Pre-eclampsia
| Pre-eclampsia | |
|---|---|
| Other names | Preeclampsia toxaemia (PET) |
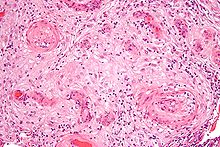 | |
| Amicrographshowinghypertrophic decidual vasculopathy,a finding seen ingestational hypertensionand pre-eclampsia.H&E stain. | |
| Specialty | Obstetrics |
| Symptoms | High blood pressure,protein in the urine[1] |
| Complications | Red blood cell breakdown,low blood platelet count,impaired liver function, kidney problems,swelling,shortness of breath due to fluid in the lungs,eclampsia[2][3] |
| Usual onset | After 20weeks of pregnancy[2] |
| Risk factors | Obesity,priorhypertension,older age,diabetes mellitus[2][4] |
| Diagnostic method | BP > 140 mmHgsystolicor 90 mmHgdiastolicat two separate times[3] |
| Prevention | Aspirin,calcium supplementation,treatment of prior hypertension[4][5] |
| Treatment | Delivery,medications[4] |
| Medication | Labetalol,methyldopa,magnesium sulfate[4][6] |
| Frequency | 2–8% of pregnancies[4] |
| Deaths | 46,900 hypertensive disorders in pregnancy (2015)[7] |
Pre-eclampsiais a multi-system disorder specific topregnancy,characterized by the new onset ofhigh blood pressureand often a significant amount ofprotein in the urineor by the new onset of high blood pressure along with significant end-organ damage, with or without theproteinuria.[8][1][9][10]When it arises, the condition begins after 20weeks of pregnancy.[2][3]In severe cases of the disease there may bered blood cell breakdown,alow blood platelet count,impaired liver function, kidney dysfunction,swelling,shortness of breath due to fluid in the lungs,or visual disturbances.[2][3]Pre-eclampsia increases the risk of undesirable as well as lethal outcomes for both the mother and the fetus including preterm labor.[11][12][3]If left untreated, it may result inseizuresat which point it is known aseclampsia.[2]
Risk factors for pre-eclampsia includeobesity,prior hypertension, older age, anddiabetes mellitus.[2][4]It is also more frequent in a woman's first pregnancy and if she is carrying twins.[2]The underlying mechanisms are complex and involve abnormalformation of blood vessels in the placentaamongst other factors.[2]Most cases are diagnosed before delivery, and may be categorized depending on the gestational week at delivery.[11]Commonly, pre-eclampsia continues into theperiod after delivery,then known as postpartum pre-eclampsia.[13][14]Rarely, pre-eclampsia may begin in the period after delivery.[3]While historically both high blood pressure and protein in the urine were required to make the diagnosis, some definitions also include those with hypertension and any associated organ dysfunction.[3][10]Blood pressure is defined as high when it is greater than 140 mmHgsystolicor 90 mmHgdiastolicat two separate times, more than four hours apart in a woman after twenty weeks of pregnancy.[3]Pre-eclampsia is routinely screened duringprenatal care.[15][16]
Recommendations for prevention include:aspirinin those at high risk,calcium supplementationin areas with low intake, and treatment of prior hypertension with medications.[4][5]In those with pre-eclampsia, delivery of the baby andplacentais an effective treatment[4]but full recovery can take days or weeks.[13]The point at which delivery becomes recommended depends on how severe the pre-eclampsia and how far along in pregnancy a woman is.[4]Blood pressure medication,such aslabetalolandmethyldopa,may be used to improve the mother's condition before delivery.[6]Magnesium sulfatemay be used to prevent eclampsia in those with severe disease.[4]Bed rest and salt intake have not been found to be useful for either treatment or prevention.[3][4]
Pre-eclampsia affects 2–8% of pregnancies worldwide.[4][17][12]Hypertensive disorders of pregnancy(which include pre-eclampsia) are one of the most common causes of death due to pregnancy.[6]They resulted in 46,900 deaths in 2015.[7]Pre-eclampsia usually occurs after 32 weeks; however, if it occurs earlier it is associated with worse outcomes.[6]Women who have had pre-eclampsia are at increased risk of high blood pressure,heart diseaseandstrokelater in life.[15][18]Further, those with pre-eclampsia may have a lower risk of breast cancer.[19]
Etymology
[edit]The word "eclampsia" is from the Greek term for lightning.[20]The first known description of the condition was byHippocratesin the 5th century BC.[20]
An outdated medical term for pre-eclampsia istoxemiaof pregnancy, a term that originated in the mistaken belief that the condition was caused bytoxins.[21]
Signs and symptoms
[edit]
Edema(especially in the hands and face) was originally considered an important sign for a diagnosis of pre-eclampsia. However, because edema is a common occurrence in pregnancy, its utility as a distinguishing factor in pre-eclampsia is not high.Pitting edema(unusual swelling, particularly of the hands, feet, or face, notable by leaving an indentation when pressed on) can be significant, and should be reported to a health care provider.
Further, a symptom such as epigastric pain may be misinterpreted as heartburn. Common features of pre-eclampsia which are screened for during pre-natal visits include elevated blood pressure and excess protein in the urine. Additionally, some women may develop severe headache as a sign of pre-eclampsia.[22]In general, none of the signs of pre-eclampsia are specific, and even convulsions in pregnancy are more likely to have causes other than eclampsia in modern practice.[23]Diagnosis depends on finding a coincidence of several pre-eclamptic features, the final proof being their regression within the days and weeks after delivery.[13]
Causes
[edit]The cause of preeclampsia is not fully understood. It is likely related factors such as:[2][15]
- Abnormalplacentation(formation and development of the placenta)
- Immunologic factors
- Prior or existing maternal pathology – pre-eclampsia is seen more at a higher incidence in individuals with pre-existinghypertension,obesity, orantiphospholipid antibody syndromeor those with a history of pre-eclampsia
- Dietary factors, e.g. calcium supplementation in areas where dietary calcium intake is low has been shown to reduce the risk of pre-eclampsia[4]
- Environmental factors, e.g. air pollution[24]
Those with long-termhigh blood pressurehave a 7 to 8 times higher risk than those without.[25]
Physiologically, research has linked pre-eclampsia to the following physiologic changes: alterations in the interaction between the maternal immune response and the placenta, placental injury,endothelialcell injury, altered vascular reactivity, oxidative stress, imbalance amongvasoactivesubstances, decreased intravascular volume, anddisseminated intravascular coagulation.[15][26]
While the exact cause of pre-eclampsia remains unclear, there is strong evidence that a major cause predisposing a susceptible woman to pre-eclampsia is an abnormally implanted placenta.[2][15]This abnormally implanted placenta may result in poor uterine and placental perfusion, yielding a state ofhypoxiaand increased oxidative stress and the release of anti-angiogenicproteins along with inflammatory mediators into the maternal plasma.[15]A major consequence of this sequence of events is generalizedendothelialdysfunction.[1]The abnormal implantation may stem from the maternalimmune system's response to the placenta, specifically a lack of establishedimmunological tolerance in pregnancy.Endothelial dysfunction results in hypertension and many of the other symptoms and complications associated with pre-eclampsia.[2]When pre-eclampsia develops in the last weeks of pregnancy or in a multiple pregnancy, the causation may in some cases, partly be due to a large placenta outgrowing the capacity of the uterus, eventually leading to the symptoms of pre-eclampsia.[27]
Abnormalchromosome 19microRNA cluster (C19MC) impairsextravillustrophoblastcell invasion to thespiral arteries,causing high resistance, low blood flow, and low nutrient supply to the fetus.[28][29][30]
Genetic factors
[edit]Despite a lack of knowledge on specific causal mechanisms of pre-eclampsia, there is strong evidence to suggest it results from both environmental and heritable factors. A 2005 study showed that women with a first-degree relative who had a pre-eclamptic birth are twice as likely to develop it themselves. Furthermore, men related to someone with affected birth have an increased risk of fathering a pre-eclamptic pregnancy.[31]Fetuses affected by pre-eclampsia have a higher chance of later pregnancy complications including growth restriction, prematurity, and stillbirth.[32]
The onset of pre-eclampsia is thought to be caused by several complex interactions between genetics and environmental factors. Our current understanding of the specifically heritable cause involves an imbalance of angiogenic factors in the placenta.[33]Angiogenesisinvolves the growth of new blood vessels from existing vessels, and an imbalance during pregnancy can affect the vascularization, growth, and biological function of the fetus. The irregular expression of these factors is thought to be controlled by multiple loci on different chromosomes.[34][32][35]Research on the topic has been limited because of theheterogeneousnature of the disease. Maternal, paternal, and fetal genotypes all play a role as well as complex epigenetic factors such as whether the parents smoke, maternal age, sexual cohabitation, and obesity.[33]Currently, there is very little understanding behind the mechanisms of these interactions. Due to the polygenic nature of pre-eclampsia, a majority of the studies that have been conducted thus far on the topic have utilizedgenome-wide association studies.[31]
One known effector of pre-eclampsia is the fetal lociFLT1.Located onchromosome 13in the q12 region, FLT1 codes for Fms-liketyrosine kinase1, an angiogenic factor expressed in fetaltrophoblasts.[34]Angiogenic factors are crucial for vascular growth in the placenta. An FLT1 soluble isoform caused by asplice variantis sFLT1, which works as an antiangiogenic factor, reducing vascular growth in the placenta. A healthy, normotensive pregnancy is characterized by a balance between these factors. However, upregulation of this variant and overexpression of sFL1 can contribute toendothelial dysfunction.Reduced vascular growth and endothelial dysfunction manifest primarily in maternal symptoms such as renal failure,edema,and seizures. However, these factors can also lead to inadequate oxygen, nutrient, or blood supply to the fetus.[36]Furthermore, in this loci region, severalsingle-nucleotide polymorphisms(SNPs) have been observed to impact the overexpression of sFL1. Specifically, SNPs rs12050029 and rs4769613's risk alleles are linked with low red blood cell counts and carry an increased risk of late-onset pre-eclampsia.
Patau syndrome,or Trisomy 13, is also associated with the upregulation of sFLT1 due to the extra copy of the 13th chromosome. Because of this upregulation of an antiangiogenic factor, women with trisomy 13 pregnancies often experience reduced placental vascularization and are at higher risk for developing pre-eclampsia.[37]
Beyond fetal loci, there have been some maternal loci identified as effectors of pre-eclampsia.Alpha-ketoglutarate-dependent hydroxylaseexpression onchromosome 16in the q12 region is also associated with pre-eclampsia. Specifically, allele rs1421085 heightens the risk of not just pre-eclampsia but also an increase inBMIand hypertension.[35]Thispleiotropyis one of the reasons why these traits are considered to be a risk factor. Furthermore,ZNF831(zinc finger protein 831) and its loci on chromosome 20q13 were identified as another significant factor in pre-eclampsia. The risk allele rs259983 is also associated with both pre-eclampsia and hypertension, further evidence that the two traits are possibly linked.
While the current understanding suggests that maternal alleles are the main hereditary cause of pre-eclampsia, paternal loci have also been implicated. In one study, paternalDLX5(Distal-Less Homeobox 5) was identified as animprinted gene.Located onchromosome 7in the q21 region, DLX5 serves as a transcription factor often linked with the developmental growth of organs.[38]When paternally inherited, DLX5 and its SNP rs73708843 are shown to play a role in trophoblast proliferation, affecting vascular growth and nutrient delivery.[39]
Besides specific loci, several important genetic regulatory factors contribute to the development of pre-eclampsia. Micro RNAs, ormiRNAs,are noncoding mRNAs that down-regulate posttranscriptional gene expression through RNA-induced silencing complexes. In the placenta, miRNAs are crucial for regulating cell growth, angiogenesis, cell proliferation, and metabolism.[40]These placental-specific miRNAs are clustered in large groups, mainly onchromosomes 14and19,and irregular expression of either is associated with an increased risk of an affected pregnancy. For instance, miR-16 and miR-29 arevascular endothelial growth factors(VEGFs) and play a role in upregulating sFLT-1. In particular, the overexpression of miRNA miR-210 has been shown to inducehypoxia,which affects spiral artery remodeling, an important part of the pathogenesis of pre-eclampsia.[28]
Risk factors
[edit]Known risk factors for pre-eclampsia include:[6][41]
- Having never previously given birth
- Diabetes mellitus[42]
- Endometriosis[43]
- Obesity[42]
- Advanced maternal age (>35 years)
- Kidney disease
- Untreated hypertension[42]
- Prior history of pre-eclampsia[42]
- Family history of pre-eclampsia
- Antiphospholipid antibody syndrome[42]
- Multiple gestation[42]
- Havingdonated a kidney[44]
- Having sub-clinicalhypothyroidismorthyroidantibodies[45][46]
- Placental abnormalities such as placentalischemia
- Socioeconomicsplay a large role in the prevalence of theserisk factors,and, like other processes, each risk factor plays a role in the likelihood of increased consequences (morbidity) to, and the complexity of care for, the hospitalized patient
Pathogenesis
[edit]Although much research into mechanism of pre-eclampsia has taken place, its exact pathogenesis remains uncertain. Pre-eclampsia is thought to result from an abnormal placenta, the removal of which ends the disease in most cases.[2]During normal pregnancy, the placenta vascularizes to allow for the exchange of water, gases, and solutes, including nutrients and wastes, between maternal and fetal circulations.[26]Abnormal development of the placenta leads to poor placental perfusion. The placenta of women with pre-eclampsia is abnormal and characterized by poor trophoblastic invasion.[26]It is thought that this results in oxidative stress, hypoxia, and the release of factors that promote endothelial dysfunction, inflammation, and other possible reactions.[1][26][47]
In normal early embryonic development, the outer epithelial layer contains cytotrophoblast cells, a stem cell type found in the trophoblast that later differentiates into the fetal placenta. These cells differentiate into many placental cells types, including extravillous trophoblast cells. Extravillous trophoblast cells are an invasive cell type which remodel the maternal spiral arteries by replacing the maternal epithelium and smooth muscle lining the spiral arteries, thus causing and maintaining spiral artery dilation. This prevents maternal vasoconstriction in the spiral arteries and allows for continued blood and nutrient supply to the growing fetus with low resistance and high blood flow.[28]
The clinical manifestations of pre-eclampsia are associated with general endothelial dysfunction, including vasoconstriction and end-organischemia.[26]Implicit in this generalized endothelial dysfunction may be an imbalance ofangiogenicandanti-angiogenicfactors.[2]Both circulating and placental levels ofsoluble fms-like tyrosine kinase-1(sFlt-1) are higher in women with pre-eclampsia than in women with normal pregnancy.[26]sFlt-1 is an anti-angiogenic protein that antagonizesvascular endothelial growth factor(VEGF) andplacental growth factor(PIGF), both of which are proangiogenic factors.[15]Solubleendoglin(sEng) has also been shown to be elevated in women with pre-eclampsia and has anti-angiogenic properties, much like sFlt-1 does.[26]
Both sFlt-1 and sEng are upregulated in all pregnant women to some extent, supporting the idea that hypertensive disease in pregnancy is a normal pregnancy adaptation gone awry. As natural killer cells are intimately involved in placentation and placentation involves a degree ofmaternal immune tolerancefor a foreign placenta, it is not surprising that the maternal immune system might respond more negatively to the arrival of some placentae under certain circumstances, such as a placenta which is more invasive than normal. Initial maternal rejection of the placentalcytotrophoblastsmay be the cause of the inadequately remodeledspiral arteriesin those cases of pre-eclampsia associated with shallow implantation, leading to downstream hypoxia and the appearance of maternal symptoms in response to upregulated sFlt-1 and sEng.
Oxidative stress may also play an important part in the pathogenesis of pre-eclampsia. The main source of reactive oxygen species (ROS) is the enzymexanthine oxidase(XO) and this enzyme mainly occurs in the liver. One hypothesis is that the increased purine catabolism from placental hypoxia results in increased ROS production in the maternal liver and release into the maternal circulation that causes endothelial cell damage.[48]
Abnormalities in the maternalimmune systemand insufficiency ofgestational immune toleranceseem to play major roles in pre-eclampsia. One of the main differences found in pre-eclampsia is a shift towardTh1responsesand the production ofIFN-γ.The origin of IFN-γ is not clearly identified and could be thenatural killer cellsof the uterus, the placental dendritic cells modulating responses ofT helper cells,alterations in synthesis of or response to regulatory molecules, or changes in the function ofregulatory T cellsin pregnancy.[49]Aberrant immune responses promoting pre-eclampsia may also be due to an altered fetal allorecognition or to inflammatory triggers.[49]It has been documented that fetal cells such as fetalerythroblastsas well ascell-free fetal DNAare increased in the maternal circulation in women who develop pre-eclampsia. These findings have given rise to the hypothesis that pre-eclampsia is a disease process by which a placental lesion such as hypoxia allows increased fetal material into the maternal circulation, that in turn leads to animmune responseand endothelial damage, and that ultimately results in pre-eclampsia and eclampsia.
One hypothesis for vulnerability to pre-eclampsia is the maternal-fetal conflict between the maternal organism and fetus.[50]After the first trimester trophoblasts enter the spiral arteries of the mother to alter the spiral arteries and thereby gain more access to maternal nutrients.[50]Occasionally there is impaired trophoblast invasion that results in inadequate alterations to the uterine spiral arteries.[50]It is hypothesized that the developing embryo releases biochemical signals that result in the woman developing hypertension and pre-eclampsia so that the fetus can benefit from a greater amount of maternal circulation of nutrients due to increased blood flow to the impaired placenta.[50]This results in a conflict between maternal and fetal fitness and survival because the fetus is invested in only its survival and fitness while the mother is invested in this and subsequent pregnancies.[50]
Another evolutionary hypothesis for vulnerability to pre-eclampsia is the idea of ensuring pair-bonding between the mother and father and paternal investment in the fetus.[51]Researchers posit that pre-eclampsia is an adaptation for the mother to terminate investment in a fetus that might have an unavailable father, as determined by repeated semen exposure of the father to the mother.[51]Various studies have shown that women who frequently had exposure to partners' semen before conception had a reduced risk of pre-eclampsia.[51]Also, subsequent pregnancies by the same father had a reduced risk of pre-eclampsia while subsequent pregnancies by a different father had a higher risk of developing pre-eclampsia.[51]
In pre-eclampsia, abnormal expression of chromosome 19 microRNA cluster (C19MC) in placental cell lines reduces extravillus trophoblast migration.[29][30]Specific microRNAs in this cluster which might cause abnormal spiral artery invasion include miR-520h, miR-520b, and 520c-3p. This impairs extravillus trophoblast cells invasion to the maternal spiral arteries, causing high resistance and low blood flow and low nutrient supply to the fetus.[28]There is tentative evidence that vitamin supplementation can decrease the risk.[52]
Immune factors may also play a role.[53][49]
Diagnosis
[edit]| Pre-eclampsia laboratory values | |
|---|---|
 Shorthand for laboratory values commonly used in pre-eclampsia. LDH=Lactate dehydrogenase,Uric acid=Uric acid,AST=Aspartate aminotransferase,ALT=Alanine aminotransferase,Plt=Platelets,Cr=Creatinine. | |
| Reference range | LDH: 105–333 IU/L Uric Acid: 2.4–6.0 mg/dL AST: 5–40 U/L ALT: 7–56 U/L Plt: 140–450 x 109/L Cr: 0.6–1.2 mg/dL |
| MeSH | D007770 |
| LOINC | Codes for pre-eclampsia |
Testing for pre-eclampsia is recommended throughoutpregnancyvia measuring a woman's blood pressure.[16]
Diagnostic criteria
[edit]Pre-eclampsia is diagnosed when a pregnant woman develops:[54]
- Blood pressure ≥140 mmHg systolic or ≥90 mmHg diastolic on two separate readings taken at least four to six hours apart after 20 weeks' gestation in an individual with previously normal blood pressure.
- In a woman with essential hypertension beginning before 20 weeks' gestational age, the diagnostic criteria are an increase in systolic blood pressure (SBP) of ≥30 mmHg or an increase in diastolic blood pressure (DBP) of ≥15 mmHg.
- Proteinuria≥ 0.3 grams (300 mg) or more of protein in a 24-hour urine sample or a SPOT urinary protein to creatinine ratio ≥0.3 or a urine dipstick reading of 1+ or greater (dipstick reading should only be used if other quantitative methods are not available).[3]
Suspicion for pre-eclampsia should be maintained in any pregnancy complicated by elevated blood pressure, even in the absence of proteinuria. Ten percent of individuals with other signs and symptoms of pre-eclampsia and 20% of individuals diagnosed with eclampsia show no evidence of proteinuria.[26]In the absence of proteinuria, the presence of new-onsethypertension(elevated blood pressure) and the new onset of one or more of the following is suggestive of the diagnosis of pre-eclampsia:[3][6]
- Evidence of kidney dysfunction (oliguria,elevatedcreatininelevels)
- Impaired liver function (noted byliver function tests)
- Thrombocytopenia(platelet count <100,000/microliter)
- Pulmonary edema
- Ankle edema(pitting type)
- Cerebral or visual disturbances
Pre-eclampsia is a progressive disorder and these signs of organ dysfunction are indicative of severe pre-eclampsia. A systolic blood pressure ≥160 or diastolic blood pressure ≥110 and/or proteinuria >5g in a 24-hour period is also indicative of severe pre-eclampsia.[6]Clinically, individuals with severe pre-eclampsia may also presentepigastric/right upper quadrant abdominal pain, headaches, and vomiting.[6]Severe pre-eclampsia is a significant risk factor for intrauterine fetal death.
A rise in baseline blood pressure (BP) of 30mmHgsystolic or 15 mmHg diastolic, while not meeting the absolute criteria of 140/90, is important to note but is not considered diagnostic.
Predictive tests
[edit]There have been many assessments of tests aimed at predicting pre-eclampsia, though no single biomarker is likely to be sufficiently predictive of the disorder.[15]Predictive tests that have been assessed include those related to placental perfusion, vascular resistance, kidney dysfunction,endothelialdysfunction, and oxidative stress. Examples of notable tests include:
- Dopplerultrasonographyof the uterine arteries to investigate for signs of inadequate placental perfusion. This test has a high negative predictive value among those individuals with a history of prior pre-eclampsia.[26]
- Elevations in serum uric acid (hyperuricemia) is used by some to "define" pre-eclampsia,[41]though it has been found to be a poor predictor of the disorder.[26]Elevated levels in the blood (hyperuricemia) are likely due to reduced uric acid clearance secondary to impaired kidney function.
- Angiogenicproteins such asvascular endothelial growth factor(VEGF) andplacental growth factor(PIGF) and anti-angiogenic proteins such assoluble fms-like tyrosine kinase-1(sFlt-1) have shown promise for potential clinical use in diagnosing pre-eclampsia, though evidence is insufficient to recommend a clinical use for these markers.[41]
A recent study, ASPRE, known to be the largest multi-country prospective trial, has reported a significant performance in identifying pregnant women at high risk of pre-eclampsia yet during the first trimester of pregnancy. Utilizing a combination of maternal history, mean arterial blood pressure, intrauterine Doppler and PlGF measurement, the study has shown a capacity to identify more than 75% of the women that will develop pre-eclampsia, allowing early intervention to prevent development of later symptoms.[55]This approach is now officially recommended by the International Federation of Gynecologists & Obstetricians (FIGO),[56]However this model particularly predict pre-eclampsia with onset before 34 weeks' of gestation, while prediction of pre-eclampsia with later onset remains challenging.[57][58]
- Recent studies have shown that looking forpodocytes(specialized cells of the kidney) in the urine has the potential to aid in the prediction of pre-eclampsia. Studies have demonstrated that finding podocytes in the urine may serve as an early marker of and diagnostic test for pre-eclampsia.[59][60][61]
Differential diagnosis
[edit]Pre-eclampsia can mimic and be confused with many other diseases, including chronic hypertension, chronic renal disease, primary seizure disorders, gallbladder andpancreatic disease,immune orthrombotic thrombocytopenic purpura,antiphospholipid syndromeandhemolytic-uremic syndrome.It must be considered a possibility in any pregnant woman beyond 20 weeks of gestation. It is particularly difficult to diagnose when pre-existing conditions such ashypertensionare present.[62]Women withacute fatty liver of pregnancymay also present with elevated blood pressure and protein in the urine, but differ by the extent of liver damage. Other disorders that can cause high blood pressure includethyrotoxicosis,pheochromocytoma,anddrug misuse.[6]
Prevention
[edit]Preventive measures against pre-eclampsia have been heavily studied. Because the pathogenesis of pre-eclampsia is not completely understood, prevention remains a complex issue. Some currently accepted recommendations are:
Diet
[edit]Supplementation with a balanced protein and energy diet does not appear to reduce the risk of pre-eclampsia.[63]Further, there is no evidence that changingsaltintake has an effect.[64]
Supplementation withantioxidantssuch asvitamin C,DandEhas no effect on pre-eclampsia incidence;[65][66]therefore, supplementation with vitamins C, E, and D is not recommended for reducing the risk of pre-eclampsia.[66]
Calciumsupplementation of at least 1 gram per day is recommended during pregnancy as it prevents pre-eclampsia where dietary calcium intake is low, especially for those at high risk.[66][67]Higherseleniumlevel is associated with lower incidence of pre-eclampsia.[68][69]Highercadmiumlevel is associated with higher incidence of pre-eclampsia.[69]
Aspirin
[edit]Takingaspirinis associated with a 1 to 5% reduction in pre-eclampsia and a 1 to 5% reduction in premature births in women at high risk.[70]TheWorld Health Organizationrecommends low-dose aspirin for the prevention of pre-eclampsia in women at high risk and recommends it be started before 20 weeks of pregnancy.[66]TheUnited States Preventive Services Task Forcerecommends a low-dose regimen for women at high risk beginning in the 12th week.[71]Benefits are less if started after 16 weeks.[72]Since 2018 theAmerican College of Obstetricians and Gynecologistshas recommended low-dose aspirin therapy as standard preventive treatment for pre-eclampsia.[73]There is a reported problem of its efficacy when combined withparacetamol.[73]Supplementation of aspirin withL-Argininehas shown favourable results.[73]
The study ASPRE, besides its efficacy in identifying women suspected to develop pre-eclampsia, has also been able to demonstrate a strong drop in the rate of early pre-eclampsia (-82%) and preterm pre-eclampsia (-62%). The efficacy of aspirin is due to screening to identify high risk women, adjusted prophylaxis dosage (150 mg/day), timing of the intake (bedtime) and must start before week 16 of pregnancy.[55]
Physical activity
[edit]There is insufficient evidence to recommend either exercise[74]or strict bedrest[75]as preventive measures of pre-eclampsia.
Smoking cessation
[edit]In low-risk pregnancies, the association between cigarettesmokingand a reduced risk of pre-eclampsia has been consistent and reproducible across epidemiologic studies. High-risk pregnancies (those with pregestational diabetes, chronic hypertension, history of pre-eclampsia in a previous pregnancy, or multifetal gestation) showed no significant protective effect. The reason for this discrepancy is not definitively known; research supports speculation that the underlying pathology increases the risk of pre-eclampsia to such a degree that any measurable reduction of risk due to smoking is masked.[76]However, the damaging effects of smoking on overall health and pregnancy outcomes outweighs the benefits in decreasing the incidence of pre-eclampsia.[15]It is recommended that smoking be stopped prior to, during and after pregnancy.[77]
Immune modulation
[edit]Some studies have suggested the importance of a woman'sgestational immunological toleranceto her baby's father, as the baby and father share genetics. There is tentative evidence that ongoing exposure either by vaginal or oral sex to the same semen that resulted in the pregnancy decreases the risk of pre-eclampsia.[78]As one early study described, "although pre-eclampsia is a disease of first pregnancies, the protective effect of multiparity is lost with change of partner".[79]The study also concluded that although women with changing partners are strongly advised to use condoms to prevent sexually transmitted diseases, "a certain period of sperm exposure within a stable relation, when pregnancy is aimed for, is associated with protection against pre-eclampsia".[79]
Several other studies have since investigated the decreased incidence of pre-eclampsia in women who had received blood transfusions from their partner, those with long preceding histories of sex without barrier contraceptives, and in women who had been regularly performingoral sex.[80]
Having already noted the importance of a woman's immunological tolerance to her baby's paternal genes, several Dutch reproductive biologists decided to take their research a step further. Consistent with the fact that human immune systems tolerate things better when they enter the body via the mouth, the Dutch researchers conducted a series of studies that confirmed a surprisingly strong correlation between a diminished incidence of pre-eclampsia and a woman's practice of oral sex, and noted that the protective effects were strongest if she swallowed her partner's semen.[80][81]A team from theUniversity of Adelaidehas also investigated to see if men who have fathered pregnancies which have ended inmiscarriageor pre-eclampsia had low seminal levels of critical immune modulating factors such asTGF-beta.The team has found that certain men, dubbed "dangerous males", are several times more likely to father pregnancies that would end in either pre-eclampsia or miscarriage.[78]Among other things, most of the "dangerous males" seemed to lack sufficient levels of the seminal immune factors necessary to induceimmunological tolerancein their partners.[82]
As the theory of immune intolerance as a cause of pre-eclampsia has become accepted, women with repeated pre-eclampsia, miscarriages, orin vitro fertilizationfailures could potentially be administered key immune factors such as TGF-beta along with the father's foreign proteins, possibly either orally, as a sublingual spray, or as a vaginal gel to be applied onto the vaginal wall before intercourse.[78]
Treatment
[edit]The definitive treatment for pre-eclampsia is the delivery of the baby and placenta, but danger to the mother persists after delivery, and full recovery can take days or weeks.[13]The timing of delivery should balance the desire for optimal outcomes for the baby while reducing risks for the mother.[15]The severity of disease and the maturity of the baby are primary considerations.[83]These considerations are situation specific, and management will vary with situation, location, and institution. Treatment can range from expectant management to expedited delivery byinduction of labororcaesarean section.In the case ofpreterm deliveryadditional treatments including corticosteroid injection to accelerate fetal pulmonary maturation and magnesium sulfate for prevention of cerebral palsy should be considered. Important in management is the assessment of the mother's organ systems, management of severe hypertension, and prevention and treatment of eclamptic seizures.[15]Separate interventions directed at the baby may also be necessary. Bed rest has not been found to be useful and is thus not routinely recommended.[84]
Blood pressure
[edit]The World Health Organization recommends that women with severehypertensionduring pregnancy should receive treatment with anti-hypertensive agents.[4]Severe hypertension is generally considered systolic BP of at least 160 or diastolic BP of at least 110.[3]Evidence does not support the use of one anti-hypertensive over another.[15]The choice of which agent to use should be based on the prescribing clinician's experience with a particular agent, its cost, and its availability.[4]Diuretics are not recommended for prevention of pre-eclampsia and its complications.[4]Labetalol,hydralazineandnifedipineare commonly used antihypertensive agents forhypertension in pregnancy.[6]ACE inhibitorsandangiotensin receptor blockersare contraindicated as they affect fetal development.[54]
The goal of treatment of severe hypertension in pregnancy is to prevent cardiovascular, kidney, and cerebrovascular complications.[3]The target blood pressure has been proposed to be 140–160 mmHg systolic and 90–105 mmHg diastolic, although values are variable.[85]
Prevention of eclampsia
[edit]The intrapartum and postpartum administration of magnesium sulfate is recommended in severe pre-eclampsia for the prevention ofeclampsia.[4][15]Further, magnesium sulfate is recommended for the treatment of eclampsia over other anticonvulsants.[4]Magnesium sulfate acts by interacting withNMDA receptors.[54]
Epidemiology
[edit]Pre-eclampsia affects approximately 2–8% of all pregnancies worldwide.[1][2][86]The incidence of pre-eclampsia has risen in the U.S. since the 1990s, possibly as a result of increased prevalence of predisposing disorders, such as chronic hypertension, diabetes, and obesity.[15]
Pre-eclampsia is one of the leading causes of maternal and perinatal morbidity and mortality worldwide.[1]Nearly one-tenth of all maternal deaths in Africa and Asia and one-quarter in Latin America are associated with hypertensive diseases in pregnancy, a category that encompasses pre-eclampsia.[4]
Pre-eclampsia is much more common in women who are pregnant for the first time.[87]Women who have previously been diagnosed with pre-eclampsia are also more likely to experience pre-eclampsia in subsequent pregnancies.[6]Pre-eclampsia is also more common in women who have pre-existinghypertension,obesity,diabetes,autoimmunediseases such aslupus,various inherited thrombophilias such asFactor V Leiden,renal disease,multiple gestation (twinsormultiple birth), and advanced maternal age.[6]Women who live at high altitude are also more likely to experience pre-eclampsia.[88][89]Pre-eclampsia is also more common in some ethnic groups (e.g. African-Americans, Sub-Saharan Africans, Latin Americans, African Caribbeans, and Filipinos).[15][90][91]Change of paternity in a subsequent pregnancy has been implicated as affecting risk, except in those with a family history of hypertensive pregnancy.[92]
Eclampsiais a major complication of pre-eclampsia. Eclampsia affects 0.56 per 1,000 pregnant women in developed countries and almost 10 to 30 times as many women in low-income countries as in developed countries.[6]
Complications
[edit]Complications of pre-eclampsia can affect both the mother and the fetus. Acutely, pre-eclampsia can be complicated byeclampsia,the development ofHELLP syndrome,hemorrhagic or ischemicstroke,liver damage and dysfunction,acute kidney injury,andacute respiratory distress syndrome(ARDS).[6][26]
Pre-eclampsia is also associated with increased frequency ofcaesarean section,preterm delivery,andplacental abruption.Furthermore, an elevation in blood pressure can occur in some individuals in the first week postpartum attributable to volume expansion and fluid mobilization.[26]Fetal complications include fetal growth restriction and potential fetal or perinatal death.[26]
Long-term, an individual with pre-eclampsia is at increased risk for recurrence of pre-eclampsia in subsequent pregnancies.
Eclampsia
[edit]Eclampsiais the development of newconvulsionsin a pre-eclamptic patient that may not be attributed to other causes. It is a sign that the underlying pre-eclamptic condition is severe and is associated with high rates of perinatal and maternal morbidity and mortality.[4]Warning symptoms for eclampsia in an individual with current pre-eclampsia may include headaches, visual disturbances, and right upper quadrant or epigastric abdominal pain, with a headache being the most consistent symptom.[15][41]During pregnancy brisk or hyperactive reflexes are common, however, ankleclonusis a sign of neuromuscular irritability that usually reflects severe pre-eclampsia and also can precede eclampsia.[93]Magnesium sulfateis used to prevent convulsions in cases of severe pre-eclampsia.
HELLP Syndrome
[edit]HELLP syndromeis defined ashemolysis(microangiopathic), elevated liver enzymes (liver dysfunction), and low platelets (thrombocytopenia). This condition may occur in 10–20% of patients with severe pre-eclampsia and eclampsia[15]and is associated with increased maternal and fetal morbidity and mortality. In 50% of instances, HELLP syndrome develops preterm, while 20% of cases develop in late gestation and 30% during the post-partum period.[6]
Long term
[edit]Preeclampsia predisposes for future cardiovascular disease and a history of preeclampsia/eclampsia doubles the risk for cardiovascular mortality later in life.[26][94]Other risks includestroke,chronic hypertension,kidney disease andvenous thromboembolism.[95][94]Preeclampsia and cardiovascular disease share many risk factors such as age, elevated BMI, family history and certain chronic diseases.[96]
It seems that pre-eclampsia does not increase the risk ofcancer.[95]
Lowered blood supply to the fetus in pre-eclampsia causes lowered nutrient supply, which could result inintrauterine growth restriction(IUGR) and low birth weight.[28]The fetal origins hypothesis states that fetal undernutrition is linked with coronary heart disease later in adult life due to disproportionate growth.[97]
Because pre-eclampsia leads to a mismatch between the maternal energy supply and fetal energy demands, pre-eclampsia can lead to IUGR in the developing fetus.[98]Infants with IUGR are prone to have poor neuronal development and in increased risk for adult disease according to the Barker hypothesis. Associated adult diseases of the fetus due to IUGR include, but are not limited to,coronary artery disease(CAD),type 2 diabetes mellitus(T2DM),cancer,osteoporosis,and various psychiatric illnesses.[99]
The risk of pre-eclampsia and development of placental dysfunction has also been shown to be recurrent cross-generationally on the maternal side and most likely on the paternal side. Fetuses born to mothers who were born small forgestational age(SGA) were 50% more likely to develop pre-eclampsia while fetuses born to both SGA parents were three-fold more likely to develop pre-eclampsia in future pregnancies.[100]
Postpartum preeclampsia
[edit]Preeclampsia can also occur in the postpartum period or after delivery. There are currently no clear definitions or guidelines for postpartum preeclampsia, but experts have proposed a definition of new-onset preeclampsia that occurs between 48 hours after delivery up to 6 weeks after delivery.[101]
Thediagnostic criteriaotherwise are essentially the same as for preeclampsia diagnosed during pregnancy. Similarly, many of therisk factorsare the same, except that not having been pregnant previously does not seem to be a risk factor for postpartum preeclampsia.[102]There are other risk factors related to the labor and/or delivery that are associated with postpartum preeclampsia like cesarean delivery and higher rates of intravenous fluids.[101]
The American College of Obstetricians and Gynecologists recommends blood pressure evaluation for patients who have any hypertensive disorder of pregnancy within 7-10 days after delivery. Home blood pressure monitoring may increase the likelihood of measuring blood pressure during these recommended time periods.[103]
In general, thetreatmentof postpartum preeclampsia is the same as during pregnancy, including using anti-hypertensive medications to lower blood pressure and magnesium sulfate to prevent eclampsia. The same blood pressure medications that are used during pregnancy can be used in the postpartum period. There may be other medications that can be used, when there is no longer concern for the developing fetus. In general,ACE inhibitors,beta-blockers,andcalcium channel blockersall appear to be safe in lactating patients.[104]There is no data showing that any one medication is most effective for postpartum blood pressure management.[103]In addition, there is evidence that the use of a diuretic,furosemide,may shorten the duration of hypertension in patients with postpartum preeclampsia.[103]
Other animals
[edit]Primatescan also rarely experience pre-eclampsia.[105]In 2024, a femalewestern lowland gorillawas diagnosed with pre-eclampsia and had a successfulcaesarean section.[106]
References
[edit]- ^abcdefEiland E, Nzerue C, Faulkner M (2012)."Preeclampsia 2012".Journal of Pregnancy.2012:586578.doi:10.1155/2012/586578.PMC3403177.PMID22848831.
- ^abcdefghijklmnoAl-Jameil N, Aziz Khan F, Fareed Khan M, Tabassum H (February 2014)."A brief overview of preeclampsia".Journal of Clinical Medicine Research.6(1): 1–7.doi:10.4021/jocmr1682w.PMC3881982.PMID24400024.
- ^abcdefghijklm"Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists' Task Force on Hypertension in Pregnancy"(PDF).Obstetrics and Gynecology.122(5): 1122–1131. November 2013.doi:10.1097/01.AOG.0000437382.03963.88.PMC1126958.PMID24150027.Archived(PDF)from the original on 2016-01-06.Retrieved2015-02-17.
- ^abcdefghijklmnopqrstWHO recommendations for prevention and treatment of pre-eclampsia and eclampsia.World Health Organization. 2011.hdl:10665/44703.ISBN978-92-4-154833-5.Archived(PDF)from the original on 2015-05-13.
- ^abHenderson JT, Whitlock EP, O'Connor E, Senger CA, Thompson JH, Rowland MG (May 2014). "Low-dose aspirin for prevention of morbidity and mortality from preeclampsia: a systematic evidence review for the U.S. Preventive Services Task Force".Annals of Internal Medicine.160(10): 695–703.doi:10.7326/M13-2844.PMID24711050.S2CID33835367.
- ^abcdefghijklmnoArulkumaran N, Lightstone L (December 2013). "Severe pre-eclampsia and hypertensive crises".Best Practice & Research. Clinical Obstetrics & Gynaecology.27(6): 877–884.doi:10.1016/j.bpobgyn.2013.07.003.PMID23962474.
- ^abWang H, et al. (GBD 2015 Mortality and Causes of Death Collaborators) (October 2016)."Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980–2015: a systematic analysis for the Global Burden of Disease Study 2015".Lancet.388(10053): 1459–1544.doi:10.1016/s0140-6736(16)31012-1.PMC5388903.PMID27733281.
- ^Phipps EA (1 May 2019)."Pre-eclampsia: pathogenesis, novel diagnostics and therapies".Nature Reviews Nephrology.15:275–289.doi:10.1038/s41581-019-0119-6– via PubMed.
- ^Hypertension in pregnancy.ACOG. 2013. p. 2.ISBN978-1-934984-28-4.Archived fromthe originalon 2016-11-18.Retrieved2016-11-17.
- ^abLambert G, Brichant JF, Hartstein G, Bonhomme V, Dewandre PY (2014). "Preeclampsia: an update".Acta Anaesthesiologica Belgica.65(4): 137–149.PMID25622379.
- ^abMagee LA, Nicolaides KH, von Dadelszen P (May 2022). Longo DL (ed.). "Preeclampsia".The New England Journal of Medicine.386(19): 1817–1832.doi:10.1056/NEJMra2109523.PMID35544388.S2CID248695137.
- ^abLaule CF, Odean EJ, Wing CR, Root KM, Towner KJ, Hamm CM, et al. (October 2019)."Role of B1 and B2 lymphocytes in placental ischemia-induced hypertension".American Journal of Physiology. Heart and Circulatory Physiology.317(4): H732–H742.doi:10.1152/ajpheart.00132.2019.PMC6843018.PMID31397167.
- ^abcdMartin N (2018-08-14)."Trusted Health Sites Spread Myths About a Deadly Pregnancy Complication".ProPublica.Lost Mothers. Archived fromthe originalon 2021-05-15.Retrieved2021-05-28.
From the Mayo Clinic to Harvard, sources don't always get the facts right about preeclampsia. Reached by ProPublica, some are making needed corrections.
- ^Martin N, Montagne R (2017-05-12)."The Last Person You'd Expect to Die in Childbirth".ProPublica.Lost Mothers. Archived fromthe originalon 2019-06-21.Retrieved2021-05-28.
The death of Lauren Bloomstein, a neonatal nurse, in the hospital where she worked illustrates a profound disparity: The health care system focuses on babies but often ignores their mothers.
- ^abcdefghijklmnopqSteegers EA, von Dadelszen P, Duvekot JJ, Pijnenborg R (August 2010). "Pre-eclampsia".Lancet.376(9741): 631–644.doi:10.1016/S0140-6736(10)60279-6.PMID20598363.S2CID208792631.
- ^abBibbins-Domingo K, Grossman DC, Curry SJ, Barry MJ, Davidson KW, Doubeni CA, et al. (April 2017). "Screening for Preeclampsia: US Preventive Services Task Force Recommendation Statement".JAMA.317(16): 1661–1667.doi:10.1001/jama.2017.3439.PMID28444286.S2CID205091250.
- ^Ananth CV, Keyes KM, Wapner RJ (November 2013)."Pre-eclampsia rates in the United States, 1980–2010: age-period-cohort analysis".BMJ.347(nov07 15): f6564.doi:10.1136/bmj.f6564.PMC3898425.PMID24201165.
- ^Brown MC, Best KE, Pearce MS, Waugh J, Robson SC, Bell R (January 2013). "Cardiovascular disease risk in women with pre-eclampsia: systematic review and meta-analysis".European Journal of Epidemiology.28(1): 1–19.doi:10.1007/s10654-013-9762-6.PMID23397514.S2CID13239431.
- ^Innes KE, Byers TE (November 1999)."Preeclampsia and breast cancer risk".Epidemiology.10(6): 722–732.doi:10.1097/00001648-199911000-00013.JSTOR3703514.PMID10535787.
- ^abMohler ER (2006).Advanced Therapy in Hypertension and Vascular Disease.PMPH-USA. pp. 407–408.ISBN978-1-55009-318-6.Archivedfrom the original on 2015-10-05.
- ^"Toxemia of pregnancy | medical disorder".Encyclopedia Britannica.Archivedfrom the original on 2014-03-28.Retrieved2013-06-28.
- ^Brown MA, Lindheimer MD, de Swiet M, Van Assche A, Moutquin JM (January 2001)."The classification and diagnosis of the hypertensive disorders of pregnancy: statement from the International Society for the Study of Hypertension in Pregnancy (ISSHP)".Hypertension in Pregnancy.20(1): IX–XIV.doi:10.3109/10641950109152635.PMID12044323.S2CID45149920.
- ^"Pre-eclampsia".Mayo Clinic.Retrieved21 January2021.
- ^Wu J, Ren C, Delfino RJ, Chung J, Wilhelm M, Ritz B (November 2009)."Association between local traffic-generated air pollution and preeclampsia and preterm delivery in the south coast air basin of California"(PDF).Environmental Health Perspectives.117(11): 1773–1779.doi:10.1289/ehp.0800334.PMC2801174.PMID20049131.Archived fromthe original(PDF)on 2009-07-19.Retrieved2009-07-05.
- ^Bramham K, Parnell B, Nelson-Piercy C, Seed PT, Poston L, Chappell LC (April 2014)."Chronic hypertension and pregnancy outcomes: systematic review and meta-analysis".BMJ.348:g2301.doi:10.1136/bmj.g2301.PMC3988319.PMID24735917.
- ^abcdefghijklmnMustafa R, Ahmed S, Gupta A, Venuto RC (2012)."A comprehensive review of hypertension in pregnancy".Journal of Pregnancy.2012:105918.doi:10.1155/2012/105918.PMC3366228.PMID22685661.
- ^Staff AC (September 2019). "The two-stage placental model of preeclampsia: An update".Journal of Reproductive Immunology.134–135: 1–10.doi:10.1016/j.jri.2019.07.004.hdl:10852/78065.PMID31301487.S2CID196458745.
- ^abcdeChen DB, Wang W (May 2013)."Human placental microRNAs and preeclampsia".Biology of Reproduction.88(5): 130.doi:10.1095/biolreprod.113.107805.PMC4013914.PMID23575145.
- ^abOuyang Y, Mouillet JF, Coyne CB, Sadovsky Y (February 2014)."Review: placenta-specific microRNAs in exosomes - good things come in nano-packages".Placenta.3(Suppl): S69–S73.doi:10.1016/j.placenta.2013.11.002.PMC3944048.PMID24280233.
- ^abXie L, Mouillet JF, Chu T, Parks WT, Sadovsky E, Knöfler M, Sadovsky Y (December 2014)."C19MC microRNAs regulate the migration of human trophoblasts".Endocrinology.155(12): 4975–4985.doi:10.1210/en.2014-1501.PMC4239420.PMID25211593.
- ^abSkjaerven R, Vatten LJ, Wilcox AJ, Rønning T, Irgens LM, Lie RT (October 2005)."Recurrence of pre-eclampsia across generations: exploring fetal and maternal genetic components in a population based cohort".BMJ.331(7521): 877.doi:10.1136/bmj.38555.462685.8F.PMC1255793.PMID16169871.
- ^abEhret G (August 2018)."Genes for Preeclampsia: An Opportunity for Blood Pressure Genomics".Hypertension.72(2): 285–286.doi:10.1161/HYPERTENSIONAHA.118.10840.PMC6397719.PMID29967038.
- ^abPhipps EA, Thadhani R, Benzing T, Karumanchi SA (May 2019)."Pre-eclampsia: pathogenesis, novel diagnostics and therapies".Nature Reviews. Nephrology.15(5): 275–289.doi:10.1038/s41581-019-0119-6.PMC6472952.PMID30792480.
- ^abMcGinnis R, Steinthorsdottir V, Williams NO, Thorleifsson G, Shooter S, Hjartardottir S, et al. (August 2017)."Variants in the fetal genome near FLT1 are associated with risk of preeclampsia"(PDF).Nature Genetics.49(8): 1255–1260.doi:10.1038/ng.3895.hdl:2381/40488.PMID28628106.S2CID205354725.
- ^abSteinthorsdottir V, McGinnis R, Williams NO, Stefansdottir L, Thorleifsson G, Shooter S, et al. (November 2020)."Genetic predisposition to hypertension is associated with preeclampsia in European and Central Asian women".Nature Communications.11(1): 5976.doi:10.1038/s41467-020-19733-6.PMC7688949.PMID33239696.
- ^Maynard SE, Venkatesha S, Thadhani R, Karumanchi SA (May 2005)."Soluble Fms-like tyrosine kinase 1 and endothelial dysfunction in the pathogenesis of preeclampsia".Pediatric Research.57(5 Pt 2): 1R–7R.doi:10.1203/01.PDR.0000159567.85157.B7.PMID15817508.
- ^Chen CP (March 2009)."Placental abnormalities and preeclampsia in trisomy 13 pregnancies".Taiwanese Journal of Obstetrics & Gynecology.48(1): 3–8.doi:10.1016/S1028-4559(09)60028-0.PMID19346185.
- ^"GRCh38".Ensembl release 89.May 2017.
- ^Zadora J, Singh M, Herse F, Przybyl L, Haase N, Golic M, et al. (November 2017)."Disturbed Placental Imprinting in Preeclampsia Leads to Altered Expression of DLX5, a Human-Specific Early Trophoblast Marker".Circulation.136(19): 1824–1839.doi:10.1161/CIRCULATIONAHA.117.028110.PMC5671803.PMID28904069.
- ^Bounds KR, Chiasson VL, Pan LJ, Gupta S, Chatterjee P (September 2017)."MicroRNAs: New Players in the Pathobiology of Preeclampsia".Frontiers in Cardiovascular Medicine.4:60.doi:10.3389/fcvm.2017.00060.PMC5622156.PMID28993808.
- ^abcdCunningham FG, Leveno KJ, Bloom S, Gilstrap L, eds. (2010).Williams obstetrics(23rd ed.). New York: McGraw-Hill Medical.ISBN978-0-07-149701-5.
- ^abcdefBartsch E, Medcalf KE, Park AL, Ray JG (April 2016)."Clinical risk factors for pre-eclampsia determined in early pregnancy: systematic review and meta-analysis of large cohort studies".BMJ.353:i1753.doi:10.1136/bmj.i1753.PMC4837230.PMID27094586.
- ^Berlac JF, Hartwell D, Skovlund CW, Langhoff-Roos J, Lidegaard Ø (June 2017). "Endometriosis increases the risk of obstetrical and neonatal complications".Acta Obstetricia et Gynecologica Scandinavica.96(6): 751–760.doi:10.1111/aogs.13111.PMID28181672.
- ^Garg AX, Nevis IF, McArthur E, Sontrop JM, Koval JJ, Lam NN, et al. (January 2015)."Gestational hypertension and preeclampsia in living kidney donors".The New England Journal of Medicine.372(2): 124–133.doi:10.1056/NEJMoa1408932.PMC4362716.PMID25397608.
- ^van den Boogaard E, Vissenberg R, Land JA, van Wely M, van der Post JA, Goddijn M, Bisschop PH (2011)."Significance of (sub)clinical thyroid dysfunction and thyroid autoimmunity before conception and in early pregnancy: a systematic review".Human Reproduction Update(Review).17(5): 605–619.doi:10.1093/humupd/dmr024.PMID21622978.
- ^Vissenberg R, van den Boogaard E, van Wely M, van der Post JA, Fliers E, Bisschop PH, Goddijn M (July 2012)."Treatment of thyroid disorders before conception and in early pregnancy: a systematic review".Human Reproduction Update(Review).18(4): 360–373.doi:10.1093/humupd/dms007.PMID22431565.
- ^Drife JO, Magowan B (2004).Clinical obstetrics and gynecology.Edinburgh, New York: Saunders. pp.367–70.ISBN978-0-7020-1775-9.
- ^McMaster-Fay RA (2008). "Pre-eclampsia: a disease of oxidative stress resulting from the catabolism of DNA (primarily fetal) to uric acid by xanthine oxidase in the maternal liver; a hypothesis".Bioscience Hypotheses.1:35–43.doi:10.1016/j.bihy.2008.01.002.
- ^abcLaresgoiti-Servitje E, Gómez-López N, Olson DM (April 2010)."An immunological insight into the origins of pre-eclampsia".Human Reproduction Update.16(5): 510–524.doi:10.1093/humupd/dmq007.PMID20388637.
- ^abcdeRedman CW, Sargent IL (June 2005). "Latest advances in understanding preeclampsia".Science.308(5728): 1592–1594.Bibcode:2005Sci...308.1592R.doi:10.1126/science.1111726.PMID15947178.S2CID21889468.
- ^abcdDavis JA, Gallup GG (2006). "Preeclampsia and other pregnancy complications as an adaptive response to unfamiliar semen)". In Platek SM, Shackelford TK (eds.).Female Infidelity and Paternal Uncertainty. Evolutionary Perspectives on Male Anti-Cuckoldry Tactics.Cambridge University Press. pp.191–204.doi:10.1017/CBO9780511617812.010.ISBN978-0-511-61781-2.
- ^Fu ZM, Ma ZZ, Liu GJ, Wang LL, Guo Y (January 2018)."Vitamins supplementation affects the onset of preeclampsia".Journal of the Formosan Medical Association = Taiwan Yi Zhi.117(1): 6–13.doi:10.1016/j.jfma.2017.08.005.hdl:10654/41911.PMID28877853.
- ^Matthiesen L, Berg G, Ernerudh J, Ekerfelt C, Jonsson Y, Sharma S (2005). "Immunology of preeclampsia".Chemical Immunology and Allergy.89:49–61.doi:10.1159/000087912.ISBN978-3-8055-7970-4.PMID16129952.
- ^abcLongo DL (2012).Harrison's principles of internal medicine.New York: McGraw-Hill. pp. 55–61.ISBN978-0-07-174889-6.
- ^abRolnik DL, Wright D, Poon LC, Syngelaki A, O'Gorman N, de Paco Matallana C, et al. (October 2017)."ASPRE trial: performance of screening for preterm pre-eclampsia".Ultrasound in Obstetrics & Gynecology.50(4): 492–495.doi:10.1002/uog.18816.hdl:2434/559777.PMID28741785.S2CID24728853.
- ^Poon LC, Shennan A, Hyett JA, Kapur A, Hadar E, Divakar H, et al. (May 2019)."The International Federation of Gynecology and Obstetrics (FIGO) initiative on pre-eclampsia: A pragmatic guide for first-trimester screening and prevention".International Journal of Gynaecology and Obstetrics.145(Suppl 1): 1–33.doi:10.1002/ijgo.12802.PMC6944283.PMID31111484.
- ^Gallo DM, Wright D, Casanova C, Campanero M, Nicolaides KH (May 2016)."Competing risks model in screening for preeclampsia by maternal factors and biomarkers at 19-24 weeks' gestation".American Journal of Obstetrics and Gynecology.214(5): 619.e1–619.e17.doi:10.1016/j.ajog.2015.11.016.PMID26627730.
- ^Zeisler H, Llurba E, Chantraine F, Vatish M, Staff AC, Sennström M, et al. (January 2016)."Predictive Value of the sFlt-1:PlGF Ratio in Women with Suspected Preeclampsia".The New England Journal of Medicine.374(1): 13–22.doi:10.1056/NEJMoa1414838.PMID26735990.
- ^Craici IM, Wagner SJ, Bailey KR, Fitz-Gibbon PD, Wood-Wentz CM, Turner ST, et al. (June 2013)."Podocyturia predates proteinuria and clinical features of preeclampsia: longitudinal prospective study".Hypertension.61(6): 1289–1296.doi:10.1161/HYPERTENSIONAHA.113.01115.PMC3713793.PMID23529165.
- ^"Pre-eclampsia predicted using test during pregnancy".BBC News.2011-11-12.Archivedfrom the original on 2011-11-18.Retrieved2011-11-22.
- ^Brown CM, Garovic VD (October 2011)."Mechanisms and management of hypertension in pregnant women".Current Hypertension Reports.13(5): 338–346.doi:10.1007/s11906-011-0214-y.PMC3746761.PMID21656283.
- ^"Pre-eclampsia-Eclampsia".Diagnosis and management of pre-eclampsia and eclampsia.Armenian Medical Network. 2003.Retrieved2005-11-23.
- ^Ota E, Hori H, Mori R, Tobe-Gai R, Farrar D (June 2015). "Antenatal dietary education and supplementation to increase energy and protein intake".The Cochrane Database of Systematic Reviews.2015(6): CD000032.doi:10.1002/14651858.CD000032.pub3.PMID26031211.
- ^Duley L, Henderson-Smart D, Meher S (October 2005)."Altered dietary salt for preventing pre-eclampsia, and its complications".The Cochrane Database of Systematic Reviews.2012(4): CD005548.doi:10.1002/14651858.CD005548.PMC11270530.PMID16235411.S2CID21173116.
- ^Rumbold AR, Crowther CA, Haslam RR, Dekker GA, Robinson JS (April 2006). "Vitamins C and E and the risks of preeclampsia and perinatal complications".The New England Journal of Medicine.354(17): 1796–1806.doi:10.1056/NEJMoa054186.hdl:2440/23161.PMID16641396.
- ^abcdWHO recommendations for prevention and treatment of pre-eclampsia and eclampsia.2011.ISBN978-92-4-154833-5.
- ^Hofmeyr GJ, Lawrie TA, Atallah ÁN, Torloni MR (October 2018)."Calcium supplementation during pregnancy for preventing hypertensive disorders and related problems".The Cochrane Database of Systematic Reviews.2018(10): CD001059.doi:10.1002/14651858.CD001059.pub5.PMC6517256.PMID30277579.
- ^Rayman MP, Bode P, Redman CW (November 2003)."Low selenium status is associated with the occurrence of the pregnancy disease preeclampsia in women from the United Kingdom"(PDF).American Journal of Obstetrics and Gynecology.189(5): 1343–1349.doi:10.1067/S0002-9378(03)00723-3.PMID14634566.Archived(PDF)from the original on 2018-07-20.Retrieved2019-06-30.
- ^abLiu T, Zhang M, Guallar E, Wang G, Hong X, Wang X, Mueller NT (August 2019)."Trace Minerals, Heavy Metals, and Preeclampsia: Findings from the Boston Birth Cohort".Journal of the American Heart Association.8(16): e012436.doi:10.1161/JAHA.119.012436.PMC6759885.PMID31426704.
- ^Duley L, Meher S, Hunter KE, Seidler AL, Askie LM (October 2019)."Antiplatelet agents for preventing pre-eclampsia and its complications".The Cochrane Database of Systematic Reviews.2019(10).doi:10.1002/14651858.CD004659.pub3.PMC6820858.PMID31684684.
- ^"Low-Dose Aspirin Use for the Prevention of Morbidity and Mortality From Preeclampsia".United States Preventive Services Task Force. September 2014. Archived fromthe originalon 17 September 2014.Retrieved17 September2014.
- ^Roberge S, Nicolaides K, Demers S, Hyett J, Chaillet N, Bujold E (February 2017). "The role of aspirin dose on the prevention of preeclampsia and fetal growth restriction: systematic review and meta-analysis".American Journal of Obstetrics and Gynecology.216(2): 110–120.e6.doi:10.1016/j.ajog.2016.09.076.PMID27640943.S2CID3079979.
- ^abcWalsh SW, Strauss JF (June 2021)."The Road to Low-Dose Aspirin Therapy for the Prevention of Preeclampsia Began with the Placenta".International Journal of Molecular Sciences.22(13): 6985.doi:10.3390/ijms22136985.PMC8268135.PMID34209594.
- ^Meher S, Duley L (April 2006). Meher S (ed.)."Exercise or other physical activity for preventing pre-eclampsia and its complications".The Cochrane Database of Systematic Reviews.2006(2): CD005942.doi:10.1002/14651858.CD005942.PMC8900135.PMID16625645.
- ^Meher S, Duley L (April 2006). Meher S (ed.)."Rest during pregnancy for preventing pre-eclampsia and its complications in women with normal blood pressure".The Cochrane Database of Systematic Reviews.2006(2): CD005939.doi:10.1002/14651858.CD005939.PMC6823233.PMID16625644.
- ^Jeyabalan A, Powers RW, Durica AR, Harger GF, Roberts JM, Ness RB (August 2008)."Cigarette smoke exposure and angiogenic factors in pregnancy and preeclampsia".American Journal of Hypertension.21(8): 943–947.doi:10.1038/ajh.2008.219.PMC2613772.PMID18566591.
- ^Whitworth M, Dowswell T (October 2009)."Routine pre-pregnancy health promotion for improving pregnancy outcomes".The Cochrane Database of Systematic Reviews(4): CD007536.doi:10.1002/14651858.CD007536.pub2.PMC4164828.PMID19821424.
- ^abcRobertson SA, Bromfield JJ, Tremellen KP (August 2003). "Seminal 'priming' for protection from pre-eclampsia-a unifying hypothesis".Journal of Reproductive Immunology.59(2): 253–265.doi:10.1016/S0165-0378(03)00052-4.PMID12896827.
- ^abDekker GA, Robillard PY, Hulsey TC (June 1998). "Immune maladaptation in the etiology of preeclampsia: a review of corroborative epidemiologic studies".Obstetrical & Gynecological Survey.53(6): 377–382.doi:10.1097/00006254-199806000-00023.PMID9618714.
- ^abBonney EA (December 2007)."Preeclampsia: a view through the danger model".Journal of Reproductive Immunology.76(1–2): 68–74.doi:10.1016/j.jri.2007.03.006.PMC2246056.PMID17482268.
- ^Mattar R, Soares RV, Daher S (February 2005). "Sexual behavior and recurrent spontaneous abortion".International Journal of Gynaecology and Obstetrics.88(2): 154–155.doi:10.1016/j.ijgo.2004.11.006.PMID15694097.S2CID37475639.
- ^Dekker G (2002). "The partner's role in the etiology of preeclampsia".Journal of Reproductive Immunology.57(1–2): 203–215.doi:10.1016/S0165-0378(02)00039-6.PMID12385843.
- ^Beckmann CR, Ling FW, Smith RP, Barzansky BM, Herbert WN, Laube DW, American Congress of Obstetricians and Gynecologists, eds. (2010).Obstetrics and gynecology(6th ed.). Baltimore, MD: Lippincott Williams & Wilkins.ISBN978-0-7817-8807-6.[page needed]
- ^McCall CA, Grimes DA, Lyerly AD (June 2013). "'Therapeutic' bed rest in pregnancy: unethical and unsupported by data ".Obstetrics and Gynecology.121(6): 1305–1308.doi:10.1097/aog.0b013e318293f12f.PMID23812466.S2CID9069311.
- ^Hypertensive Disorders in Pregnancy. Version 2.0.Archived2016-03-06 at theWayback Machineat Nederlandse Vereniging voor Obstetrie en Gynaecologie. Date of approval: 20-05-2005
- ^World Health Organization (WHO). World health report 2005: make every mother and child count. Geneva: WHO; 2005, p. 63
- ^Robbins and Cotran,Pathological Basis of Disease, 7th ed.
- ^Keyes LE, Armaza JF, Niermeyer S, Vargas E, Young DA, Moore LG (July 2003)."Intrauterine growth restriction, preeclampsia, and intrauterine mortality at high altitude in Bolivia".Pediatric Research.54(1): 20–25.doi:10.1203/01.PDR.0000069846.64389.DC.PMID12700368.S2CID25586771.
- ^Moore LG, Shriver M, Bemis L, Hickler B, Wilson M, Brutsaert T, et al. (April 2004)."Maternal adaptation to high-altitude pregnancy: an experiment of nature – a review"(PDF).Placenta.25(Suppl A): S60–S71.doi:10.1016/j.placenta.2004.01.008.PMID15033310.Archived fromthe original(PDF)on 2016-08-17.Retrieved2016-06-14.
- ^Urquia ML, Glazier RH, Gagnon AJ, Mortensen LH, Nybo Andersen AM, Janevic T, et al. (November 2014)."Disparities in pre-eclampsia and eclampsia among immigrant women giving birth in six industrialised countries".BJOG.121(12): 1492–1500.doi:10.1111/1471-0528.12758.PMC4232918.PMID24758368.
- ^Martin N, Montagne R (2017-12-07)."Nothing Protects Black Women From Dying in Pregnancy and Childbirth".ProPublica.Lost Mothers. Archived fromthe originalon 2021-05-05.Retrieved2021-05-28.
Not education. Not income. Not even being an expert on racial disparities in health care.
- ^Hjartardottir S, Leifsson BG, Geirsson RT, Steinthorsdottir V (2004). "Paternity change and the recurrence risk in familial hypertensive disorder in pregnancy".Hypertension in Pregnancy.23(2): 219–225.doi:10.1081/PRG-120037889.PMID15369654.S2CID8936562.
- ^Anthony J, Damasceno A, Ojjii D (2016-05-18)."Hypertensive disorders of pregnancy: what the physician needs to know".Cardiovascular Journal of Africa.27(2): 104–110.doi:10.5830/CVJA-2016-051.PMC4928160.PMID27213858.
- ^abMcDonald SD, Malinowski A, Zhou Q, Yusuf S, Devereaux PJ (November 2008). "Cardiovascular sequelae of preeclampsia/eclampsia: a systematic review and meta-analyses".American Heart Journal.156(5): 918–930.doi:10.1016/j.ahj.2008.06.042.PMID19061708.
- ^abBellamy L, Casas JP, Hingorani AD, Williams DJ (November 2007)."Pre-eclampsia and risk of cardiovascular disease and cancer in later life: systematic review and meta-analysis".BMJ.335(7627): 974.doi:10.1136/bmj.39335.385301.BE.PMC2072042.PMID17975258.
- ^Mostello D, Catlin TK, Roman L, Holcomb WL, Leet T (August 2002). "Preeclampsia in the parous woman: who is at risk?".American Journal of Obstetrics and Gynecology.187(2): 425–429.doi:10.1067/mob.2002.123608.PMID12193937.
- ^Barker DJ (July 1995)."Fetal origins of coronary heart disease".BMJ.311(6998): 171–174.doi:10.1136/bmj.311.6998.171.PMC2550226.PMID7613432.
- ^Sharma D, Shastri S, Sharma P (2016)."Intrauterine Growth Restriction: Antenatal and Postnatal Aspects".Clinical Medicine Insights. Pediatrics.10:67–83.doi:10.4137/CMPed.S40070.PMC4946587.PMID27441006.
- ^Calkins K, Devaskar SU (July 2011)."Fetal origins of adult disease".Current Problems in Pediatric and Adolescent Health Care.41(6): 158–176.doi:10.1016/j.cppeds.2011.01.001.PMC4608552.PMID21684471.
- ^Wikström AK, Svensson T, Kieler H, Cnattingius S (November 2011)."Recurrence of placental dysfunction disorders across generations".American Journal of Obstetrics and Gynecology.205(5): 454.e1–454.e8.doi:10.1016/j.ajog.2011.05.009.PMID21722870.
- ^abHauspurg A, Jeyabalan A (February 2022)."Postpartum preeclampsia or eclampsia: defining its place and management among the hypertensive disorders of pregnancy".American Journal of Obstetrics and Gynecology.226(2S): S1211–S1221.doi:10.1016/j.ajog.2020.10.027.PMC8857508.PMID35177218.
- ^Redman EK, Hauspurg A, Hubel CA, Roberts JM, Jeyabalan A (November 2019)."Clinical Course, Associated Factors, and Blood Pressure Profile of Delayed-Onset Postpartum Preeclampsia".Obstetrics and Gynecology.134(5): 995–1001.doi:10.1097/AOG.0000000000003508.PMC6922052.PMID31599846.
- ^abcSteele DW, Adam GP, Saldanha IJ, Kanaan G, Zahradnik ML, Danilack VA, Stuebe AM, Peahl AF, Chen KK, Balk EM (2023-05-31).Management of Postpartum Hypertensive Disorders of Pregnancy(Report). Agency for Healthcare Research and Quality (AHRQ).doi:10.23970/ahrqepccer263.
- ^Beardmore KS, Morris JM, Gallery ED (January 2002). "Excretion of antihypertensive medication into human breast milk: a systematic review".Hypertension in Pregnancy.21(1): 85–95.doi:10.1081/PRG-120002912.PMID12044345.
- ^Conrad K (2008)."Animal models of pre-eclampsia: do they exist?".Fetal and Maternal Medicine Review.2(1): 67.doi:10.1017/S0965539500000267.Retrieved18 February2024.
- ^Yousef N (17 February 2024)."Texas zoo delivers baby gorilla via caesarean section".BBC News.Retrieved18 February2024.
