail from the nail bed.[2]Fingernailsmay be affected, but it is more common for toenails.[3]Complications may includecellulitisof the lower leg.[3] A number of different types of fungus can cause onychomycosis, includingdermatophytesandFusarium.[3]Risk factors includeathlete's foot,othernail diseases,exposure to someone with the condition,peripheral vascular disease,andpoor immune function.[3]The diagnosis is generally suspected based on the appearance and confirmed by laboratory testing.[2]
Onychomycosis does not necessarily require treatment.[3]Theantifungal medicationterbinafinetaken by mouth appears to be the most effective but is associated withliver problems.[2][5]Trimming the affected nails when on treatment also appears useful.[2]
There is aciclopirox-containingnail polish,but there is no evidence that it works.[2]The condition returns in up to half of cases following treatment.[2]Not using old shoes after treatment may decrease the risk of recurrence.[3]
Onychomycosis occurs in about 10 percent of the adult population,[2]with older people more frequently affected.[2]Males are affected more often than females.[3]Onychomycosis represents about half of nail disease.[2]It was first determined to be the result of a fungal infection in 1853 byGeorg Meissner.[6]
Signs and symptoms
[edit]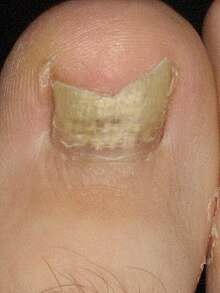

The most common symptom of a fungal nail infection is the nail becoming thickened and discoloured: white, black, yellow or green. As the infection progresses the nail can become brittle, with pieces breaking off or coming away from the toe or finger completely. If left untreated, the skin underneath and around the nail can become inflamed and painful. There may also be white or yellow patches on the nailbed or scaly skin next to the nail,[7]and a foul smell.[8]There is usually no pain or other bodily symptoms, unless the disease is severe.[9]People with onychomycosis may experience significantpsychosocialproblems due to the appearance of the nail, particularly when fingers – which are always visible – rather than toenails are affected.[10] Dermatophytidsare fungus-freeskin lesionsthat sometimes form as a result of a fungus infection in another part of the body. This could take the form of arashoritchin an area of the body that is not infected with the fungus. Dermatophytids can be thought of as anallergic reactionto the fungus.
Causes
[edit]The causativepathogensof onychomycosis are all in thefungus kingdomand includedermatophytes,Candida(yeasts), and nondermatophyticmolds.[2]Dermatophytes are the fungi most commonly responsible for onychomycosis in the temperate western countries; whileCandidaand nondermatophytic molds are more frequently involved in the tropics and subtropics with a hot and humid climate.[11]
Dermatophytes
[edit]When onychomycosis is due to a dermatophyte infection, it is termed tinea unguium.Trichophyton rubrumis the most commondermatophyteinvolved in onychomycosis. Other dermatophytes that may be involved areT. interdigitale,Epidermophyton floccosum,Tricholosporum violaceum,Microsporum gypseum,T. tonsurans,andT. soudanense.A common outdated name that may still be reported by medical laboratories isTrichophyton mentagrophytesforT. interdigitale.The nameT. mentagrophytesis now restricted to the agent offavusskin infection of themouse;though this fungus may be transmitted frommiceand theirdandersto humans, it generally infects skin and not nails.
Other
[edit]Other causativepathogensincludeCandidaand nondermatophyticmolds,in particular members of the mold genusScytalidium(name recently changed toNeoscytalidium),Scopulariopsis,andAspergillus. Candidaspecies mainly cause fingernail onychomycosis in people whose hands are often submerged in water.Scytalidiummainly affects people in thetropics,though it persists if they later move to areas oftemperate climate.
Other molds more commonly affect people older than 60 years, and their presence in the nail reflects a slight weakening in the nail's ability to defend itself against fungal invasion.
Nail injury andnail psoriasiscan cause damaged toenails to become thick, discolored & brittle.[12]
Risk factors
[edit]Advancing age (usually over the age of 60) is the most common risk factor for onychomycosis due to diminishedblood circulation,longer exposure to fungi, nails which grow more slowly and thicken, and reduced immune function increasing susceptibility to infection.[13]Nail fungus tends to affect men more often than women and is associated with a family history of this infection.
Other risk factors includeperspiringheavily, being in a humid or moist environment,psoriasis,wearing socks and shoes that hinder ventilation and do not absorb perspiration, going barefoot in damp public places such as swimming pools, gyms and shower rooms, havingathlete's foot(tinea pedis), minor skin or nail injury, damaged nail, or other infection, and having diabetes, circulation problems, which may also lead to lower peripheral temperatures on hands and feet, or a weakened immune system.[14]
Diagnosis
[edit]The diagnosis is generally suspected based on the appearance and confirmed by laboratory testing.[2]The four main tests are apotassium hydroxide smear,culture,histologyexamination, andpolymerase chain reaction.[2][3]The sample examined is generally nail scrapings or clippings.[2]These being from as far up the nail as possible.[3]
Nail platebiopsywithperiodic acid-Schiff stainappear more useful than culture or direct KOH examination.[15]To reliably identify nondermatophyte molds, several samples may be necessary.[16]
Classification
[edit]There are five classic types of onychomycosis:[17][18]
- Distal subungual onychomycosisis the most common form oftinea unguium[2]and is usually caused byTrichophyton rubrum,which invades thenail bedand the underside of thenail plate.
- White superficial onychomycosis(WSO) is caused by fungal invasion of the superficial layers of the nail plate to form "white islands" on the plate. It accounts for around 10 percent of onychomycosis cases. In some cases, WSO is a misdiagnosis of "keratins granulations" which are not a fungus, but a reaction to nail polish that can cause the nails to have a chalky white appearance. A laboratory test should be performed to confirm.[19]
- Proximal subungual onychomycosisis fungal penetration of the newly formed nail plate through the proximalnail fold.It is the least common form oftinea unguiumin healthy people, but is found more commonly when the patient is immunocompromised.[2]
- Endonyx onychomycosis is characterized byleukonychiaalong with a lack ofonycholysisor subungualhyperkeratosis.[18]
- Candidal onychomycosisisCandidaspecies invasion of the fingernails, usually occurring in persons who frequently immerse their hands in water. This normally requires the prior damage of the nail byinfectionortrauma.
Differential diagnosis
[edit]In many cases of suspected nail fungus there is actually no fungal infection, but only nail deformity.[20][21]
To avoid misdiagnosis asnail psoriasis,lichen planus,contact dermatitis,nail bedtumorssuch asmelanoma,trauma,oryellow nail syndrome,laboratory confirmation may be necessary.[2]
Other conditions that may appear similar to onychomycosis include:psoriasis,normal aging,green nail syndrome,yellow nail syndrome,and chronicparonychia.[22]
Treatment
[edit]
Medications
[edit]Most treatments are withantifungalmedications, either topically or by mouth.[2]Avoiding use of antifungal therapy by mouth (e.g.,terbinafine) in persons without a confirmed infection is recommended, because of the possible side effects of that treatment.[20]First topical terbinafine medication (MOB-015) was launched in February 2024 in Sweden under the name Terclara. This medication recorded 76% mycological cure rate in two phase 3 studies. The topical property of this medication ensures that typical terbinafine side effects are not present (1000 times lower terbinafine levels in plasma). Roll-out in other countries will continue in the coming years.[23][24]
Medications that may be taken by mouth include terbinafine (76% effective),itraconazole(60% effective), andfluconazole(48% effective).[2]They share characteristics that enhance their effectiveness: prompt penetration of the nail and nail bed,[25]and persistence in the nail for months after discontinuation of therapy.[26]Ketoconazoleby mouth is not recommended due to side effects.[27]Oral terbinafine is better tolerated than itraconazole.[28]For superficial white onychomycosis, systemic rather than topical antifungal therapy is advised.[29]
Topical agents includeciclopiroxnail paint,amorolfine,andefinaconazole.[30][31][32]Some topical treatments need to be applied daily for prolonged periods (at least one year).[31]Topical amorolfine is applied weekly.[33]
Efinaconazole,a topicalazole antifungal,led to cure rates two or three times better than the next-best topical treatment, ciclopirox.[34]In trials, about 17% of people were cured using efinaconazole, as opposed to 4% of people using placebo.[35]
Topical ciclopirox results in a cure in 6% to 9% of cases.[2][31]Ciclopirox when used with terbinafine appears to be better than either agent alone.[2]Although eficonazole, P-3051 (ciclopirox 8% hydrolacquer), andtavaboroleare effective at treating fungal infection of toenails, complete cure rates are low.[36]
Other
[edit]Chemical (keratolytic) or surgicaldebridementof the affected nail appears to improve outcomes.[2]
As of 2014, evidence forlaser treatmentis unclear as the evidence is of low quality[37]and varies by type of laser.[38]
Tea tree oilis not recommended as a treatment on present data. It was found to irritate the surrounding skin in some trial participants.[39]
Cost
[edit]United States
[edit]According to a 2015 study, the cost in the United States of testing with theperiodic acid–Schiff stain(PAS) was about $148. Even if the cheaperKOH testis used first and the PAS test is used only if the KOH test is negative, there is a good chance that the PAS will be done (because of either a true or a false negative with the KOH test). But the terbinafine treatment costs only $10 (plus an additional $43 for liver function tests). In conclusion the authors say that terbinafine has a relatively benign adverse effect profile, with liver damage very rare, so it makes more sense cost-wise for the dermatologist to prescribe the treatment without doing the PAS test. (Another option would be to prescribe the treatment only if the potassium hydroxide test is positive, but it gives a false negative in about 20% of cases of fungal infection.) On the other hand, as of 2015 the price of topical (non-oral) treatment withefinaconazolewas $2307 per nail, so testing is recommended before prescribing it.[21]
The cost of efinaconazole treatment can be reduced to $65 per 1-month dose usingdrug coupons,bringing the treatment cost to $715 per nail.[40]
Canada
[edit]In 2019, a study by theCanadian Agency for Drugs and Technologies in Healthfound the cost for a 48-week efinaconazole course to be $178 for a big toe, and $89 for a different toe.[41]
Prognosis
[edit]Recurrence may occur following treatment, with a 20-25% relapse rate within 2 years of successful treatment.[13]Nail fungus can be painful and cause permanent damage to nails. It may lead to other serious infections if the immune system is suppressed due to medication, diabetes or other conditions. The risk is most serious for people with diabetes and with immune systems weakened by leukemia or AIDS, or medication after organ transplant. Diabetics have vascular and nerve impairment, and are at risk ofcellulitis,a potentially serious bacterial infection; any relatively minor injury to feet, including a nail fungal infection, can lead to more serious complications.[42]Infection of the boneis another rare complication.[7]
Epidemiology
[edit]A 2003 survey of diseases of the foot in 16 European countries found onychomycosis to be the most frequent fungal foot infection and estimated its prevalence at 27%.[43][44]Prevalence was observed to increase with age. In Canada, the prevalence was estimated to be 6.48%.[45]Onychomycosis affects approximately one-third ofdiabetics[46]and is 56% more frequent in people withpsoriasis.[47]
Etymology
[edit]The term is fromAncient Greekὄνυξonyx"nail",μύκηςmykēs"fungus",[48]and the suffix-ωσιςōsis"functional disease".
Research
[edit]Research suggests that fungi are sensitive to heat, typically 40–60 °C (104–140 °F). The basis oflasertreatment is to try to heat the nail bed to these temperatures in order to disrupt fungal growth.[49]As of 2013 research into laser treatment seemed promising.[2]There is also ongoing development inphotodynamic therapy,which uses laser or LED light to activate photosensitisers that eradicate fungi.[50]
References
[edit]- ^abRapini RP, Bolognia JL, Jorizzo JL (2007).Dermatology: 2-Volume Set.St. Louis: Mosby. p. 1135.ISBN978-1-4160-2999-1.
- ^abcdefghijklmnopqrstuvwxyzaaabacadaeWesterberg DP, Voyack MJ (December 2013). "Onychomycosis: Current trends in diagnosis and treatment".American Family Physician.88(11): 762–70.PMID24364524.
- ^abcdefghijklmno"Onychomycosis – Dermatologic Disorders".Merck Manuals Professional Edition.February 2017.Retrieved2 June2018.
- ^Rodgers P, Bassler M (February 2001). "Treating onychomycosis".American Family Physician.63(4): 663–72, 677–8.PMID11237081.
- ^Kreijkamp-Kaspers S, Hawke K, Guo L, Kerin G, Bell-Syer SE, Magin P, et al. (July 2017)."Oral antifungal medication for toenail onychomycosis".The Cochrane Database of Systematic Reviews.2017(7): CD010031.doi:10.1002/14651858.CD010031.pub2.PMC6483327.PMID28707751.
- ^Rigopoulos D, Elewski B, Richert B (2018).Onychomycosis: Diagnosis and Effective Management.John Wiley & Sons.ISBN9781119226505.
- ^abNHS Choices: Symptoms of fungal nail infection
- ^Mayo clinic: Nail fungus
- ^OnychomycosisateMedicine
- ^Szepietowski JC, Reich A (July 2009). "Stigmatisation in onychomycosis patients: a population-based study".Mycoses.52(4): 343–9.doi:10.1111/j.1439-0507.2008.01618.x.PMID18793262.S2CID26932678.
- ^Chi CC, Wang SH, Chou MC (November 2005). "The causative pathogens of onychomycosis in southern Taiwan".Mycoses.48(6): 413–20.doi:10.1111/j.1439-0507.2005.01152.x.PMID16262878.S2CID43885361.
- ^"What is nail psoriasis, and how can I treat it?".aad.org.Retrieved2022-06-18.
- ^abFrazier, Winfred Taylor; Santiago-Delgado, Zuleica M.; Kenneth C. Stupka, I. I. (October 2021)."Onychomycosis: Rapid Evidence Review".American Family Physician.104(4): 359–367.ISSN1532-0650.PMID34652111.
- ^Mayo Clinic – Nail fungus – risk factors
- ^Velasquez-Agudelo V, Cardona-Arias JA (February 2017)."Meta-analysis of the utility of culture, biopsy, and direct KOH examination for the diagnosis of onychomycosis".BMC Infectious Diseases.17(1): 166.doi:10.1186/s12879-017-2258-3.PMC5320683.PMID28222676.
- ^Shemer A, Davidovici B, Grunwald MH, Trau H, Amichai B (January 2009). "New criteria for the laboratory diagnosis of nondermatophyte moulds in onychomycosis".The British Journal of Dermatology.160(1): 37–9.doi:10.1111/j.1365-2133.2008.08805.x.PMID18764841.S2CID42320540.
- ^James WD, Berger TG (2006).Andrews' Diseases of the Skin: clinical Dermatology.Saunders Elsevier.ISBN0-7216-2921-0.
- ^abTosti, Antonella (31 Jul 2018). Elston, Dirk M; Vinson, Richard P (eds.)."Onychomycosis".Medscape.Retrieved18 Jun2020.
- ^"AAPA".Cmecorner. Archived fromthe originalon 2011-07-08.Retrieved2010-08-05.
- ^abAmerican Academy of Dermatology(February 2013),"Five Things Physicians and Patients Should Question",Choosing Wisely:an initiative of theABIM Foundation,American Academy of Dermatology,retrieved5 December2013.Which cites:*Roberts DT, Taylor WD, Boyle J (March 2003)."Guidelines for treatment of onychomycosis"(PDF).The British Journal of Dermatology.148(3): 402–10.doi:10.1046/j.1365-2133.2003.05242.x.PMID12653730.S2CID33750748.Archived fromthe original(PDF)on 2017-08-10.Retrieved2014-08-01.
- ^abMikailov A, Cohen J, Joyce C, Mostaghimi A (March 2016)."Cost-effectiveness of Confirmatory Testing Before Treatment of Onychomycosis".JAMA Dermatology.152(3): 276–81.doi:10.1001/jamadermatol.2015.4190.PMID26716567.
- ^Hall B (2012).Sauer's Manual of Skin Diseases(10 ed.). Lippincott Williams & Wilkins. p. Chapter 33.ISBN9781451148688.
- ^"MOB-015".Retrieved13 June2024.
- ^"Efficacy and safety of topical terbinafine 10% solution (MOB-015) in the treatment of mild to moderate distal subungual onychomycosis: A randomized, multicenter, double-blind, vehicle-controlled phase 3 study".Retrieved12 June2024.
- ^Elewski BE (July 1998)."Onychomycosis: pathogenesis, diagnosis, and management".Clinical Microbiology Reviews.11(3): 415–29.doi:10.1128/CMR.11.3.415.PMC88888.PMID9665975.
- ^Elewski BE, Hay RJ (August 1996)."Update on the management of onychomycosis: highlights of the Third Annual International Summit on Cutaneous Antifungal Therapy".Clinical Infectious Diseases.23(2): 305–13.doi:10.1093/clinids/23.2.305.PMID8842269.
- ^"Nizoral (ketoconazole) Oral Tablets: Drug Safety Communication - Prescribing for Unapproved Uses including Skin and Nail Infections Continues; Linked to Patient Death".FDA.19 May 2016.Retrieved20 May2016.
- ^Haugh M, Helou S, Boissel JP, Cribier BJ (July 2002). "Terbinafine in fungal infections of the nails: a meta-analysis of randomized clinical trials".The British Journal of Dermatology.147(1): 118–21.doi:10.1046/j.1365-2133.2002.04825.x.PMID12100193.S2CID19682557.
- ^Baran R, Faergemann J, Hay RJ (November 2007). "Superficial white onychomycosis--a syndrome with different fungal causes and paths of infection".Journal of the American Academy of Dermatology.57(5): 879–82.doi:10.1016/j.jaad.2007.05.026.PMID17610995.
- ^Rodgers P, Bassler M (February 2001)."Treating onychomycosis".American Family Physician.63(4): 663–72, 677–8.PMID11237081.Archived fromthe originalon 2008-05-14.Retrieved2007-09-18.
- ^abcCrawford F, Hollis S (July 2007). Crawford F (ed.)."Topical treatments for fungal infections of the skin and nails of the foot".The Cochrane Database of Systematic Reviews.2007(3): CD001434.doi:10.1002/14651858.CD001434.pub2.PMC7073424.PMID17636672.
- ^Gupta AK, Paquet M (2014). "Efinaconazole 10% nail solution: a new topical treatment with broad antifungal activity for onychomycosis monotherapy".Journal of Cutaneous Medicine and Surgery.18(3): 151–5.doi:10.2310/7750.2013.13095.PMID24800702.S2CID10079807.
- ^Loceryl (5% amorolfine) package labelling
- ^"A Closer Look At A New Topical Option For Onychomycosis".Retrieved21 May2015.
- ^"Drugs at FDA: JUBLIA"(PDF).Retrieved26 June2014.
- ^Foley K, Gupta AK, Versteeg S, Mays R, Villanueva E, John D, et al. (Cochrane Skin Group) (January 2020)."Topical and device-based treatments for fungal infections of the toenails".The Cochrane Database of Systematic Reviews.1(1): CD012093.doi:10.1002/14651858.CD012093.pub2.PMC6984586.PMID31978269.
- ^Bristow IR (2014)."The effectiveness of lasers in the treatment of onychomycosis: a systematic review".Journal of Foot and Ankle Research.7:34.doi:10.1186/1757-1146-7-34.PMC4124774.PMID25104974.
- ^Liddell LT, Rosen T (April 2015)."Laser Therapy for Onychomycosis: Fact or Fiction?".Journal of Fungi.1(1): 44–54.doi:10.3390/jof1010044.PMC5770012.PMID29376898.
- ^Halteh P, Scher RK, Lipner SR (November 2016)."Over-the-counter and natural remedies for onychomycosis: do they really work?".Cutis.98(5): E16–E25.PMID28040821.
there was no statistical difference between the clotrimazole and TTO treatment groups in mycologic cure, clinical assessment, or patient subjective assessment of the nails. Although there was an 80% complete cure in the butenafine and TTO group, it was 0% in the TTO group at week 36. Trial design, longer treatment periods, incorporation into nanocapsules, or combination treatment with other antifungal agents may influence our future use of TTO for onychomycosis, but based on the present data we cannot recommend this treatment in clinical practice.
- ^"Ortho Dermatologics Access Program".orthorxaccess.Retrieved2021-08-10.
- ^"Table 5, CDR Cost Comparison Table for Onychomycosis".ncbi.nlm.nih.gov.8 June 2019.
- ^Mayo clinic – Nail fungus: complications
- ^Burzykowski T, Molenberghs G, Abeck D, Haneke E, Hay R, Katsambas A, et al. (December 2003). "High prevalence of foot diseases in Europe: results of the Achilles Project".Mycoses.46(11–12): 496–505.doi:10.1046/j.0933-7407.2003.00933.x.hdl:1942/429.PMID14641624.S2CID20055970.
- ^Verma S, Heffernan MP (2008). Superficial fungal infection: Dermatophytosis, onychomycosis, tinea nigra, piedra. In K Wolff et al., eds., Fitzpatrick's Dermatology in General Medicine, 7th ed., vol 2, pp. 1807–1821. New York: McGraw Hill.
- ^Vender, Ronald B.; Lynde, Charles W.; Poulin, Yves (2006). "Prevalence and epidemiology of onychomycosis".Journal of Cutaneous Medicine and Surgery.10 Suppl 2 (6_suppl): S28–S33.doi:10.2310/7750.2006.00056.PMID17204229.S2CID74819774.
- ^Gupta AK, Konnikov N, MacDonald P, Rich P, Rodger NW, Edmonds MW, et al. (October 1998). "Prevalence and epidemiology of toenail onychomycosis in diabetic subjects: a multicentre survey".The British Journal of Dermatology.139(4): 665–71.doi:10.1046/j.1365-2133.1998.02464.x.PMID9892911.S2CID22038748.
- ^Gupta AK, Lynde CW, Jain HC, Sibbald RG, Elewski BE, Daniel CR, et al. (May 1997). "A higher prevalence of onychomycosis in psoriatics compared with non-psoriatics: a multicentre study".The British Journal of Dermatology.136(5): 786–9.doi:10.1046/j.1365-2133.1997.6771624.x.PMID9205520.S2CID5969796.
- ^ὄνυξ,μύκης.Liddell, Henry George;Scott, Robert;A Greek–English Lexiconat thePerseus Project.
- ^"Device-based Therapies for Onychomycosis Treatment".Retrieved23 December2012.
- ^Piraccini BM, Alessandrini A (March 2015)."Onychomycosis: A Review".Journal of Fungi.1(1): 30–43.doi:10.3390/jof1010030.PMC5770011.PMID29376897.
